Outcomes of Patients Undergoing Anterior Screw Fixation for Odontoid Fracture and Analysis of the Predictive Factors for Surgical Failure
Article information
Abstract
Objective
Anterior odontoid screw fixation (AOSF) is a safe and effective treatment for type II and rostral type III odontoid fracture. This study aimed to report the outcomes of the AOSF surgery and evaluate the potential risk factors of surgical failure.
Methods
We enrolled 63 patients who underwent AOSF. Follow-up computed tomography was performed 6 months after the surgery and once a year thereafter to evaluate the union. Clinical data including the age, sex, presenting symptoms, cause of injury, fracture gaps, dislocation position, degree of displacement, screw direction angle, and time interval from injury to operation were collected.
Results
Successful fusion was achieved in 55 patients (87.3%) and surgical failure occurred in 8 patients (12.7%). Variables such as age, sex, dislocation position, degree of displacement, screw direction angle, and time interval from injury to operation were not significantly associated with the surgical failure. However, surgical failure was statistically significantly associated with the fracture gap. The overall mean fracture gap at the time of injury was 1.29 mm (range, 0–3.11 mm), and the incidence of surgical failure was 8.3 times higher when the fracture gap at the time of injury was > 2 mm (p=0.019).
Conclusion
When performing AOSF in patients with type II or rostral shallow type III odontoid fractures, the displacement of the odontoid fracture fragment should be appropriately reduced to the aligning position before screw insertion and downward reduction should be achieved by perforation of the apical cortex of the odontoid during screw fixation, even if the surgery is delayed.
INTRODUCTION
Odontoid fracture is common type of cervical spine fracture accounting for 5%–20% of all cervical spine fractures [1,2], and it is classified into 3 types according to the fracture location in the sagittal plane [3]. Type II and rostral shallow type III odontoid fractures are considered highly unstable and require surgical treatment [4-7]. Various treatment strategies have been attempted to prevent potential spinal cord injury and craniocervical deformities, spanning from conservative treatment with external immobilization to surgical treatment with anterior odontoid screw fixation (AOSF) or posterior cervical screw fixation with or without fusion [2]. Many studies have suggested that AOSF is a safe and effective treatment with the provision of immediate stabilization of the spine, preservation of substantial C1–2 rotatory motion, and a high union rate ranged of 88%–100% [8-11]. However, a few studies have reported AOSF-related complications or nonunion related risk factors after AOSF.
In this study, we report the outcomes of AOSF surgery for odontoid fractures by analyzing the radiologic and clinical data. We have also evaluated the potential risk factors of surgical failure associated with this technique.
MATERIALS AND METHODS
1. Patient Population and Study Design
This study fulfilled all the requirements for patient anonymity and was approved by the Institutional Review Board of Chonnam National University Medical School Research Institution, Republic of Korea (CNUH-2020-054).
This study included 63 patients who underwent AOSF between January 2001 and June 2019 at our institution. All patients were preoperatively assessed using anteroposterior, lateral, and open-mouth plain radiographs. Preoperative computed tomography (CT) and magnetic resonance imaging (MRI) of the spine were also performed in all patients. The indications for AOSF were an Anderson and D’Alonzo type II or a rostral shallow type III odontoid fracture with intact transverse ligament on MRI [3]. Patients with AOSF contraindications (such as disruption of transverse ligament, fracture > 6 months ago, comminuted fracture, and pathologic fracture) and those with < 12 months of clinical or radiological follow-up after surgery were excluded from the study. All AOSF surgeries were performed by a single surgeon. During follow-up, anteroposterior, lateral, flexion, and extension plain radiographs were taken postoperatively, 6 months after the surgery, and once a year thereafter. Similarly, follow-up CT was performed 6 months after the surgery and once a year thereafter to evaluate the union. Successful fusion was defined as the presence of a bony bridge and definite continuity of the cortical bone or absence of motion and fracture gap at the fractured site on dynamic radiographs despite persistent cortical bone discontinuity within a fracture gap on CT. Surgical failure was defined as a definite fracture gap with abnormal motion at the fractured site on dynamic radiographs and CT that may require additional surgical treatment, such as posterior cervical fixation with or without fusion. Follow-up was discontinued when the fracture was considered clinically and radiologically stable. To analyze the clinical characteristics of the patient, clinical data at the time of treatment, including age, sex, presenting symptoms, cause of injury, fracture gaps, dislocation position, degree of displacement, screw direction angle, and time interval from injury to operation were collected. Fracture displacement was measured perpendicularly from a line through the posterior margin of the odontoid fracture, drawn parallel to the posterior wall of the C2 vertebral body using preoperative CT scans. Fracture gap was measured as the largest gap between the superior fracture line of the odontoid process and the inferior fracture line of C2 vertebral body using preoperative CT scans. The screw direction angle was measured between the inferior endplate of the vertebral body and the inserted screw in the cervical lateral plain radiographs (Fig. 1).
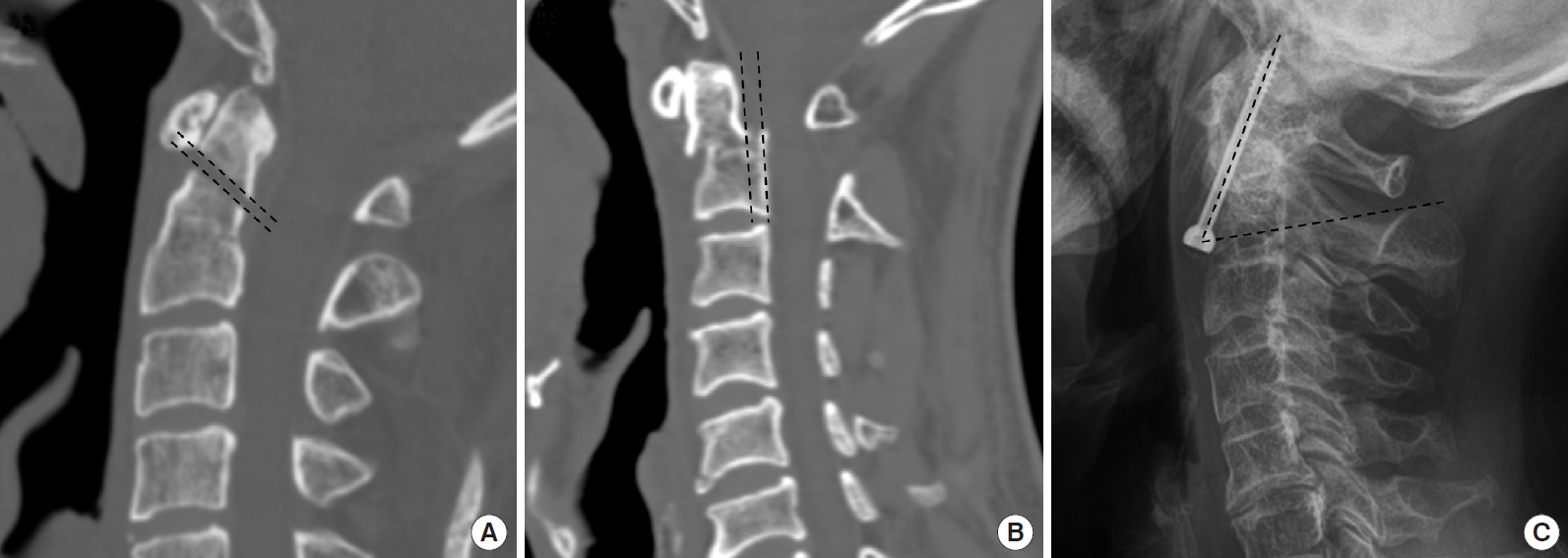
(A) Fracture gap: the largest gap between the superior fracture line of the odontoid process and the inferior fracture line of the C2 vertebral body. (B) Fracture displacement: perpendicular from a line through the posterior margin of the odontoid fracture, drawn parallel to the posterior wall of the vertebral body. (C) The screw direction angle is measured between the inferior endplate of the vertebral body and the inserted screw in the cervical lateral plain radiograph.
A visual analogue scale (VAS) of neck pain and the Neck Disability Index (NDI) were used preoperatively and postoperatively and at the last follow-up for clinical evaluation.
2. Surgical Technique
General anesthesia was used in all patients. After the patient was placed in a supine position on the operating table, we tried to achieve the correct alignment of the C2 vertebral body and fragment of the odontoid process with Gardner-Wells tongs using 2 fluoroscopies (open-mouth and lateral view). A transverse incision was made along the skin crease at the C5–6 level. The standard Smith-Robertson method was used to expose the prevertebral space. After exposing the anterior cervical spine, the anterior-inferior edge of C2 was exposed. Under fluoroscopy, a 2-mm Kirschner wire was drilled from the midline of anterior-inferior edge of C2 to the apical cortical bone of dens. A hollow hand drill was used to enlarge the trajectory over the Kirschner wire. A cannulated lag screw measuring 4.5 mm in diameter was inserted along the Kirschner wire and advanced through the tapped hole under fluoroscopy. We confirmed that the distal fragment was pulled down to the C2 vertebral body as the screw tightened. Neck brace was used postoperatively for 12 weeks in all patients.
3. Statistical Analysis
Continuous variables are expressed as mean and standard deviation. A paired t-test was used to compare the measurements taken at different time points. Multivariate logistic regression analysis was used to identify the predictive factors for surgical failure. The following variables related to surgical failure were evaluated: age, sex, cause of injury, fracture gaps, dislocation position, degree of displacement, screw direction angle, and time interval from injury to operation. All statistical analyses were performed using IBM SPSS Statistics ver. 26.0 (IBM Co., Armonk, NY, USA). Values of p<0.05 were considered significant.
RESULTS
1. Patient Characteristics
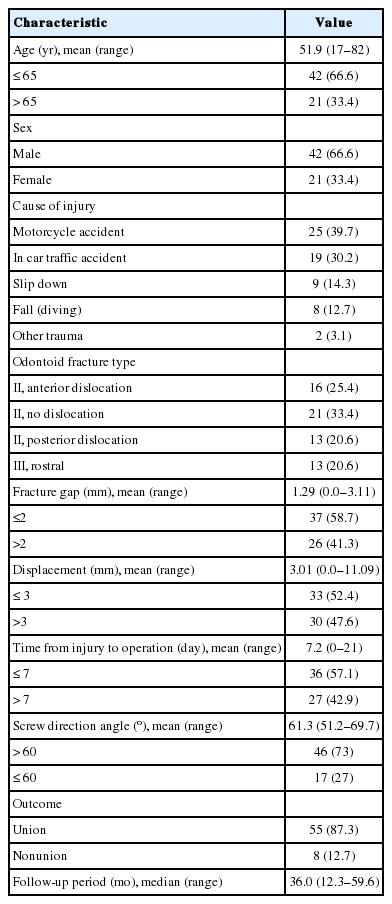
The mean age of patients at the time of surgery was 51.9 years (range, 17–82 years). Of the total patients, 42 (66.6%) were men and 21 (33.4%) were women. Motorcycle accident was the most common cause of injury (39.7%), followed by in car traffic accidents (30.2%), slipping down (14.3%), and fall (12.7%). On the basis of preoperative imaging, 16 patients (25.4%) had type II odontoid fractures with anterior dislocation, 21 patients (33.4%) had type II odontoid fractures with no dislocation, 13 patients (20.6%) had type II odontoid fractures with posterior dislocation, and 13 patients (20.6%) had rostral shallow type III odontoid fractures. AOSF was performed after a mean of 7.2 days (range, 0–21 days) after injury, and the mean follow-up duration after surgery was 36.0 months (range, 12.3–59.6 months). The clinical characteristics of the enrolled patients are summarized in Table 1.
2. Clinical Outcomes
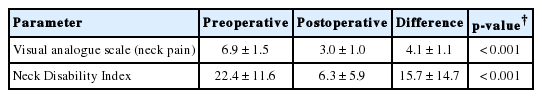
The mean VAS score of neck pain decreased by 5.1 points, from 6.9±1.5 at injury to 3.0±1.0 postoperatively (p<0.001). The overall mean change in the NDI score was 15.7, from 22.4±11.6 at injury to 6.3±5.9 postoperatively (p<0.001) (Table 2). No patient reported worsening pain or increased NDI score after surgery. None of the patients developed AOSF-related complications such as neurological deterioration, anterior cervical space hematoma, surgical site infection, dysphagia, and cardiopulmonary complications.
3. Radiological Outcomes and Predicting Factors for Nonunion
During the follow-up period, successful fusion was achieved in 55 patients (87.3%) and surgical failure occurred in 8 patients (12.7%). The VAS and NDI scores improved in all patients, including those with surgical failure after surgery. However, additional surgical treatment was performed in patients with surgical failure after surgery because a fracture gap and abnormal motion were detected radiologically. Seven patients underwent posterior C1–2 transarticular screw fixation with wiring, and 1 patient underwent C1 lateral mass and C2–3 pedicular screw fixation.
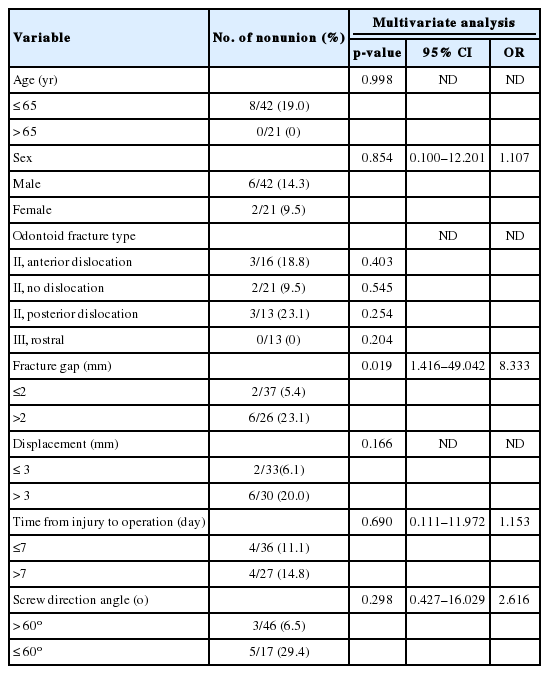
Analysis of the variables that could be correlated with the nonunion is shown in Table 3. Variables such as age, sex, dislocation position, degree of displacement, screw direction angle, and time interval from injury to operation were not significantly associated with surgical failure. However, there was a statistically significant association between surgical failure and the fracture gap. The overall mean fracture gap at the time of injury was 1.29 mm (range, 0–3.11 mm), and the incidence of surgical failure was 8.3 times higher when the fracture gap at the time of injury was > 2 mm. (p=0.019; 95% confidence interval, 1.416–49.042; odds ratio, 8.333).
4. Case Illustration
A 37-year-old woman was admitted to our hospital with neck pain after a car traffic accident. A neurological examination revealed no abnormal findings. Radiological findings of the cervical spine showed a type II odontoid fracture with 3.2 mm of anterior displacement and 2.69 mm of fracture gap (Fig. 2A). She underwent AOSF 2 days after the injury (Fig. 2B) [7]. The 6 months postoperative follow-up cervical CT revealed nonunion with periscrew radiolucency (Fig. 2C, D). She underwent additional posterior C1–2 transarticular screw fixation with wiring (Fig. 2E).
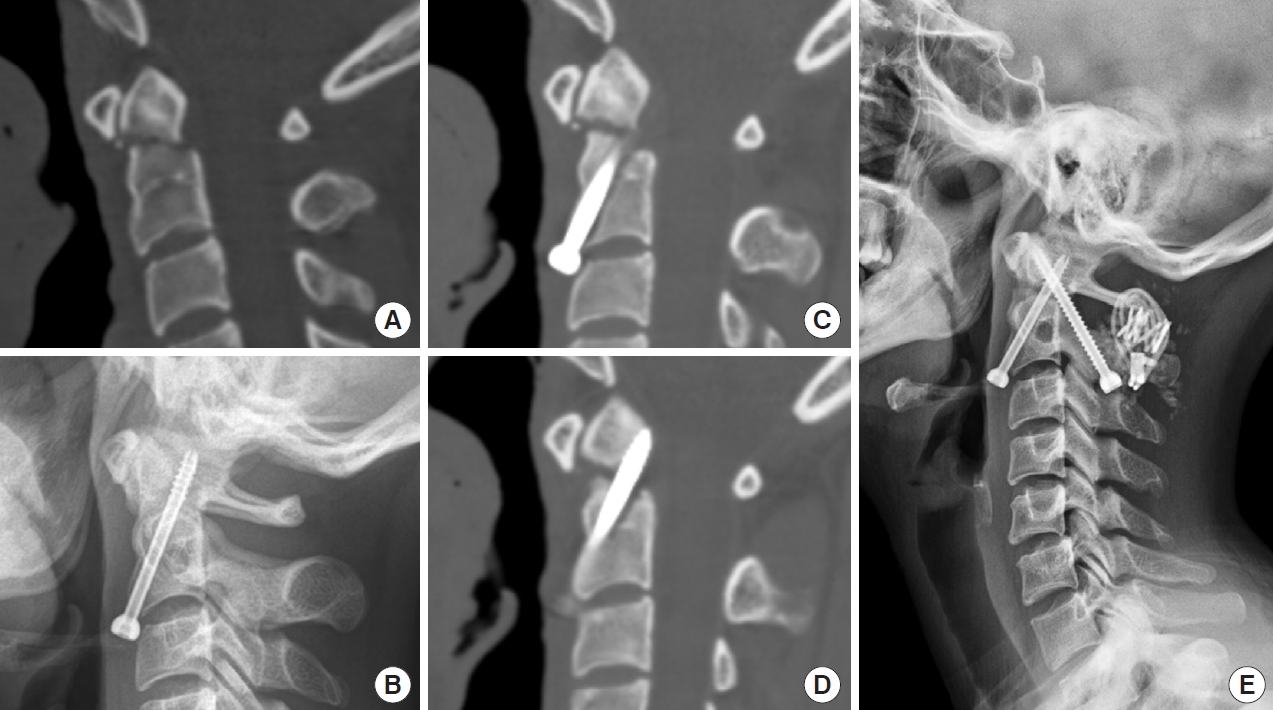
(A) Preoperative computed tomography (CT) image showing type II odontoid fracture with 3.2 mm of anterior displacement and 2.69 mm of fracture gap. (B) Cervical plain radiograph showing anterior odontoid screw fixation with a screw direction angle of 53.8°. (C, D) At 6 months after surgery, follow-up cervical CT showing nonunion with periscrew radiolucency. (E) Cervical plain radiograph showing C1–2 transarticular screw fixation with wiring.
DISCUSSION
The odontoid process of the C2 vertebrae controls the rotatory movements and restricts the translational movements in the most mobile segment of the cervical spine [12]. Fracture of the odontoid process can occur due to the flexion or extension force of the cervical spine, which usually result from low-energy impact such as a fall in elderly patients and high-energy impact such as motorcycle accidents or diving in younger patients [13,14]. Many studies have suggested that AOSF is safe and effective in stabilizing acute type II and rostral type III odontoid fractures [8-11]. Although controversy exists regarding the best way to manage odontoid fractures such as the anterior versus posterior approach [15], it is certain that AOSF has several biomechanical advantages such as preservation of substantial C1–2 rotatory motion and a high union rate (88%–100%) [8-11]. In this study, a successful fusion rate of 87.3% was achieved, and none of the patients experienced worsening pain or had increased NDI scores after surgery.
Several studies have identified predictive factors for surgical failure after AOSF and AOSF-related complications [2,5,15-17]. Regarding patients’ clinical characteristics, some studies have reported that old age is a predictive factor for surgical failure after AOSF for odontoid fractures and AOSF-related complications such as dysphagia and cardiopulmonary complications [16,17]. In contrast, some studies have reported that old age does not influence the union and that AOSF is suitable for elderly patients with odontoid fractures [5,18]. Similarly, in our study, patient age was not a significant predictive factor for surgical failure after AOSF (p=0.998). In addition, there were no surgery-related complications, such as neurological deterioration, anterior cervical space hematoma, surgical site infection, dysphagia, and cardiopulmonary complications.
Regarding patient's radiological characteristics, it is controversial if large fracture gap and severe displacement of odontoid fractures are risk factors of surgical failure after AOSF. According to Green et al. [19], odontoid displacement of ≥ 6 mm at injury is associated with surgical failure. In a study by Koivikko et al. [20], a fracture gap of ≥ 1 mm, posterior dislocation and displacement of ≥ 5 mm of odontoid fracture were risk factors of surgical failure. Our study result, which shows that a fracture gap > 2 mm is predictive factor for surgical failure (p=0.019), is consistent with the previous findings that a large fracture gap is a risk factor of surgical failure. Therefore, we recommend that, although it may be technically difficult, perforation of the apical cortex of the odontoid process should be performed to achieve appropriate downward reduction of the fracture during AOSF, especially in patients with a fracture gap of > 2 mm.
Park et al. [6] reported that with a larger direction angle, sufficient engagement of the odontoid process can be achieved without injury to the bone or disc, and good results can be expected after AOSF. In their study, the mean screw direction angle was 60.5±4.63 and the fusion rate was 100%. However, the screw direction angle was not significantly associated with surgical failure (p=0.298) in our study. In addition, unlike previous studies, the degree of fracture displacement was not a significant risk factor of surgical failure in our study. In a study by Cho et al. [7], fracture displacement was not a significant risk factor of fusion failure, which is similar to our results. With the development of medical technology such as intraoperative neurophysiologic monitoring, the displacement of the odontoid fracture fragment can be sufficiently reduced to a well-aligned position using Gardner-Wells tongs under general anesthesia (Fig. 3). In addition, this may also explain the results of our study that the dislocation position is not risk factor for surgical failure after AOSF surgery. Therefore, we recommend that, although the displacement of the odontoid fracture segment at the injury is severe, AOSF is sufficient if the displacement is adequately reduced before surgery and that other surgical methods such as the posterior approach should be considered if the reduction fails.
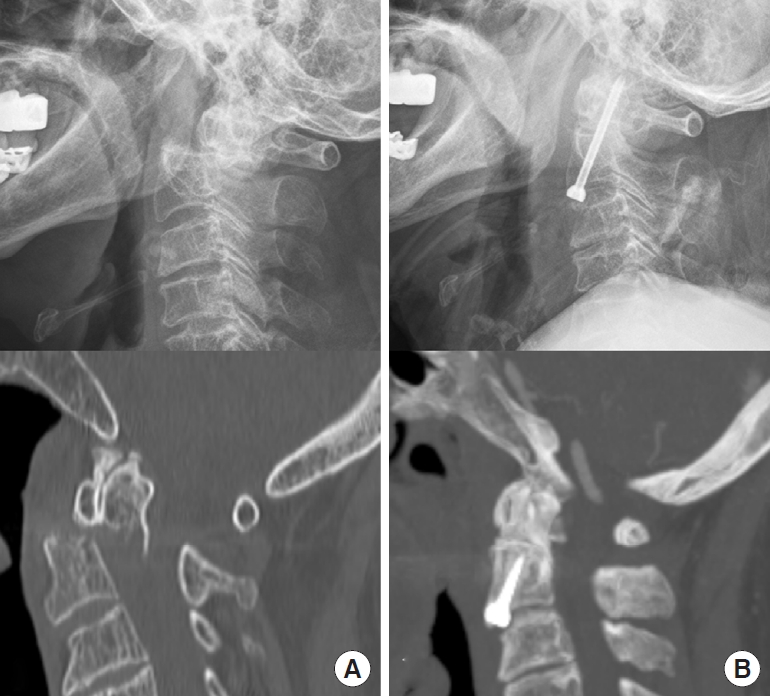
(A) Preoperative plain radiograph and computed tomography (CT) image in lateral plane showing a displacement of 11.09 mm and fracture gap of 2.83 mm. (B) At 18 months after surgery, plain radiograph and CT image in lateral plane showing the union state with a screw direction angle of 57.9°.
Further, it is controversial if delayed AOSF is a risk factor of surgical failure. Cho et al. [5] reported that the incidence of nonunion is 37.5 times higher for a patient if AOSF is delayed with for > 1 week after injury. However, the results of our study revealed that a delay of ≥ 1 week was not significantly associated with nonunion after AOSF (p=0.690). Similarly, Lobo et al. [9] reported that surgical timing was not significantly associated with successful fusion. In their study, the average time from trauma to surgery was 7 days, and they suggested that the success of AOSF depends on the selection of the appropriate patients, technical care in the perioperative period, and surgeon’s experience. Since the general condition of patient can affect bone healing, we recommend that it is acceptable to perform AOSF after recovery of the general condition in trauma patients. Moreover, rather than the timing of surgery, it is important that the displacement of the odontoid fracture fragment is appropriately reduced to the aligning position prior to screw insertion, and that downward reduction is achieved by perforation of the apical cortex of the odontoid during screw fixation.
This retrospective study has some limitations. First this study was performed at a single institution with a small number of patients. Second, the decision for the surgical method was not randomized and only cannulated lag screw was used in this study. Third, selection bias may occur because patients who did not achieve adequate reduction before AOSF were excluded. Further biomechanical and prospective studies are needed to determine the ideal surgical technique to improve the outcome.
CONCLUSION
AOSF achieved successful fusion in 87.3% patients with type II or a rostral shallow type III odontoid fracture. Fracture gap of > 2 mm is a predictive factor associated for surgical failure. When performing AOSF in patients with type II or rostral shallow type III odontoid fractures, the displacement of the odontoid fracture fragment should be appropriately reduced to the aligning position before screw insertion and downward reduction should be achieved by perforation of the apical cortex of the odontoid during screw fixation, even if the surgery is delayed.
Notes
The authors have nothing to disclose.