 |
 |
- Search
|
|
||
See commentary "The Underdiagnosed, Understudied Complexity of Pseudoangina: Should Clinicians Take a Neurosurgical Approach in Diagnosing Unexplained Visceral Pain?" in Volume 18 on page 250.
See commentary "Cervical Angina" in Volume 17 on page 939.
Abstract
Cervical angina is an often-overlooked etiology of noncardiac chest pain that may mimic true angina pectoris but is due to cervical spine disease. Diagnosis can be difficult, and treatment ranges from conservative therapy to surgical management. However, of patient’s refractory to conservative therapy, approximately ninety percent experience postoperative relief of angina symptoms. Here, we present a case report on cervical angina and performed a systematic review of the literature. A 34-year-old male with prior surgery for thoracic outlet syndrome presented with persistent anterior neck and chest pain as well as posterior left scapular and upper lateral arm pain. The pain was refractory to 12 months of conservative therapy. Cardiac workup was negative and cervical spine imaging revealed a C6–7 herniation with neuroforaminal stenosis. A systematic literature search was conducted in PubMed, Web of Science, and Cochrane databases from database inception to April 2020. Studies reporting cervical level, average symptom duration, location of pain, and postoperative pain improvement were included. The patient's atypical symptoms were completely resolved after C6–7 anterior cervical discectomy and arthroplasty. To our knowledge, this is the first study which reports on the use of arthroplasty in the treatment of cervical angina. The systematic review included 11 articles from 1989–2020 consisting of 1,186 total patients and 109 patients (age range, 36–84 years; 60.7% male) meeting inclusion criteria. Symptom duration range was 2 days to 90 months, with the most common location of pain being localized to the anterior chest wall (66.7% of patients). All patients (100%) had postoperative resolution of their pain symptoms. The most common herniation level was C6–7 (87.3% of patients). We conclude that a broad and multidisciplinary approach is necessary for the diagnosis and management of noncardiac chest pain. When cervical disease is identified as the underlying cause for the angina-like pain, conservative therapy should be sought. Refractory cases should be treated surgically depending on the cervical pathology.
Cervical angina, or pseudoangina, is a rare and likely underdiagnosed clinical syndrome in which cervical spondylarthropathy and degenerative disc disease presents as chest and scapular pain due to either nerve root irritation and compression or, less commonly, central stenosis and myelopathy [1-4]. Cervical angina has been described in association with a multitude of symptoms including nausea, parasternal tenderness, transient neck pain and stiffness, shortness of breath, vertigo, occipital headaches, and neurogenic bladder [2,3,5-9]. Angina-like pain has also been commonly reported with active neck motion [2,4-6]. In fact, Güler et al. [5] report reproduction of pseudoangina with ECG changes during neck anteflexion. Cervical angina secondary to myelopathy may be additionally associated with autonomic symptoms such as dyspnea, diaphoresis, fatigue, and diplopia [1,3,8]. It has been speculated that cervical angina due to myelopathy may be more difficult to diagnose due to the greater incidence of autonomic symptoms and lower incidence of upper extremity symptoms [1,8].
The prevalence of cervical angina has not been clearly established. It has been reported that up to 50% of patients evaluated for chest pain have normal coronary arteriography [10,11]. Of these patients, the true frequency of cervical angina is unclear due to delays in appropriate diagnostic evaluation during extensive cardiac work ups. A definitive diagnosis of cervical angina can only be made once coronary artery disease is ruled-out [2,4,6,8]. A thorough history and physical examination, and imaging modalities such as a radiography and magnetic resonance imaging are critical to establishing a diagnosis of cervical angina [3,4]. A standard Spurling maneuver as part of physical examination to reproduce pain due to foraminal stenosis has been demonstrated to reproduce anginal pain in this syndrome [2-5]. Further, functional nerve studies such as electromyography, discography, positron emission tomography, and diagnostic nerve block can help confirm the diagnosis [3,4,8].
As with more typical cervical radiculopathy and stenosis, conservative measures including rest, physical therapy, cervical orthosis, intermittent cervical traction, nonsteroidal anti-inflammatory drugs, and muscle relaxants should be attempted first [1,2,4,8]. Failure of conservative management or the presence of significant spinal cord or nerve root compression may be an indicator for surgical management [1,2,4]. There have been multiple reports regarding the use of procedures such as anterior cervical discectomy and fusion as well as subtotal spondylectomy in the treatment of cervical angina [2,3,8,12]. However, to our knowledge there are no reports on the role cervical arthroplasty in the treatment of cervical angina.
We present here a case study on the management of cervical angina with anterior cervical discectomy and arthroplasty at C6–7 level. We also performed a systematic review on the relevant literature.
A 34-year-old male with a prior history of thoracic outlet syndrome treated with multiple surgeries including a first rib and anterior and middle scalene resection presented with 2 years of persistent left anterior neck and chest pain, as well as posterior left scapular and upper outer arm pain refractory to 12 months of physical therapy, epidural steroid injections, stellate ganglion injection, and smoking cessation. After a negative cardiology work up was performed a neurologic work up was performed. He demonstrated 5/5 bilateral upper extremity strength throughout with fully intact sensation. Of note, he displayed no hyperreflexia, a negative Hoffman's bilaterally, negative Romberg and the ability to tandem walk without difficulty. Multimodal cervical spine imaging was performed. Magnetic resonance imaging demonstrated herniation of the C6–7 disc upon weight-bearing, with a protrusion of 3.6 mm, and disc material abutting the anterior aspect of the spinal cord (Fig. 1), along with moderate bilateral neural foraminal narrowing and annular fissure (Fig. 2). Radiographs demonstrated slight loss of normal cervical lordosis centered at C4–5 (Fig. 3) with otherwise normal spine alignment and no instability on flexion and extension (Fig. 4). A surgical approach of C6–7 anterior cervical discectomy and arthroplasty with a Prestige LP (Medtronic, Dublin, Ireland) implant was planned.
A left-sided standard Smith-Robinson approach was utilized to expose the anterior vertebrae. The appropriate level was localized with an x-ray at C6–7 and the longus coli were elevated bilaterally. The patient's disc was removed in its entirety at C6–7 using bilateral foraminotomies and a left-sided uncinate decompression. The region was then reconstructed with a Prestige LP, 6× 16 mm, arthroplasty implant after templating it to an appropriate size.
The patient reported complete resolution of his pain immediately upon waking up postoperation. Radiographic images of the cervical spine demonstrated good positioning of the C6–7 arthroplasty implant. At 6-month follow-up, the patient has maintained complete resolution of his cervical angina pain and has discontinued all pain medications. Repeat radiographs at 6 months showed his implant to be in good stable position (Figs. 5-7).
With Institutional Review Board exemption, a systematic review was performed targeting studies investigating cervical disc herniation in the subaxial cervical spine (C3–7) resulting in chest pain. This systematic review evaluated cervical level, average symptom duration, location of pain, and postoperative improvement of pain.
On April 10th, 2020, a literature search was conducted using PubMed, Web of Science, and Cochrane databases using the PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-analyses) recommendations [13]. In order to include as many relevant articles as possible, there were no restrictions on the date of publication when searching databases. The following Boolean search terms were used: (“cervical”) AND (“angina” OR “chest pain”) AND (“herniation”).
Our search yielded 83 results from PubMed, 40 results from Web of Science, and 0 result from Cochrane, with a total of 89 unique articles after the removal of duplicates. The reference lists from articles identified during our search were analyzed individually for additional studies that met inclusion criteria, yielding an additional 10 papers (Fig. 8).
All articles reviewed were subject to the following inclusion criteria: (1) availability of the manuscript in English or an English translation, (2) primary clinical studies investigating cervical disc herniation in the subaxial cervical spine (C3-7) resulting in chest pain. All articles reviewed were also subject to the following exclusion criteria: (1) axial cervical spine, (2) nonherniation pathologies of the cervical spine.
Titles and abstracts of studies for this systematic review were evaluated independently by 2 authors (RS and LDA). The reviewers then compared these selections, and disagreements were resolved by further discussion with the senior author. Final selections were chosen by both authors independently after examining full-text articles, after which the methodological index for nonrandomized studies (MINORS) criteria was used to objectively evaluate the quality of the studies and evaluate the risk of bias for selected studies [14]. Each item on the MINORS checklist was independently scored by 2 authors as 0 (not reported), 1 (reported but inadequate), and 2 (reported and adequate), then averaged. Since all selected articles were noncomparative studies, the maximum score was 16. As previously described, we considered a score of below 5 as poor, between 6 and 10 as moderate, and between 11 and 16 as good [15]. Because scores were averaged, noninteger values were rounded down to reduce the risk of overestimating study quality.
Out of the 89 unique papers from the database search and review of reference lists, 75 papers were examined in full text. Out of 89 papers, 11 papers met both inclusion and exclusion criteria (Table 1). These 11 articles were included for further analysis.
A total of 11 articles were selected matching our inclusion and exclusion criteria for this systematic review (Table 1). The papers included 6 case series and 5 case reports. The study publication dates ranged from 1989–2020. The sample size across all the studies was 1,186 patients, and after filtering out inclusion and exclusion criteria, the final cohort was 109 patients. The cohort ranged in age from 36–84 years. Gender was reported for only 28 patients (25.7%), with 17 patients (60.7%) being male. Average symptom duration ranged from 2 days to 90 months. Of the 15 patients in which the location of the chest pain was reported, 3 patients (20%) reported primarily retrosternal pain, 1 (6.7%) reported primarily epigastric pain, 10 (66.7%) reported primarily anterior chest pain, 1 (6.7%) primarily reported upper back pain. Postoperative resolution of symptoms was reported in 92 (84.4%). All 92 patients (100%) demonstrated complete resolution of symptoms postoperatively. A total of 55 patients (50.5%) reported the cervical level at which the herniation occurred. The most common level was C6–7, with 48 patients (87.3%), followed by C5–6 with 5 patients (9.1%), followed by C4–5 with 1 patient (1.8%), and C3–4 with 1 patient (1.8%).
The mean MINORS criteria score was 5.45 (range, 3–8) for the 11 studies selected for this systematic review. The studies by Ozgur and Marshall [12], Nakajima et al. [8], Sussman et al. [3], and Brodsky et al. [1] received the highest score with 8 and were considered moderate studies. A total of 5 studies were considered poor and the other 2 studies were considered moderate.
The pathogenesis of cervical angina is an area of study and speculation and is a widely reported source of unrecognized chest pain [2,8,16]. Cervical angina has been described most commonly with disc herniation at the C5–6, C6–7 levels [1-4]. The pain is thus potentially mediated by the medial and lateral pectoral nerve [2,8]. Nerve roots from C4 to C8 contribute to sensory and motor innervation of the anterior chest wall, shoulder, and arm and thus are believed to be involved in the primary pathogenesis of cervical angina [2,5]. In addition to radiculopathy caused by cervical disc hernia, other causes of cervical angina involving nerve root compression include osteoarthritic spurs and narrowing of intervertebral foramina [1,7,17]. Cervical angina can also be myelopathic, involving direct compression of the cervical spinal cord [3,6,8]. Furthermore, spinal infarction and ischemia have been reported as causes of cervical angina [6-8,18]. The role of spinal ischemia in the pathogenesis of angina-like pain, may explain reports of nitroglycerin causing symptomatic improvement of chest pain unexplained by coronary artery disease [2,5,19]. In addition, protopathic pain involving pressure on ventral motor roots as well as referred pain caused by focal lesions in the neck due to such factors as facet syndrome, disc degeneration, or disease of the anterior or posterior longitudinal ligament may be causes of cervical angina [3,7,8]. Cases of cervical angina secondary to an ossified posterior longitudinal ligament (OPLL) have been described [8,9]. Lastly, sympathetic pain and involvement of sinuvertebral nerves have been discussed as being potentially involved in the pathogenesis of some cases of cervical angina [2,8,20,21].
The particular pathogenic processes involved in a cervical angina case can be significant in informing therapy. Table 1 reports on the clinical data reported cases of cervical angina present within the literature. Most were caused by disc herniation, an OPLL, and the remaining cases were caused by spinal infarction, atlantoaxial instability, and neuroforaminal stenosis. Of these studies 7 of 11 reported improvement in symptoms following surgical intervention [1,3,8,12,22-29]. Nakajima et al. [8] report resolving cervical angina caused by an OPLL with anterior decompression with interbody fusion, at the C5–6 and C6–7 levels, along with a subtotal spondylectomy at the C6 level. One patient reported improvement with conservative therapy, including rest and a neck collar, and a total of 3 patients refused surgical intervention [5,9].
Ozgur and Marshall [12] report that 16% of 241 patients undergoing anterior cervical discectomy presented with chest pain or subscapular pain. Of these patients, 90% experienced significant to complete symptomatic relief after anterior cervical discectomy. Jacobs [2] reports on 164 cervical angina patients, the majority of which achieved symptomatic relief through conservative management. Furthermore, 38 of the 164 (23%) were refractory to conservative management and underwent anterior disc excision and spinal fusion. Of these, 33 patients (87%) achieved complete symptomatic relief and the remaining 5 patients achieved complete relief after subsequent revision surgery [2]. Nakajima et al. [8] reports on 10 surgical patients with cervical pathology who exhibited symptoms of pseudoangina. The patients underwent either anterior decompression (n = 6) or subtotal spondylectomy (n = 4), and all of them achieved symptomatic relief within 4 months of operation.
Better guidelines should be established for the diagnosis and management of cervical angina. Clinicians must consider a broad differential diagnosis for chest pain unexplained by coronary artery disease. When present, neurological symptoms should not be overlooked as a separate clinical entity. Guidelines for diagnoses should involve a thorough physical examination, including neurological examination, cooperation among specialties and should consider the cost of exhaustive cardiac examination. Once diagnosed, management of cervical angina must balance the risk factors and cost of surgical intervention with the probability of patient pain relief and life-style improvement. The majority of cervical angina patients achieve symptomatic relief through conservative management [1-3]. In patients in which conservative therapy fails to provide sufficient relief, various surgical procedures should be considered, including cervical arthroplasty.
Cervical arthroplasty, or total disc replacement, is a well-established alternative in appropriate patients who would benefit from motion sparing discectomy. As traditional fusion surgery is typically extremely well tolerated, there is some equanimity among the neurosurgical community about the benefit of arthroplasty. However, numerous clinical trials and meta-analyses are showing at least noninferiority and in most cases are describing improved patient pain outcomes, decreased recovery times, preserved motion, and decreased adjacent level disease with arthroplasty when compared with fusion [30-33]. Given our patient’s young age and degenerative pathology isolated to a single vertebral level, we felt that he was an ideal candidate for cervical arthroplasty surgery.
We present this unique case to highlight the nuance involved in the diagnosis and treatment of cervical angina. The patient presented with atypical symptoms complicated by a history of thoracic outlet syndrome and multiple surgeries. The patient's symptoms of left anterior neck and chest pain as well as posterior left scapular and upper outer arm pain were refractory to several conservative therapies and had persisted for greater than 2 years. The patient’s symptoms were consistent with cervical angina with a component of C7 radiculopathy, which was potentially referable to his disc herniation and neuroforaminal stenosis at C 6/7. We, therefore, pursued surgical management given his failure of conservative management and debilitating pain with correlative imaging findings. This is the first study which reports on the use of arthroplasty in the treatment of cervical angina. The patient's atypical symptoms of cervical angina appear to have completely resolved with the discectomy and arthroplasty at the C6–7 level.
We also present the first reported systematic review on cervical disc herniation in the subaxial cervical spine (C3–7) resulting in chest pain. The results are consistent with the reported literature, with all patients experiencing postoperative symptomatic recovery from their chest pain. The majority of included studies were small single institutional retrospective analyses or case reports, which reported extremely heterogeneous clinical data. Though great care was taken in collecting relevant studies an performing the appropriate analyses, this study has a number of limitations. First, this systematic review was comprised of several collective studies and case reports with intrinsic heterogeneity in treatment guidelines and measurement of outcome variables. There were inconsistent patient baselines and follow-up timelines in the included cases, which makes the analysis difficult to control or standardize. Furthermore, differences in reported outcomes and the incomplete presentation of clinical data for patients meeting inclusion criteria, coupled with the relative rarity of relevant cases, increases the susceptibility for type II error and false-negative conclusion. Nonetheless, this systematic review is the first to synthesize the reported cervical level, average symptom duration, location of pain, and postoperative improvement of pain of patients with chest pain secondary to cervical disc herniation in the subaxial cervical spine (C3–7) [1,3,8,12,22-29].
Fig. 1.
T2-weighted magnetic resonance imaging showing sagittal view (A) of the cervical spine and sagittal view (B) demonstrating increased signal within the spinal cord from C2–T1.
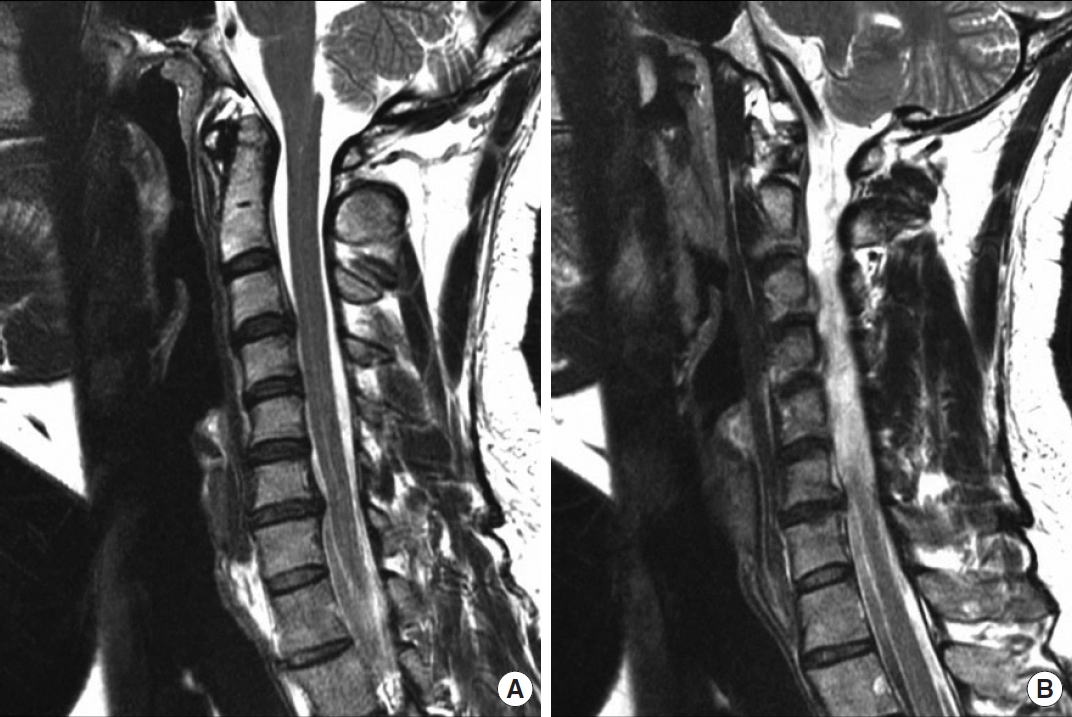
Fig. 2.
T2-weighted magnetic resonance imaging showing an axial view of the cervical spine demonstrating mild to moderate bilateral neural foraminal narrowing and annular fissure at C6–7 level.

Fig. 3.
X-ray showing anteriorposterior (A) and lateral views (B) of the cervical spine prior to cervical arthroplasty.
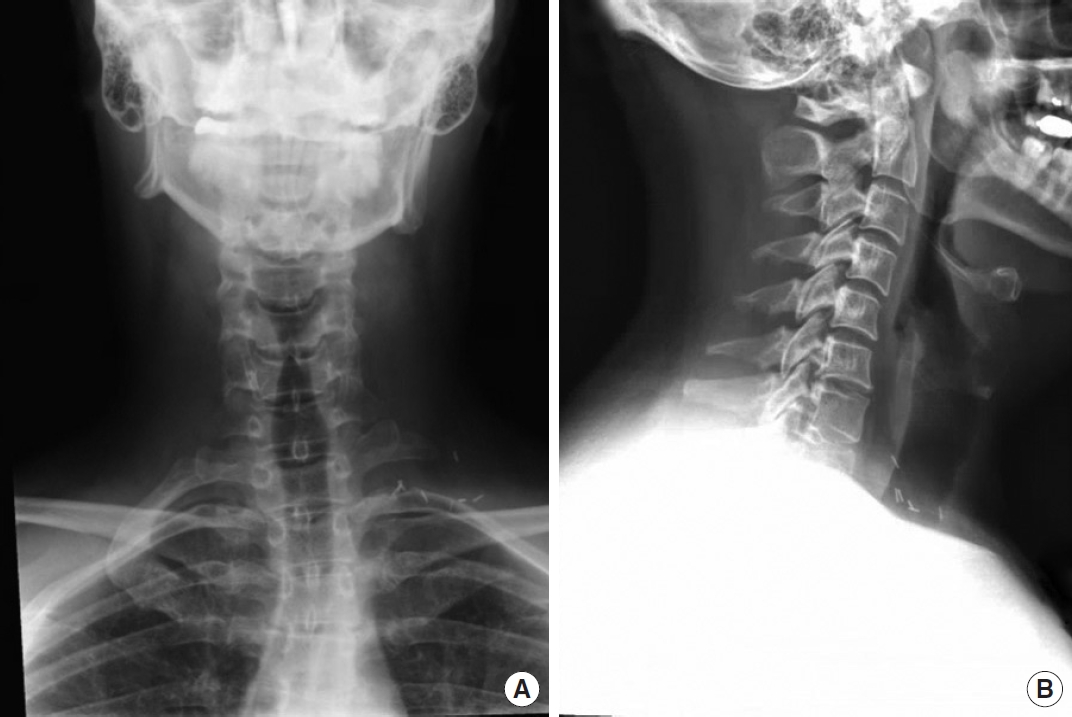
Fig. 4.
X-ray showing dynamic extension (A) and flexion views (B) of the cervical spine prior to cervical arthroplasty.

Fig. 5.
X-ray showing anteriorposterior view of cervical spine. Red arrow points to the left uncinatectomy for full decompression of the foramen.
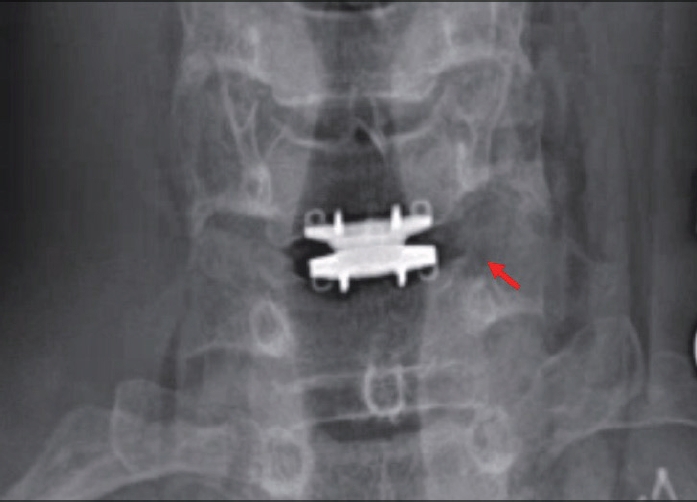
Fig. 6.
X-ray showing anteriorposterior (A) and lateral views (B) of the cervical spine after anterior cervical discectomy and arthroplasty at the C6–7 level.
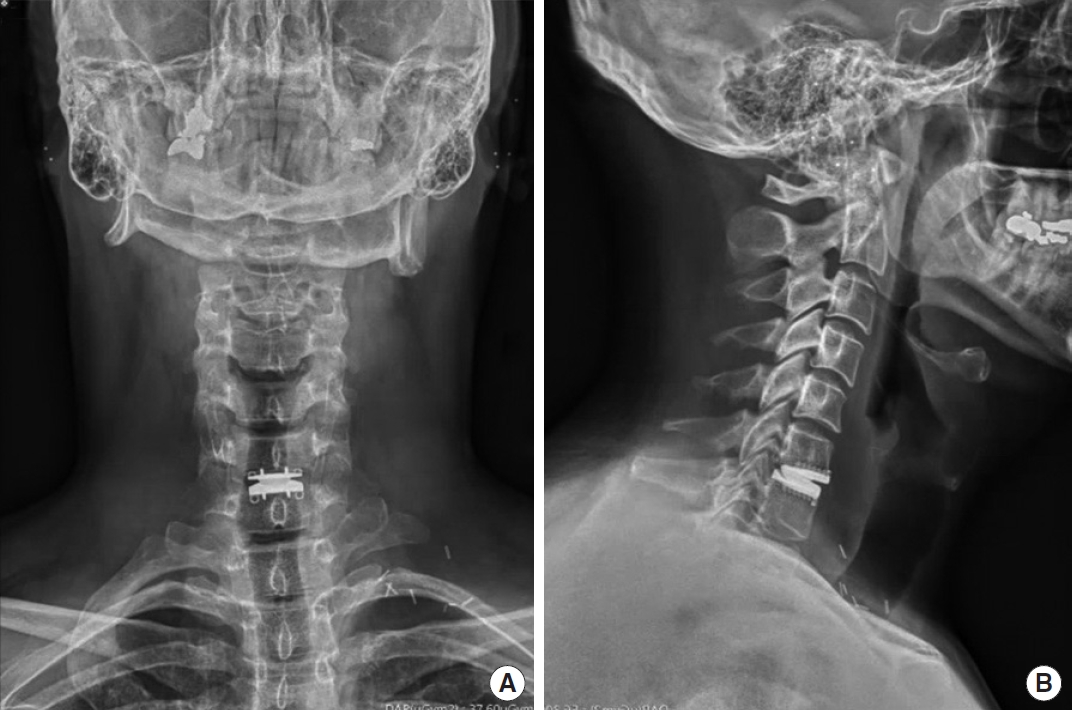
Fig. 7.
X-ray showing dynamic extension (A) and flexion views (B) of the cervical spine after anterior cervical discectomy and arthroplasty at the C6–7 level.

Fig. 8.
PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-analyses) study selection flow diagram.
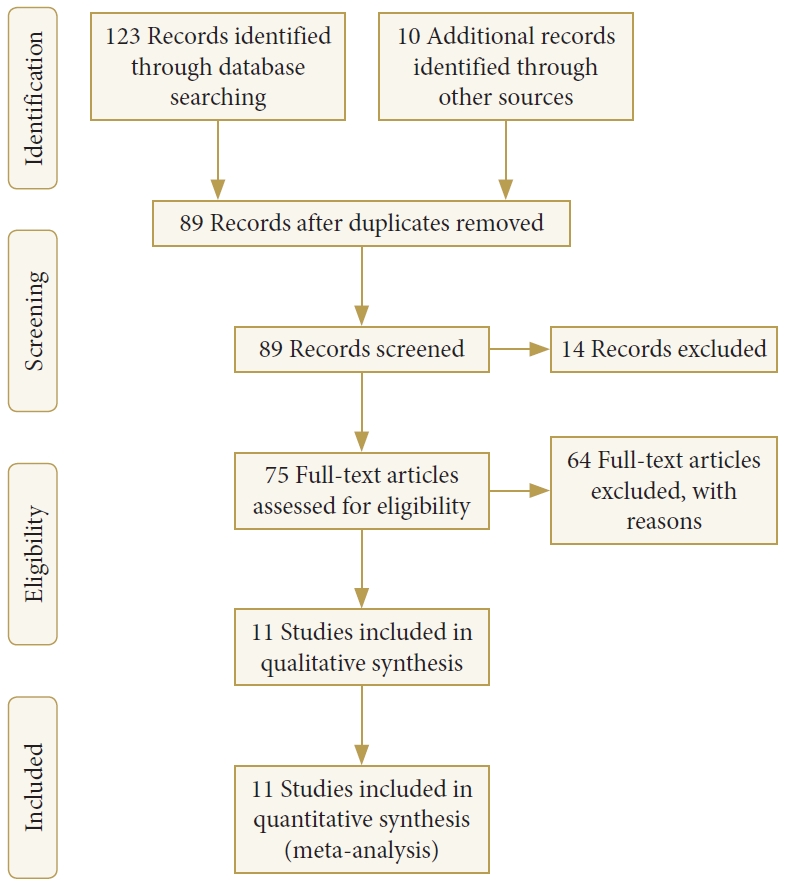
Table 1.
Demographic and clinical variables of included studies
| Study | Year | Study design | Institution | No. | No. of after exclusion criteria | Cervical level | Minors score | Age | Sex | Average symptom duration | Location of pain | Pain improved after surgery? |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Jain and Sharma [27] | 2020 | Retrospective cohort study | SMS Medical College, Jaipur, India | 25 | 8 | C5–8 | 7 | mean: 57.24 (range: 40-84) | 5M, 3F | 4.36 mo | N/A | N/A |
| Ozgur and Marshall [12] | 2003 | Retrospective cohort study | University of California, San Diego, CA, USA | 241 | 39 | C7 | 8 | N/A | N/A | N/A | N/A | Yes |
| Nakajima [8] | 2006 | Retrospective cohort study | University of Fukui, Fukui, Japan | 706 | 6 | C4–5 (1), C5–6 (3), C6–7 (2) | 8 | Mean: 54.5 (range: 36–74) | 6M, 4F | 5.6 mo (range, 2–12 mo) | 1 case had retrosternal pain, three cases had left lower anterior chest pain, and two cases had epigastric pain. | Yes |
| Sussman et al. [3] | 2015 | Retrospective cohort study | Worcester Medical Center, Worcester, MA, USA | 6 | 4 | C5–6 (2), C6–7 (2) | 8 | Range, 39–64 | 3M, 1F | Range, | Left anterior chest (1), substernal (2), unspecified (1) | Yes |
| Brodsky et al. [1] | 1989 | Retrospective cohort study | Hospital for Special Surgery, Cornell University Medical College, New York, NY, USA | 164 | 38 | N/A | 8 | N/A | N/A | 2 d–90 mo | N/A | Yes |
| Htay et al. [22] | 2019 | Case report | Melaka Manipal Medical College (MMMC), Melaka, Malaysia | 1 | 1 | C6–7 | 3 | 53 | F | 11 wk | left-sided chest pain and back pain between the spine and left scapula | N/A |
| Noji et al. [26] | 2017 | Case report | Ashigarakami Kanagawa Prefectural Hospital, Kanagawa, Japan | 1 | 1 | C3–4 | 3 | 78 | F | 1 yr | left chest and back area | Yes |
| Hammad [25] | 2015 | Retrospective cohort study | Al-Azhar University, Cairo, Egypt | 38 | 8 | N/A | 6 | N/A | M2, F6 | N/A | N/A | N/A |
| Tominaga et al. [24] | 2019 | Case report | Kyoto Katsura Hospital, Kyoto, Japan | 1 | 1 | C6–7 | 3 | 42 | M | 1 yr | Anterior chest and upper back pain | Yes |
| Yeung and Hagen [29] | 1993 | Case report | Foothills Medical Centre, Calgary, Canada | 2 | 2 | C6–7 | 3 | 40, 48 | 2F | 10 d | Anterior chest | Yes |
| Grgic [28] | 2008 | Case report | N/A | 1 | 1 | C6–7 | 3 | 41 | F | 6 mo | Anterior chest | N/A |
REFERENCES
1. Brodsky AE. Cervical angina. A correlative study with emphasis on the use of coronary arteriography. Spine (Phila Pa 1976) 1985 10:699-709.


3. Sussman WI, Makovitch SA, Merchant SH, et al. Cervical angina: an overlooked source of noncardiac chest pain. Neurohospitalist 2015 5:22-7.



5. Güler N, Bilge M, Eryonucu B, et al. Acute ECG changes and chest pain induced by neck motion in patients with cervical hernia--a case report. Angiology 2000 51:861-5.


6. Ito Y, Tanaka N, Fujimoto Y, et al. Cervical angina caused by atlantoaxial instability. J Spinal Disord Tech 2004 17:462-5.


7. Nakae Y, Johkura K, Kudo Y, et al. Spinal cord infarction with cervical angina. J Neurol Sci 2013 324:195-6.


8. Nakajima H, Uchida K, Kobayashi S, et al. Cervical angina: a seemingly still neglected symptom of cervical spine disorder? Spinal Cord 2006 44:509-13.



9. Sudo H, Goto R. Cervical angina because of ossification of the posterior longitudinal ligament. Spine J 2012 12:169.


10. Foussas SG, Adamopoulou EN, Kafaltis NA, et al. Clinical characteristics and follow-up of patients with chest pain and normal coronary arteries. Angiology 1998 49:349-54.


11. Mourad G, Alwin J, Strömberg A, et al. Societal costs of noncardiac chest pain compared with ischemic heart disease--a longitudinal study. BMC Health Serv Res 2013 13:403.




12. Ozgur BM, Marshall LF. Atypical presentation of C-7 radiculopathy. J Neurosurg 2003 99(2 Suppl):169-71.


14. Slim K, Nini E, Forestier D, et al. Methodological index for non-randomized studies (minors): development and validation of a new instrument. ANZ J Surg 2003 73:712-6.


15. Chen Y, Huang Z, Fang X, et al. Diagnosis and treatment of mycoplasmal septic arthritis: a systematic review. Int Orthop 2020 44:199-213.



16. Iwasa M. Clinical analysis of angina pectoris and angina-like pain --With special reference to ECG during attack, “cervical spondylosis” and selective coronary arteriography. Jpn Circ J 1976 40:1191-203.


18. Cheshire WP Jr. Spinal cord infarction mimicking angina pectoris. Mayo Clin Proc 2000 75:1197-9.


20. González-Darder JM, Canela P, González-Martinez V. High cervical spinal cord stimulation for unstable angina pectoris. Stereotact Funct Neurosurg 1991 56:20-7.


21. LaBan MM, Meerschaert JR, Taylor RS. Breast pain: a symptom of cervical radiculopathy. Arch Phys Med Rehabil 1979 60:315-7.

22. Htay MN, Ni H, Moe S. Cervical spondylosis mimicking cardiac angina. J Case Rep Images Med 2019 5:100050Z09-MH2019.
23. Eleraky MA, Apostolides PJ, Dickman CA, et al. Herniated thoracic discs mimic cardiac disease: three case reports. Acta Neurochir (Wien) 1998 140:643-6.



24. Tominaga T, Nishimura R, Fujita H, et al. Acute anterior chest and back pain due to cervical disc herniation without radiculopathy: a case report. Case Rep Imag Surg 2019 2:1-3.

25. Hammad WA. Pseudo-angina syndrome: a prospective diagnostic study. Al-Azhar Assiut Med J 2015 13(Suppl 2):9-12.
26. Noji M, Inagaki H, Endo S, et al. Cervical angina of high cervical disc hernia. Spinal Surg 2017 31:80-6.

27. Jain RS, Sharma JK. Cervical angina: an unnoticed cause of noncardiac chest pain. Indian J Clin Pract 2020 30:836-8.
28. Grgic V. Cervicogenic angina. Chest pain caused by unrecognized disc herniation at the segment c6-c7: a case report. Lijec Vjesn 2008 130:234-6.

29. Yeung MC, Hagen NA. Cervical disc herniation presenting with chest wall pain. Can J Neurol Sci 1993 20:59-61.


30. Coric D, Guyer RD, Nunley PD, et al. Prospective, randomized multicenter study of cervical arthroplasty versus anterior cervical discectomy and fusion: 5-year results with a metal-on-metal artificial disc. J Neurosurg Spine 2018 28:252-61.


31. Gao F, Mao T, Sun W, et al. An updated meta-analysis comparing artificial cervical disc arthroplasty (CDA) versus anterior cervical discectomy and fusion (ACDF) for the treatment of cervical degenerative disc disease (CDDD). Spine (Phila Pa 1976) 2015 40:1816-23.



- TOOLS



























