 |
 |
- Search
| Neurospine > Volume 17(Suppl 1); 2020 > Article |
|
|

See commentary "Why Should We Perform Endoscopic Spine Surgery?" in Volume 17 on page S13.
Abstract
Biportal endoscopic transforaminal lumbar interbody fusion (TLIF) may have advantages of minimally invasive fusion surgery as well as those of endoscopic surgery. The purpose of this study was to present the biportal endoscopic TLIF technique along with video presentations and a review of the literature on this technique. Basically, the biportal endoscopic TLIF technique is similar to minimally invasive TLIF with a tubular retractor. There were 2 options in the biportal endoscopic TLIF procedures. The first was the insertion of one long TLIF cage and the other was the insertion of 2 short posterior lumbar interbody fusion (PLIF) cages. After the interbody fusion procedures, percutaneous pedicles screw fixation was performed. Biportal endoscopic TLIF achieved complete neural decompression through laminectomy and facetectomy like conventional TLIF. Endplate preparation was performed completely under a clear and magnified endoscopic view. It was also feasible to insert a large TLIF cage or 2 cages for PLIF without exiting nerve root injury. Biportal endoscopic TLIF might have the advantages of endoscopic surgery as well as minimally invasive fusion surgery. Direct neural decompression, endplate preparation under endoscopic guidance, and the insertion of a large TLIF cage or 2 PLIF cages may be the merits of biportal endoscopic lumbar fusion procedures.
Minimally invasive (MIS) spine surgery has the advantages of early recovery and the preservation of normal structures.1 MIS spine procedures include percutaneous pain procedures, endoscopic spine surgery, microsurgery with tubular retractor systems, lateral lumbar interbody fusion surgeries, and transforaminal lumbar interbody fusion (TLIF) surgeries [1]. Recently, endoscopic lumbar interbody fusion procedures have been attempted for lumbar degenerative disease and instability [2-6]. Regarding the instrumentation systems, there are 2 kinds of endoscopic lumbar interbody fusion surgeries. The first is uniportal endoscopic lumbar interbody fusion and the other is biportal endoscopic lumbar interbody fusion.5,6 With regard to surgical approaches or corridor, one approach is a trans-Kambin approach using uniportal endoscopic surgery [6-10] and the other is a posterolateral approach like MIS TLIF using uniportal or biportal endoscopic surgery [5,11,12]. The trans-Kambin approach is similar to transforaminal endoscopic lumbar discectomy via the Kambin triangle. And, the technique of posterolateral endoscopic TLIF is similar to MIS TLIF involving tubular retractor systems [4,5,12].
Although endoscopic TLIF by the trans-Kambin approach may be less invasive than the posterolateral approach, the transKambin approach might exhibit a higher possibility of exiting nerve root irritation or injury and limitations in direct neural decompression compared to the posterolateral approach [7,13]. The biportal endoscopic TLIF technique uses a posterolateral approach similar to MIS TLIF involving tubular retractor systems. Through biportal endoscopic procedures, it was feasible to perform direct neural decompression through a laminectomy, contralateral sublaminar decompression, discectomy, foraminotomy, and facetectomy as well as indirect decompression by disc space restoration, and the reduction of spondylolisthesis [4,5,11,14-16]. Also, the endoscopic approach is the least invasive and may preserve the normal structure [6,17]. Biportal endoscopic TLIF is hypothesized to have advantages of minimally invasive fusion surgery as well as those of endoscopic surgery [5,11]. Herein, we present the biportal endoscopic TLIF technique along with a video presentation and review of the literature on this technique.
We present 2 illustrated cases with surgical videos. The lumbar interbody fusion procedures were performed by biportal endoscopic surgery [5,11,18] (Fig. 1). There were 2 options of biportal endoscopic lumbar interbody fusion surgical procedures performed. The first was a cage insertion procedure (Supplementary video clip 1) and the second was a 2-cage insertion procedure (Supplementary video clip 2).
The biportal endoscopy systems include a console, camera, endoscopy irrigation equipment, and tool kits, which are essential for the surgery. A waterproof surgical drape is essential for endoscopic spine surgeries and must be prepared. Also, a radiofrequency (RF) console and RF probes should be prepared for tissue cauterization and bleeding control. General spinal operation instruments for MIS TLIF were used. Angled curettes are helpful for endplate preparation of the contralateral side. A long straight TLIF cage (width, 11 mm; length, 34 mm; height, 9–18 mm) was usually used for interbody fusion, and short-length PLIF cages (width, 11 mm; length, 25 mm; height, 9–18 mm) are available. After the interbody fusion procedures, percutaneous pedicle screws were inserted under C-arm fluoroscopic guidance.
We prefer general endotracheal anesthesia. Epidural anesthesia with intravenous sedation is also available for single-level fusion. The patient is in a prone position during the interbody fusion procedure and insertion of the percutaneous pedicle screws. A Jackson table or a Wilson frame is used for this procedure.
First, we make 2 skin incisions over the ipsilateral pedicles for decompression and insertion of the cages under C-arm fluoroscopic guidance (Fig. 2). If the dominant radicular pain site was in the leg or buttock, biportal endoscopic approaches are tried at the dominant pain side. Modified skin incisions, different from routine incisions, were used. Typically, a 5-mm-long skin incision for an endoscopic portal is made close to the disc space of the medial pedicular line and the other skin incision is made on the working portal over the pedicle (Fig. 2B). These 2 skin incisions are also used for ipsilateral percutaneous pedicle screw insertion. A small-sized endoscopic portal is used for passing a drainage catheter. The purpose of the modified skin incision is to achieve optimal visualization of the superior and inferior endplates during endplate preparation.
Serial dilators are inserted through the working portals. The lower portion of the cranial lamina is gently dissected using a dissector under C-arm fluoroscopic guidance. The docking point of the endoscopic and working portals is over the lower portion of the cranial lamina. Ipsilateral unilateral laminotomy with an ipsilateral facetectomy is performed. Ipsilateral laminotomy of the upper and lower laminae is performed until full exposure of the ligamentum flavum from the proximal end to the distal end. The unilateral inferior articular process is removed using Kerrison punches and osteotomes. The superior articular process is partially removed. In cases with foraminal stenosis or foraminal disc herniation, the superior articular process is removed for decompression of the exiting nerve root. Facet and laminae bone chips are collected for fusion materials.
The ligamentum flavum is removed for ipsilateral traversing nerve root decompression (Fig. 3A). The contralateral side of the ligamentum flavum is completely removed for decompression of the central canal and contralateral traversing nerve root (Fig. 3B, C). The medial portion of the contralateral facet joint is fully released for the reduction of spondylolisthesis or distraction of the intervertebral disc space. Annulus fibrosus of the disc is incised using a blunt knife or an RF probe with a small diameter. The disc materials are removed using pituitary forceps and shavers. We perform complete endplate preparation under the endoscopic view. A small-diameter shaver is inserted and rotated in disc space. Larger shavers are used serially for endplate preparation. The endoscopy of biportal endoscopic systems can be inserted into disc space. The dissection plane between the cartilaginous endplate and osseous endplate is explored under a clear, magnified endoscopic view. The cartilaginous endplate is separated from the osseous endplate using angled dissectors and curettes (Fig. 4A). Only the cartilaginous endplate can be completely removed from the osseous endplate under a clear endoscopic view (Fig. 4B). The intervertebral disc space is distracted by serial insertion of cage trials or serial dilators. The contralateral side of endplate is prepared using angled curettes and an upward angled pituitary. For good visualization of the contralateral endplate, a 30° endoscopy is used. Sometimes we change the endoscopy from 0° to 30°. After confirmation of complete endplate preparation under endoscopic view, allogenous or autogenous bone chips are inserted using a specialized funnel under C-arm fluoroscopic guidance (Fig. 5A, B). Continuous saline irrigation is stopped during the insertion of fusion materials.
Finally, a long TLIF cage is inserted through the working portal after dura retraction. C-arm fluoroscopy was used during cage insertion. The cage is repositioned obliquely or transversely using a cage pusher device. If we use short PLIF cages, we usually put in 2 cages for interbody fusion. The first cage is obliquely and deeply inserted into the midline or contralateral side. After insertion of the first cage, the second short cage is inserted. The specialized dura retractor is deeply inserted for protection, covering the dura as well as the first inserted cage. Since the remnant of the superior articular process can protect the exiting nerve root during cage insertion, the ipsilateral exiting nerve root is decompressed after cage insertion. Finally, the exiting nerve root is additionally decompressed in cases with foraminal lesions with exiting root indentations. A drainage catheter is inserted to prevent postoperative epidural hematoma.
A 56-year-old female patient presented with back pain, claudication, and radicular pain in both the legs. The more painful side was the right leg. The preoperative magnetic resonance imaging (MRI) and x-ray images demonstrated degenerative spondylolisthesis with stenosis at L4–5 (Fig. 6). We performed biportal endoscopic TLIF of the L4–5 level. Biportal endoscopic TLIF was performed with the right approach. The postoperative MRI showed a reduction in spondylolisthesis and good decompression status of the central stenosis (Fig. 6). Postoperatively, the patient’s symptoms were significantly improved. (Supplementary video clip 1).
A 55-year-old female patient presented with radicular pain in both legs and neurological intermittent claudication. The preoperative MRI and x-ray images revealed degenerative spondylolisthesis with central and foraminal stenosis at L4–5 (Fig. 7). The patient underwent biportal endoscopic TLIF with a 2-cage insertion technique. The postoperative MRI and x-ray images demonstrated a significant reduction in spondylolisthesis and good decompression of the neural structures (Fig. 7). The pain was resolved after the biportal endoscopic TLIF. (Supplementary video clip 2).
Conceptually, this biportal endoscopic TLIF approach might have the advantages of both MIS fusion and endoscopic surgery. Theoretically, biportal endoscopic fusion surgeries may be suitable for endoscopic assistant fusion surgery. However, the term seems to be confused with air-based microendoscope-assisted fusion surgeries. Microendoscope-assisted TLIF was performed using tubular retractor systems. Therefore, we suggested that the term of endoscopic TLIF may be better than endoscope-assisted TLIF in the water-based endoscopic lumbar interbody fusion surgeries. This technique is based on conventional microscopic TLIF procedures [1]. Therefore, it is possible to achieve the direct decompression of neural tissue by biportal endoscopic TLIF [14,15], and insert large, long TLIF cages, like in MIS TLIF [4,5]. The contralateral nerve root could be fully decompressed through the contralateral sublaminar approach [4,14]. The contralateral sublaminar approach for contralateral nerve root decompression is one of the advantages of the biportal endoscopic approach [3,15]. Also, indirect decompression was achieved by the reduction of spondylolisthesis and the restoration of the collapsed disc space. Since we could insert a large, long cage for conventional TLIF, the narrowed disc space was distracted by the insertion of a large-sized cage [5].
The direct decompression of central canal and nerve roots was performed by removing the ligamentum flavum, and by laminectomy and facetectomy [5,14]. Since there was a possibility of exiting nerve root injury during insertion of a cage, we usually decompressed the ipsilateral exiting nerve root after a cage insertion. The lateral remnant of the superior articular process imparted protection to the exiting nerve root during cage insertion. If patients had severe foraminal stenosis or foraminal disc herniation, we performed direct foraminal decompression through a total facetectomy.
The distraction of narrowed disc space was important to cage insertion and for performing indirect decompression. The placement of serial dilators or cages trials into the disc space led to disc space distraction without endplate injury. It was further hypothesized that contralateral medial facet release may be important for the reduction of spondylolisthesis and the restoration of disc height. We performed contralateral facet release through complete removal of the contralateral ligamentum flavum around the facet joint and partial removal of the contralateral superior articular process. Some clinicians prefer to insert 2 cages rather than 1 cage. By using the biportal endoscopic approach, it is possible to insert 2 PLIF cages via a unilateral biportal endoscopic approach.
Two types of endoscopic lumbar interbody fusion surgeries can be used, depending on the surgical approaches (Fig. 8, Table 1). The first is the trans-Kambin approach (Fig. 8A) [6,7,13,19], and the other is a posterolateral approach (Fig. 8B) [2,4,11]. The trans-Kambin endoscopic TLIF procedure was performed via Kambin’s triangle, like fully endoscopic transforaminal lumbar discectomy. Endplate preparation and cage insertion were performed via Kambin’s triangle [6]. The posterolateral approach is similar to MIS TLIF surgery. The posterolateral endoscopic TLIF approach is based on MIS TLIF (Fig. 8B) [5,11,18]. Direct decompressive procedures, including ipsilateral laminotomy and total facetectomy, were performed in the posterolateral endoscopic TLIF approach. Although endoscopic TLIF through the trans-Kambin approach is less invasive than the posterolateral approach, the disadvantage of the trans-Kambin approach is exiting nerve root injury. Previous studies reported the frequency of exiting nerve irritation or injury from 0% to 22% in the trans-Kambin approach in uniportal endoscopic TLIF [7,19]. Since a cage is inserted through Kambin’s triangle, there might be a high possibility of exiting nerve root injury during insertion. Direct decompression and endplate preparation may also be limited in the trans-Kambin approach.
In contrast, the posterolateral approach might have a lower possibility of exiting nerve root injury during cage insertion. Before cage insertion, full neural decompression procedures were performed. Enough space for cage insertion was made through facetectomy and laminectomy. We could also achieve complete direct decompression of the central canal and nerve roots, like in MIS TLIF. We could place the cages safely during biportal endoscopic TLIF [5], This posterolateral approach was available in biportal or uniportal endoscopic systems [5].
Five articles on biportal endoscopic fusion surgeries have been published (Table 2) [2,4,5,11,18]. Two articles reported the technique and preliminary clinical results. These 2 articles focused on the technical aspect of biportal endoscopic TLIF [5,18]. Additionally, early favorable clinical outcomes were presented. Another 2 articles presented comparative studies of biportal endoscopic TLIF with conventional PLIF or TLIF surgeries [4,11]. Compared to conventional fusion surgeries or MIS fusion surgeries, the benefits of biportal endoscopic fusion were less blood loss and postoperative pain. These advantages of biportal endoscopic TLIF may lead to early recovery and early return to work after surgery. Moreover, the combination of biportal endoscopic fusion surgery with enhanced recovery after surgery programs might reduce complications and shorten hospital stays after surgery [4]. However, biportal endoscopic fusion surgeries were more difficult than conventional open surgery or microscopic surgery with a tubular retractor. A comparison of operation time may offer clues to the technical difficulty. The operation time for biportal endoscopic fusion surgeries was longer than that for conventional PLIF and TLIF surgeries [4,11]. Moreover, there were complications related to biportal endoscopic TLIF. Durotomy, postoperative epidural hematoma, infections, and nerve root palsy have been reported in previously published articles (Table 2) [2,4,5,11,18]. Although the reported complications related to biportal endoscopic TLIF were mainly minor, endoscopic fusion procedures are very difficult and have the possibility of major complications. Incomplete surgery may be another problem of endoscopic fusion surgeries. Therefore, we strongly recommend that endoscopic fusion surgeries should be tried after extensive experience with endoscopic surgeries, such as endoscopic decompression and endoscopic discectomy using uniportal or biportal endoscopy.
The last article was a review article about endoscopic TLIF, including biportal as well as uniportal endoscopic systems [2]. There were only short-term clinical outcomes of endoscopic TLIF and no randomized case-control studies of endoscopic lumbar fusions. Consequently, this review article was not able to conclude the advantages and superiority of endoscopic TLIF [2].
Compared with MIS TLIF, biportal endoscopic approaches may afford better endplate preparation. We could insert an endoscope into the intervertebral disc space during endplate preparation. It was possible to precisely demonstrate the condition of the endplate via endoscopy. The cartilaginous endplate was separated and removed from the osseous endplate under a magnified endoscopic view [4]. General instruments used for endplate preparation, such as an angled curette, box designed curette, and angled pituitary forceps, were available to perform complete endplate preparation under endoscopic guidance. Thirty-degree endoscopy and angled instruments may be useful for contralateral disc removal and endplate preparation. Endoscopy-guided endplate preparation may prevent osseous endplate injury during endplate preparation and subsidence of a cage. One of the important purposes of lumbar fusion surgery is the restoration of segmental lordosis. Since the biportal endoscopic TLIF technique achieved complete facetectomy and could accommodate the insertion of a large TLIF cage, this biportal endoscopic approach might be as good as MIS TLIF in restoring segmental lordosis.
Biportal endoscopic TLIF exhibited similarity with MIS TLIF with a tubular retractor and has several advantages of endoscopic approaches. However, a long-term follow-up study and randomized case-control studies should be performed.
Herein, we present the technique and literature review of biportal endoscopic TLIF. Biportal endoscopic TLIF might have the advantages of MIS fusion surgeries as well as those of the endoscopic approach. Direct decompression, endoscopically guided endplate preparation, and the insertion of large cages may be the merits of biportal endoscopic lumbar fusion procedures. To reveal the efficacy and clinical usefulness of the biportal technique, long-term blinded, randomized case-control studies are needed.
1. In the biportal endoscopic TLIF technique, direct decompression was first performed via unilateral laminotomy with bilateral decompression.
2. The inferior articular process, as well as the superior articular process, was removed for safe insertion of a large cage.
3. The cartilaginous endplate should be completely removed from the osseous endplate for interbody fusion under a magnified, clear endoscopic view. It was possible to demonstrate endplate conditions during the endplate preparation procedure via endoscopy.
4. A large volume of fusion materials, including auto-bone, allo-bone, and demineralization bone matrix, should be inserted via a funnel before insertion of the cage.
5. The release of the medial part of the contralateral facet joint may be helpful for disc space distraction and the reduction of spondylolisthesis.
6. Percutaneous pedicle screw insertion was subsequently performed after the interbody fusion procedures.
SUPPLEMENTARY MATERIALS
Supplementary video clip 1-3 can be found via https://doi.org/10.14245/ns.2040178.089.v.1 and https://doi.org/10.14245/ns.2040178.089.v.2.
Fig. 1.
Overview of biportal endoscopic lumbar interbody fusion. Usually, the dominant hand was used for the working portal and the nondominant hand was used for the endoscopic portal.
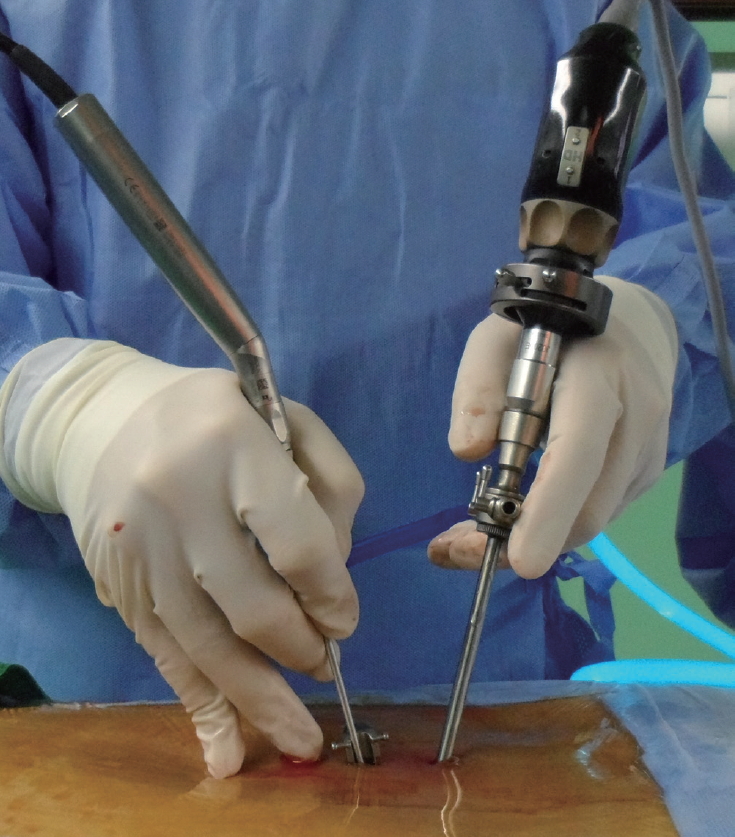
Fig. 2.
Two skin incision points for biportal endoscopic transforaminal lumbar interbody fusion. (A) Ordinary skin incision points were made over the pedicle area in the anteroposterior x-ray view. (B) Modified skin incision points. (B) An endoscopic portal incision was made near the intervertebral space for good visualization of the superior and inferior endplates.
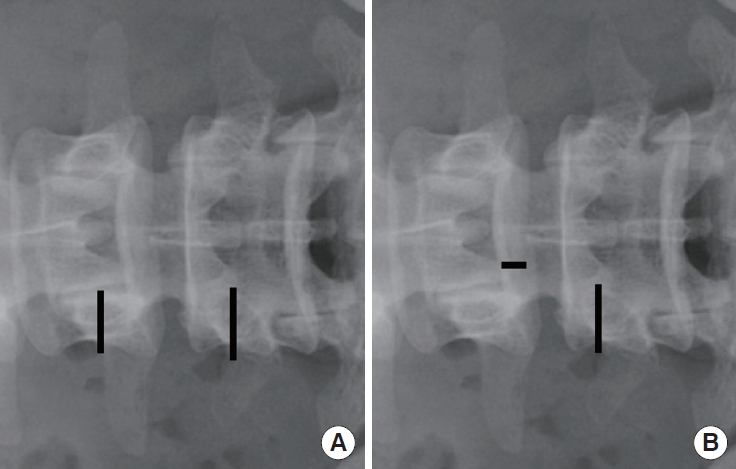
Fig. 3.
Biportal endoscopic view after neural decompression. (A) Ipsilateral traversing nerve root. (B) Central canal. (C) Contralateral traversing nerve root.
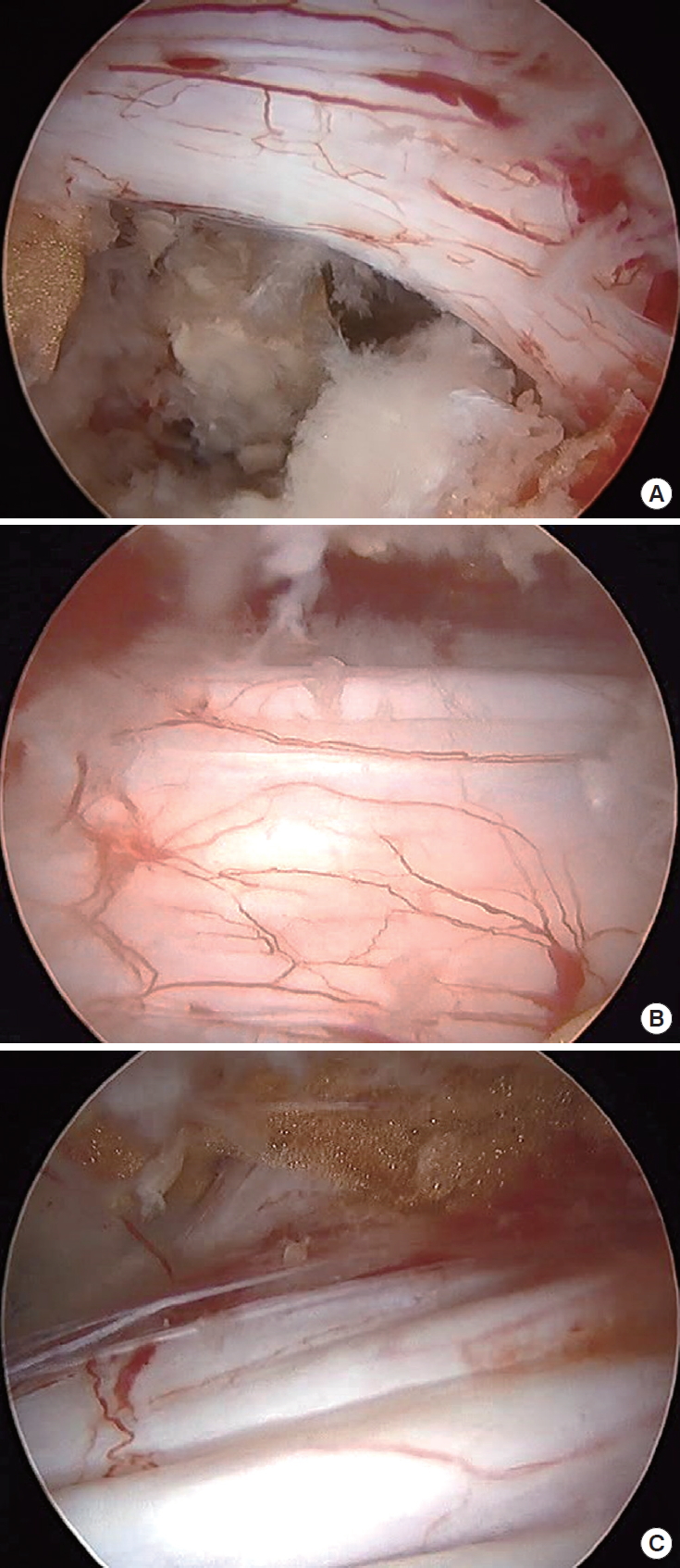
Fig. 4.
Endoscopic images during endplate preparation. (A) The cartilaginous endplate (arrowhead) was separated from the osseous endplate (arrow). (B) Final view of the endoscopic endplate preparation. The cartilaginous endplate was completely removed without injury to the osseous endplate.
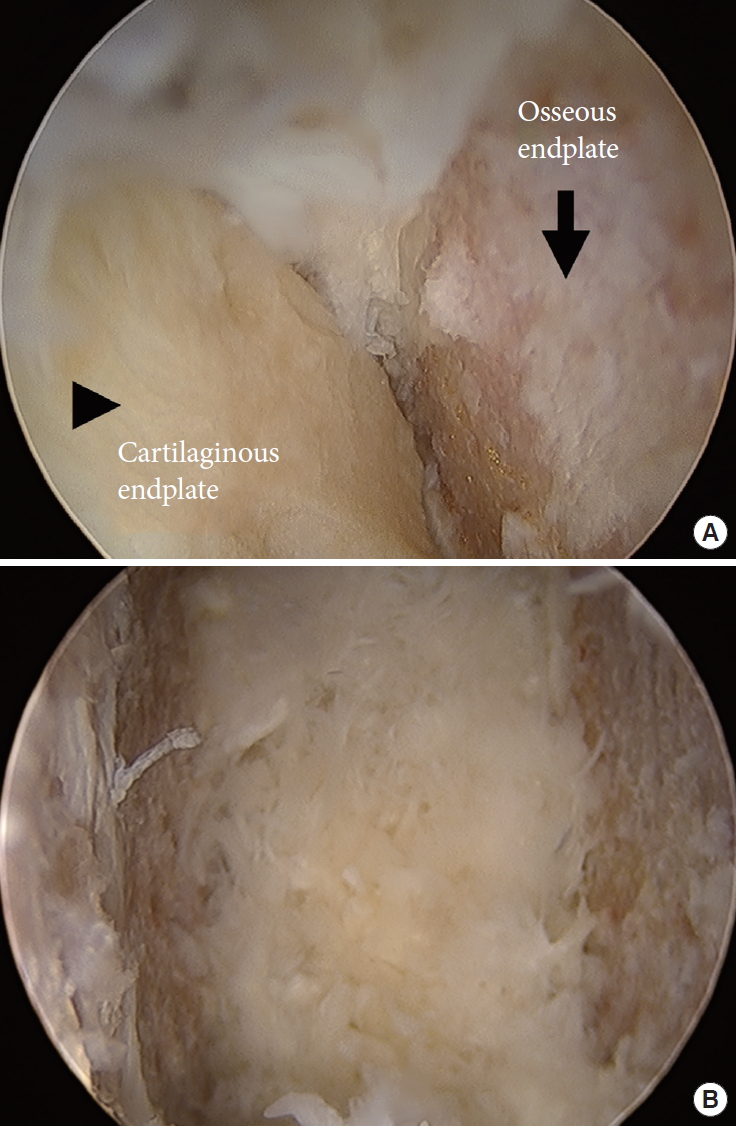
Fig. 5.
The fusion materials were inserted into the intervertebral space using a funnel before cage insertion (A. endoscopic view). (B, C) Overview of fusion material insertion using a funnel and an impactor.

Fig. 6.
Radiologic images of a 56-year-old female patient. (A) The preoperative magnetic resonance images show degenerative spondylolisthesis of L4–5. (B) After biportal endoscopic transforaminal lumbar interbody fusion (TLIF), the spondylolisthesis was well-resolved. Central stenosis of L4–5 (C) was decompressed after surgery (D). (E) The preoperative x-ray also revealed spondylolisthesis of L4–5. (F) The postoperative x-ray showed the large TLIF cage and percutaneous pedicle screw inserted.

Fig. 7.
A 55-year-old female patient presented with pain with claudication in both legs. (A) The preoperative magnetic resonance imaging showed degenerative spondylolisthesis with central stenosis at L4–5. (B) This patient received biportal endoscopic transforaminal lumbar interbody fusion using the 2-cage insertion technique. Preoperative spondylolisthesis (A) and central stenosis (C) were significantly resolved postoperatively (B, D). (E) The preoperative x-ray image demonstrates degenerative spondylolisthesis of L4–5. (F, G) The postoperative x-ray images reveal a reduction in spondylolisthesis and the presence of 2 inserted cages. The pain was significantly improved after surgery.

Fig. 8.
Two types of endoscopic transforaminal lumbar interbody fusion (TLIF). The trans-Kambin approach (A) and the posterolateral approach (B). The trans-Kambin approach was similar to transforaminal lumbar discectomy and the posterolateral approach was similar to minimally invasive TLIF with tubular retractor systems.
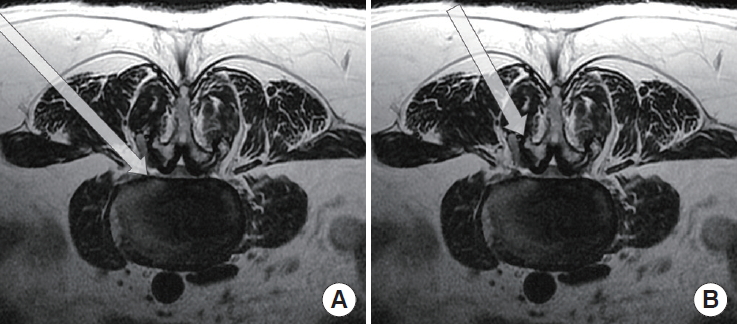
Table 1.
Comparison of 2 types of endoscopic TLIF
Table 2.
Summary of publications of biportal endoscopic lumbar interbody fusion
| Study | Publication year | Study design | Cases | Follow-up (mo), mean ± SD | Clinical outcomes | Perioperative complications |
|---|---|---|---|---|---|---|
| Heo et al. [5] | 2017 | Cases series | 69 Cases | 13.5 ± 7.1 | Improvement of VAS and ODI | Dura tear (2), hematoma (3) |
| Kim and Choi [18] | 2018 | Cases series | 14 Cases | Improvement of VAS | L5 root palsy (1), dura tear (1) | |
| Heo et al. [4] | 2019 | Cases control study | 23 Cases (biportal), 45 cases (microscopic) | 13.4 ± 2.5 | Improvement of VAS and ODI | Hematoma (1) |
| Park et al. [11] | 2019 | Cases control study | 71 Cases (biportal), 70 cases (conventional) | 17.1 ± 4.9 | Improvement of VAS and ODI | Dura tear (3), infection (1) |
| Hematoma (1) | ||||||
| Ahn et al. [2] | 2019 | Systemic review | - | - | - | - |
REFERENCES
1. Holly LT, Schwender JD, Rouben DP, et al. Minimally invasive transforaminal lumbar interbody fusion: indications, technique, and complications. Neurosurg Focus 2006 20:E6.

2. Ahn Y, Youn MS, Heo DH. Endoscopic transforaminal lumbar interbody fusion: a comprehensive review. Expert Rev Med Devices 2019 16:373-80.


4. Heo DH, Park CK. Clinical results of percutaneous biportal endoscopic lumbar interbody fusion with application of enhanced recovery after surgery. Neurosurg Focus 2019 46:E18.


5. Heo DH, Son SK, Eum JH, et al. Fully endoscopic lumbar interbody fusion using a percutaneous unilateral biportal endoscopic technique: technical note and preliminary clinical results. Neurosurg Focus 2017 43:E8.


6. Wang MY, Grossman J. Endoscopic minimally invasive transforaminal interbody fusion without general anesthesia: initial clinical experience with 1-year follow-up. Neurosurg Focus 2016 40:E13.

7. Morgenstern C, Yue JJ, Morgenstern R. Full percutaneous transforaminal lumbar interbody fusion using the facet-sparing, trans-Kambin approach. Clin Spine Surg 2020 33:40-5.


8. Ao S, Zheng W, Wu J, et al. Comparison of preliminary clinical outcomes between percutaneous endoscopic and minimally invasive transforaminal lumbar interbody fusion for lumbar degenerative diseases in a tertiary hospital: is percutaneous endoscopic procedure superior to MIS-TLIF? A prospective cohort study. Int J Surg 2020 76:136-43.


9. Wu J, Liu H, Ao S, et al. Percutaneous endoscopic lumbar interbody fusion: technical note and preliminary clinical experience with 2-year follow-up. Biomed Res Int 2018 2018:5806037.




10. Lee SH, Erken HY, Bae J. Percutaneous transforaminal endoscopic lumbar interbody fusion: clinical and radiological results of mean 46-month follow-up. Biomed Res Int 2017 2017:3731983.




11. Park MK, Park SA, Son SK, et al. Clinical and radiological outcomes of unilateral biportal endoscopic lumbar interbody fusion (ULIF) compared with conventional posterior lumbar interbody fusion (PLIF): 1-year follow-up. Neurosurg Rev 2019 42:753-61.



12. Kim HS, Wu PH, Jang IT. Technical note on Uniportal full endoscopic posterolateral approach transforaminal lumbar interbody fusion with reduction for grade 2 spondylolisthesis. Interdiscip Neurosurg 2020 21:100712. https://doi.org/10.1016/j.inat.2020.100712.

13. Lewandrowski KU, Ransom NA, Ramírez León JF, et al. The concept for a standalone lordotic endoscopic wedge lumbar interbody fusion: the LEW-LIF. Neurospine 2019 16:82-95.




14. Heo DH, Lee DC, Park CK. Comparative analysis of three types of minimally invasive decompressive surgery for lumbar central stenosis: biportal endoscopy, uniportal endoscopy, and microsurgery. Neurosurg Focus 2019 46:E9.

15. Heo DH, Quillo-Olvera J, Park CK. Can percutaneous biportal endoscopic surgery achieve enough canal decompression for degenerative lumbar stenosis? Prospective casecontrol study. World Neurosurg 2018 120:e684-9.


16. Heo DH, Sharma S, Park CK. Endoscopic treatment of extraforaminal entrapment of L5 nerve root (far out syndrome) by unilateral biportal endoscopic approach: technical report and preliminary clinical results. Neurospine 2019 16:130-7.




17. Shen J. Fully endoscopic lumbar laminectomy and transforaminal lumbar interbody fusion under local anesthesia with conscious sedation: a case series. World Neurosurg 2019 127:e745-50.



- TOOLS
- Related articles in NS
-
Journal Impact Factor 3.2



























