 |
 |
- Search
|
|
||
Abstract
Objective
Spinopelvic parameters play important roles in clinical outcomes and disability after short-segment fusion surgery for degenerative spine disease. This study aimed to investigate the relationship between preoperative or postoperative spinopelvic parameters and symptomatic adjacent segment degeneration (ASD) after single-level anterior lumbar interbody fusion (ALIF) surgery at the L4–5 segments.
Methods
All patients who underwent single-level ALIF at the L4–5 level from January 2010 to December 2013 and were followed up for 5 years were analyzed. We collected the degree of degeneration at adjacent segments and preoperative and postoperative spinopelvic parameters. We compared the preoperative and postoperative parameters between patients with and without symptomatic ASD.
Results
Sixty-one patients were included in our study, and 30 patients had symptomatic ASD. Degeneration at adjacent segments and preoperative spinopelvic parameters did not affect the occurrence of symptomatic ASD. Patients with symptomatic ASD had higher postoperative pelvic tilt (PT) and a mismatch between lumbar lordosis (LL) and pelvic incidence (PI) compared to those without. Postoperative PT > 15° and PI–LL mismatch > 10° were significant risk factors for symptomatic ASD.
Although the use of segmental motion-preserving spine surgery has increased recently, spinal fusion surgery still remains an important method of standard surgical treatments for degenerative spinal disease [1]. Improvements in the fusion rate and clinical outcome have been increasing because of the development of spinal instruments and bone grafts, such as demineralized bone matrix and bone morphogenetic protein [1]. However, an abnormal spinal biomechanical phenomenon occurs in adjacent segments and vertebral bodies, which accelerates the degeneration of the disc or facet joint at the adjacent segments [2]. These changes in biomechanical forces are called adjacent segment disease (ASD) [2]. A recent systematic review article by Xia et al. [3] reported that the rate of ASD after spinal interbody fusion ranged from 4.8% to 92.9%. According to previous articles, the risk factors of ASD after lumbar fusion surgery included age, sex, body mass index, preexisting disc degeneration, the degree of facet degeneration, number of fused levels, and lower lordotic curves of fused segments [4-7]. Recent studies have highlighted the importance of spinopelvic parameters in the occurrence of ASD [8,9]. Other studies showed that spinopelvic sagittal malalignment may contribute to the occurrence of ASD [10-13]. However, most of these studies dealt with the relationship between spinopelvic parameters and ASD in posterior approach spinal fusion surgery, such as posterior lumbar interbody fusion (PLIF) and transforaminal lumbar interbody fusion (TLIF), at various vertebral levels.
The present study aimed to reveal the relationship between spinopelvic parameters and ASD after single-level anterior lumbar interbody fusion (ALIF) surgery. Our study only included patients with degenerative spinal disease at the L4–5 level who underwent single-level ALIF surgery to exclude other variables.
The study design was approved by the Institutional Review Board (IRB) of Busan Wooridul Spine Hospital (IRB No. WRDIRB-2019-07-007) in September 2019, and written informed consent was obtained from all the participants.
We performed this retrospective case-control study to analyze the relationship between spinopelvic parameters and the occurrence of ASD after single-level ALIF surgery. We reviewed the medical records and radiologic examinations of all patients who underwent elective single-level ALIF performed by HCL from January 2010 to December 2013. The inclusion criteria were as follows: (1) single-level ALIF at the L4–5 level, (2) follow-up over 5 years, (3) fusion for degenerative lumbar disease, and (4) radiologic examination performed 5 years after the operation. Patients were excluded if they had scoliosis (Cobb angle > 20°) or underwent surgery for trauma or infection.
Patients were divided into an ASD group or a control group. The ASD group was defined as those who met the following 3 criteria: (1) newly developed lower back pain, claudication, and radiating pain 6 months after the symptoms were relieved after the previous operation, (2) newly developed instability (spondylolisthesis or dynamic instability with slippage more than 4 mm and/or angle change more than 10 degrees on flexion and extension) of adjacent segments, (3) the patients who underwent additional surgery in the adjacent segments.
Our study analyzed the known risk factors for ASD (age, body mass index, osteoporosis, preoperative facet, and disc degeneration, coronal wedge, vacuum disc, and spondylolisthesis). The preoperative degree of adjacent disc degeneration on magnetic resonance imaging was classified according to the Pfirrmann et al. [14] grading system, and facet joint degeneration on computed tomography (CT) was rated from grade 0 to grade 3 using Weishaupt classification system [15]. A positive coronal wedge was defined as > 5° of tilt between the inferior margin of the upper vertebral body and the superior bone margin at the lower vertebral body. The presence of air in the adjacent segmental disc on the CT scan was defined as a vacuum disc. Spondylolisthesis was defined as > 3 mm anterior or posterior vertebral slip on standing lateral radiographs.
Simple plain radiography films of the lumbar spine, including the femoral head, were obtained for all patients before and after surgery. We measured the composition of spinopelvic parameters, including the pelvic incidence (PI), sacral slope (SS), pelvic tilt (PT), lumbar lordosis (LL), segmental lordosis, and disc height at the L4–5 level in all patients before and after surgery. We calculated the difference between PI and LL (PILL= PI–LL) and the height at the operative level on the preoperative and postoperative films. To evaluate the lumbar sagittal alignment according to the reciprocal uppermost lumbar vertebral position change in the sagittal plane after single-level fusion of the L4/5 level, we used the L1 axis S1 distance, which is the distance from the L1 plumb line to the posterior corner of the first sacral body, in all patients before and after surgery.
The demographic and radiologic factors regarding the risks of ASD were compared between the 2 groups and within the groups using the Student t-test for continuous values and the chi-square test for categorized values. All statistical analyses were performed using SPSS ver. 12.0 (SPSS Inc., Chicago, IL, USA). Statistical significance was set at p< 0.05.
Of the 61 patients enrolled in our study, 43 patients had degenerative spondylolisthesis, 11 patients had foraminal stenosis, 6 patients had central spinal stenosis, and 1 patient had lumbar disc herniation. Mean patient ages at the time of operation were 61.42 ± 8.44 years (range, 45–77 years). The mean follow-up period was 70.16 ± 11.59 months (range, 60–101 months). Thirty patients were classified into the ASD group according to our criteria. In the ASD group, 13 patients had ASD at the L3–4 segment, and the remaining patients had ASD below that level. Demographic characteristics did not differ between the groups.
There were no significant differences in the grade of the adjacent facet joint and disc degeneration, frequency of vacuum discs, wedge deformity, spondylolisthesis, and retrolisthesis between the groups (Table 1).
In the ASD group, LL, the segmental angle, and disc height at the fused level and PI–LL mismatch were significantly improved after surgery. In the non-ASD group, LL, the fused segmental angle, disc height, and PI–LL mismatch improved similarly. The PT and L1 sagittal vertical axis decreased while the SS increased after fusion in the non-ASD group (Table 2).
There were no significant differences in the preoperative parameters between the groups. The segmental angle at the L4–5 disc level was higher in the ASD group than in the non-ASD group (4.06± 3.96 and 1.52± 5.89, respectively; p= 0.060), but the difference was not statistically significant.
Regarding the postoperative radiologic parameters, the PT was higher (21.10± 10.80 vs. 14.94± 8.76, p= 0.017) and the incidence of PT > 15° was higher in the ASD group than in the non-ASD group (22 patients [73.3%] vs. 12 patients [45.2%], p= 0.037). The postoperative values of LL and PI were not different between the groups. However, the PI–LL mismatch was higher in the ASD group than in the non-ASD group (10.36± 16.12 vs. 3.94 ± 10.37, p = 0.069), and the incidence of PI–LL mismatch > 10° was significantly higher in the ASD group than in the non- ASD group (21 patients [70%] vs. 9 patients [29.0%], p= 0.002) (Table 3).
We investigated the risk factors for ASD after single-level ALIF surgery. The results of our study revealed 2 factors, one was high postoperative PT and the other was a large mismatch between LL and PI. ASD is the most significant complication affecting the long-term outcome after lumbar fusion [6]. The incidence of ASD after lumbar fusion has been investigated in many studies. Sears et al. [16] reported that the incidence of ASD requiring reoperation after lumbar fusion was 22.2%, and the prevalence per year was 2.5% over 10 years. In Ghiselli et al.’s study [17], the incidence of ASD after lumbar surgery was 36.1% at 10 years postoperatively, the 27.4% of patients who underwent lumbar surgery required reoperation at adjacent segments. In our study, the incidence of symptomatic ASD was 49.1%, and the rate of reoperation was 21.3%. It is controversial whether the presence of degenerative discs in adjacent segments has an effect on increasing the incidence of ASD. Edwards et al. [18] reported that degeneration of the adjacent segment was a risk factor for the occurrence of ASD in 34 patients who underwent thoracolumbar fusion and were followed up for an average of 5.6 years. However, many other authors reported that the degeneration of adjacent segments did not affect the incidence of ASD [1,4,15,17]. In particular, Ghiselli et al. [17], who included 215 patients who underwent a revision surgery at adjacent segments after lumbar fusion, found no relationship between the occurrence of ASD and adjacent segment degeneration. In our study, degeneration at the adjacent disc level did not affect the incidence of ASD. The effect of preoperative facet degeneration on ASD is also controversial. Two articles reported that the presence of facet arthropathy at the adjacent segment affected the occurrence of ASD [1,19]. In contrast, Kaito et al. [4] reported that facet degeneration did not affect the occurrence of ASD. Our study showed that facet degeneration had no effect on the occurrence of ASD. Therefore, further studies are needed to identify the effect of facet degeneration at the adjacent level on the occurrence of ASD. Some studies have reported that mismatches in sagittal spinopelvic parameters play important roles in the occurrence of postoperative ASD after lumbar fusion surgery [9,11,12]. Kumar et al. [12] revealed that an abnormal C7 costovertebral angle preoperatively and SS play significant roles in the occurrence of ASD after lumbar fusion. Other articles reported that preoperative PT > 20° and SS < 40° affected the incidence of ASD [11]. Matsumoto et al. [10] reported that a low LL and high PT preoperatively were important risk factors for the high incidence of ASD after single-level PLIF surgery. In contrast, our study showed that preoperative spinopelvic parameters were not associated with the incidence of symptomatic ASD after single-level ALIF surgery. Therefore, we believe that the effects of preoperative abnormal spinopelvic parameters on postoperative ASD need to be investigated in high-quality studies.
Many studies have investigated the relationship between ASD and LL or PI [20,21]. Djurasovic et al. [20] reported that patients with less LL had more ASD after lumbar fusion. Nakashima et al. [21] revealed that a low PI was a significant risk factor for developing ASD after fusion. However, these studies did not suggest ideal LL and PI because these ideal values are individual, making them difficult to determine. In our study, preoperative or postoperative LL and PI did not affect ASD development after single-level ALIF surgery. Some studies have reported that the balance between PI and LL affects the incidence of ASD. The balance between LL and PI has been used in adult spinal deformity surgeries, and the mismatch between LL and PI was correlated with disability and low patient-reported outcome measures [22]. A study by Senteler et al. [23] that used biomechanical models reported that the mismatch between LL and PI had a tendency to increase segmental axial loadings in unfused and fused lumbar spines. The first study about the effect of PI–LL mismatch on ASD was reported by Rothenfluh et al. [24]. This study included patients who underwent lumbar fusion surgery from 1 to 3 segments and reported that a higher mismatch between PI and LL had more effects on the occurrence of ASD. Matsumoto et al. [10] included only single-level PLIF surgery and reported that spinopelvic imbalance (PI–LL mismatch ≥ 10°) was the most important risk factor for ASD. Tempel et al. [25] suggested that a high PI–LL mismatch had a meaningful relationship with the development of symptomatic ASD in single-level TLIF surgery. They proposed that the positive cutoff value for the development of symptomatic ASD was PI–LL mismatch > 11° [25]. In our study, the postoperative mismatch between PI and LL was a significant risk factor for symptomatic ASD after single-level ALIF surgery. Our cutoff value of postoperative PI–LL mismatch for symptomatic ASD was > 10°. The association between LL and PI mismatch and ASD occurrence is thought to be influenced by the following. The mismatch between PI and LL after single-level ALIF is caused by the insufficient restoration of LL. In this situation, the L1 SVA increases as the proximal lumbar spine move to the ventral side from the sagittal view of the lumbar spine. As the L1 SVA increases, the loading axis of the lumbar spine leans forward, increasing the ventral bending force throughout the lumbar spine. Due to the increased ventral bending force, the segmental axial loading of the adjacent segment is further increased and the tensile force on the posterior element is increased, which can promote degenerative changes of the disc and facet of the adjacent segment (Fig. 1). As a retrospective study, our study has limitations. We believe that the high incidence of ASD in our study was due to a selection bias. There is a possibility that patients with good outcomes after surgery did not visit the hospital anymore, which may cause selection bias. One hundred ten patients underwent ALIF surgery at the L4–5 level from January 2010 to December 2013, but only 61 patients (55.4%) were followed up for more than 5 years. Second, the PI values of patients are widely distributed, and the characteristics of the correlation with LL or PT may differ depending on the range of PI values [26]. But in our study, additional research could not be conducted due to the small number of the patients. If analysis according to this PI distribution is added in the future, more clear results could be derived. Various methods are tried to prevent ASD. When performing long-segment fusion, a hook is used in the most proximal or distal transverse process or lamina, and there is also an attempt to use an additional polyetheretherketone rod in the upper instrumented vertebra [27]. However, not only the use of these additional instruments but also obtaining an appropriate spinopelvic parameter, as shown in the studies mentioned above, is important for postoperative disability and quality of life after spinal fusion surgery. In degenerative spinal disease, the spinal surgeon should consider the patient’s symptoms, neurological examination findings, and correlative radiologic examination results when performing surgery or choosing the method of operation. If the surgeon chooses fusion surgery, the patient’s spinopelvic parameters and sagittal alignment should be considered. In particular, the segmental angle of the cage was the only parameter that affected postoperative LL, and the surgeon at our hospital selected an adequate angle for cage insertion to avoid a mismatch between the PI and LL.
This study investigated the association between symptomatic ASD after single-level ALIF surgery and spinopelvic parameters. Preoperative spinopelvic parameters did not affect the development of symptomatic ASD. Postoperative high PT and PI–LL mismatch were significant risk factors for symptomatic ASD after single-level ALIF surgery. The results of this study suggest that PI–LL mismatch should be avoided by achieving a proper LL even when performing single-level fusion.
NOTES
Fig. 1.
Reciprocal changes of lumbar lordosis after single-level fusion. (A) Proper PI and LL relationship is achieved after single-level fusion. (B) PI–LL is mismatched due to inappropriate segmental angle of the L4/5 after single-level fusion. Note that upper lumbar vertebrae are ventrally placed. PI, peIvic incidence; LL, lumbar lordosis.
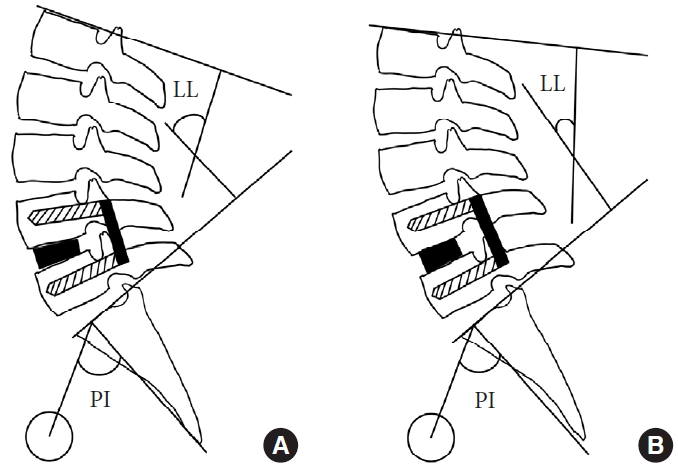
Table 1.
Baseline characteristics and preexisting degenerative pathologies
| Characteristic | ASD (n = 30) | Non-ASD (n = 31) | p-value |
|---|---|---|---|
| Sex | 0.934 | ||
| Male | 9 (30) | 9 (29) | |
| Female | 21 (70) | 22 (71) | |
| Age (yr) | |||
| Mean± SD | 59.6 ± 8.5 | 63.2 ± 8.1 | 0.091 |
| Range (IQR) | 54.3–66.0 | 55.0–70.0 | |
| BMI | |||
| Mean± SD | 24.0 ± 3.8 | 23.9 ± 2.3 | 0.868 |
| Range (IQR) | 22.6–25.6 | 21.9–25.0 | |
| Follow-up | |||
| Mean± SD | 68.5 ± 11.1 | 71.8 ± 12.0 | 0.264 |
| Range (IQR) | 59.0–75.3 | 62.0–81.0 | |
| Smoking | 3 (10.0) | 4 (12.9) | > 0.999 |
| Post decompression | 20 (66.7) | 24 (77.4) | 0.402 |
| Disease (index level) | 0.161 | ||
| DS | 20 (66.7) | 23 (74.2) | |
| FS | 7 (23.3) | 4 (12.9) | |
| CS | 2 (6.7) | 4 (12.9) | |
| DH | 1 (3.8) | 0 (0) | |
| Disease (adjacent level) | |||
| L3–4 segment | n= 13 | n= 48 | |
| Disc degeneration* | 0.238 | ||
| Grade 2 | 1 (7.7) | 2 (4.2) | |
| Grade 3 | 2 (15.4) | 20 (41.7) | |
| Grade 4 | 10 (76.9) | 25 (52.1) | |
| Grade 5 | 0 (0) | 1 (2.1) | |
| Facet degeneration† | 0.290 | ||
| Grade 0 | 3 (23.1) | 22 (45.8) | |
| Grade 1 | 7 (53.8) | 21 (43.8) | |
| Grade 2 | 2 (15.4) | 3 (6.3) | |
| Grade 3 | 1 (7.7) | 2 (4.2) | |
| Vacuum disc | 4 (30.8) | 12 (25.0) | 0.728 |
| Wedge deformity‡ | 1 (7.7) | 6 (12.5) | 0.999 |
| Spondylolisthesis§ | 0.756 | ||
| Anterior | 0 (0) | 1 (2.1) | |
| Retro | 3 (23.1) | 8 (16.7) | |
| L5-S1 segment | n= 21 | n= 40 | |
| Disc degeneration* | 0.709 | ||
| Grade 2 | 2 (9.5) | 9 (7.5) | |
| Grade 3 | 4 (19.0) | 12 (30.0) | |
| Grade 4 | 14 (66.7) | 21 (52.5) | |
| Grade 5 | 1 (4.8) | 4 (10.0) | |
| Facet degeneration† | 0.547 | ||
| Grade 0 | 11 (52.4) | 21 (52.5) | |
| Grade 1 | 9 (42.9) | 17 (42.5) | |
| Grade 2 | 0 (0) | 2 (5.0) | |
| Grade 3 | 1 (4.8) | 0 (0) | |
| Vacuum disc | 12 (57.1) | 14 (35.5) | 0.097 |
| Wedge deformity‡ | 0 (0) | 0 (0) | > 0.999 |
| Spondylolisthesis§ | 0.533 | ||
| Anterior | 1 (4.8) | 0 (0) | |
| Retro | 1 (4.8) | 3 (7.5) |
Values are presented as number (%) unless otherwise indicated.
ASD, adjacent segment disease; SD, standard deviation; IQR, interquartile range; BMI, body mass index; DS, degenerative spondylolisthesis; FS, foraminal stenosis; CS, central spinal stenosis; DH, lumbar disc herniation.
Chi-square test and Student t-test were used for statistical analysis.
Table 2.
Preoperative and postoperative spinopelvic parameters in ASD and non-ASD groups
| Variable |
ASD (n = 30) |
Non-ASD (n = 31) |
||||
|---|---|---|---|---|---|---|
| Preoperative | Postoperative | p-value | Preoperative | Postoperative | p-value | |
| PeIvic incidence (PI) | 55.34 ± 11.85 | 55.33 ± 11.85 | 0.999 | 52.56 ± 11.25 | 52.64 ± 11.26 | 0.310 |
| Pelvic tilt | 22.16 ± 10.14 | 21.10 ± 10.80 | 0.294 | 19.04 ± 8.76 | 14.94 ± 8.76 | 0.006* |
| Sacral slope | 33.16 ± 9.38 | 34.23 ± 7.82 | 0.294 | 33.51 ± 8.99 | 37.61 ± 7.68 | 0.006* |
| Lumbar lordosis (LL) | 40.63 ± 15.30 | 44.96 ± 12.08 | 0.039* | 39.67 ± 14.45 | 48.61 ± 10.20 | < 0.001* |
| Segmental angle | 4.06 ± 3.96 | 10.78 ± 3.21 | < 0.001* | 1.52 ± 5.89 | 10.62 ± 3.27 | < 0.001* |
| PI–LL | 14.07 ± 16.14 | 10.36 ± 16.12 | 0.039* | 12.89 ± 13.67 | 3.94 ± 10.37 | 0.004* |
| L1 SVA (mm) | 24.86 ± 21.84 | 18.30 ± 22.49 | 0.124 | 27.90 ± 24.57 | 18.88 ± 17.76 | < 0.001* |
| Disc height (mm) | 8.58 ± 2.55 | 13.98 ± 1.85 | < 0.001* | 7.74 ± 2.57 | 13.48 ± 1.60 | < 0.001* |
Table 3.
Differences of spinopelvic parameters between ASD and non-ASD groups
| Variable |
Preoperative |
Postoperative |
||||
|---|---|---|---|---|---|---|
| ASD (n=30) | Non-ASD (n=31) | p-value | ASD (n = 30) | Non-ASD (n = 31) | p-value | |
| PeIvic incidence (PI) | 55.34 ± 11.85 | 52.56 ± 11.25 | 0.353 | 55.33 ± 11.85 | 52.64 ± 11.26 | 0.511 |
| Pelvic tilt (PT) | 22.16 ± 10.14 | 19.04 ± 8.76 | 0.203 | 21.10 ± 10.80 | 14.94 ± 8.76 | 0.017* |
| PT > 15 | 22 (73.3) | 22 (71.0) | > 0.999 | 22 (73.3) | 14 (45.2) | 0.037* |
| Sacral slope | 33.16 ± 9.38 | 33.51 ± 8.99 | 0.882 | 34.23 ± 7.82 | 37.61 ± 7.68 | 0.094 |
| Lumbar lordosis (LL) | 40.63 ± 15.30 | 39.67 ± 14.45 | 0.801 | 44.96 ± 12.08 | 48.61 ± 10.20 | 0.207 |
| Segmental angle | 4.06 ± 3.96 | 1.52 ± 5.89 | 0.060 | 10.78 ± 3.21 | 10.62 ± 3.27 | 0.849 |
| PI–LL | 14.07 ± 16.14 | 12.89 ± 13.67 | 0.638 | 10.36 ± 16.12 | 3.94 ± 10.37 | 0.069 |
| PI–LL > 10 | 22 (73.3) | 23 (74.2) | > 0.999 | 21 (70.0) | 9 (29.0) | 0.002* |
| L1 SVA (mm) | 24.86 ± 21.84 | 27.90 ± 24.57 | 0.612 | 18.30 ± 22.49 | 18.88 ± 17.76 | 0.912 |
| Disc height (mm) | 8.58 ± 2.55 | 7.74 ± 2.57 | 0.205 | 13.98 ± 1.85 | 13.48 ± 1.60 | 0.258 |
REFERENCES
1. Lee CS, Hwang CJ, Lee SW, et al. Risk factors for adjacent segment disease after lumbar fusion. Eur Spine J 2009;18:1637-43.




2. Yamasaki K, Hoshino M, Omori K, et al. Risk factors of adjacent segment disease after transforaminal inter-body fusion for degenerative lumbar disease. Spine 2016;2:E86-92.

3. Xia XP, Chen HL, Cheng HB, et al. Prevalence of adjacent segment degeneration after spine surgery: a systematic review and metaanalysis. Spine (Phila Pa 1976) 2013;38:597-608.

4. Kaito T, Hosono N, Mukai Y, et al. Induction of early degeneration of the adjacent segment after posterior lumbar interbody fusion by excessive distraction of lumbar disc space. J Neurosurg Spine 2010;12:671-9.


5. Lee JC, Kim Y, Soh JW, et al. Risk factors of adjacent segment disease requiring surgery after lumbar spinal fusion: comparison of posterior lumbar interbody fusion and posterolateral fusion. Spine (Phila Pa 1976) 2014;39:E339-45.

6. Okuda S, Oda T, Miyauchi A, et al. Lamina horizontalization and facet tropism as the risk factors for adjacent segment degeneration after PLIF. Spine (Phila Pa 1976) 2008;33:2754-8.


7. Park P, Garton HJ, Gala VC, et al. Adjacent segment disease after lumbar or lumbosacral fusion: review of the literature. Spine (Phila Pa 1976) 2004;29:1938-44.


8. Dohzono S, Toyoda H, Matsumoto T, et al. The influence of preoperative spinal sagittal balance on clinical outcomes after microendoscopic laminotomy in patients with lumbar spinal canal stenosis. J Neurosurg Spine 2015;23:49-54.


9. Le Huec JC, Faundez A, Dominguez D, et al. Evidence showing the relationship between sagittal balance and clinical outcomes in surgical treatment of degenerative spinal diseases: a literature review. Int Orthop 2015;39:87-95.



10. Matsumoto T, Okuda S, Maeno T, et al. Spinopelvic sagittal imbalance as a risk factor for adjacent-segment disease after single-segment posterior lumbar interbody fusion. J Neurosurg Spine 2017;26:435-40.


11. Di Martino A, Quattrocchi CC, Scarciolla L, et al. Estimating the risk for symptomatic adjacent segment degeneration after lumbar fusion: analysis from a cohort of patients undergoing revision surgery. Eur Spine J 2014;23:693-8.



12. Kumar MN, Baklanov A, Chopin D. Correlation between sagittal plane changes and adjacent segment degeneration following lumbar spine fusion. Eur Spine J 2001;10:314-9.




13. Park P, Garton HJ, Gala VC, et al. Adjacent segment disease after lumbar or lumbosacral fusion: review of the literature. Spine (Phila Pa 1976) 2004;29:1938-44.


14. Pfirrmann CWA, Metzdorf A, Zanetti M, et al. Magnetic resonance classification of lumbar intervertebral disc degeneration. Spine 2001;26:1873-8.


15. Weishaupt D, Zanetti M, Boos N, et al. MR imaging and CT in osteoarthritis of the lumbar facet joints. Skeletal Radiol 1999;28:215-9.



16. Sears WR, Sergides IG, Kazemi N, et al. Incidence and prevalence of surgery at segments adjacent to a previous posterior lumbar arthrodesis. Spine J 2011;11:11-20.


17. Ghiselli G, Wang JC, Bhatia NN, et al. Adjacent segment degeneration in the lumbar spine. J Bone Joint Surg Am 2004;86:1497-503.


18. Edwards CC 2nd, Bridwell KH, Patel A, et al. Thoracolumbar deformity arthrodesis to L5 in adults: the fate of the L5- S1 disc. Spine (Phila Pa 1976) 2003;28:2122-31.


19. Okuda S, Iwasaki M, Miyauchi A, et al. Risk factors for adjacent segment degeneration after PLIF. Spine (Phila Pa 1976) 2004;29:1535-40.


20. Djurasovic MO, Carreon LY, Glassman SD, et al. Sagittal alignment as a risk factor for adjacent level degeneration: a case-control study. Orthopedics 2008;31:546.

21. Nakashima H, Kawakami N, Tsuji T, et al. Adjacent segment disease after posterior lumbar interbody fusion: based on cases with a minimum of 10 years of follow-up. Spine (Phila Pa 1976) 2015;40:E831-41.

22. Schwab FJ, Blondel B, Bess S, et al. Radiographical spinopelvic parameters and disability in the setting of adult spinal deformity: a prospective multicenter analysis. Spine (Phila Pa 1976) 2013;38:E803-12.

23. Senteler M, Weisse B, Snedeker JG, et al. Pelvic incidence-lumbar lordosis mismatch results in increased segmental joint loads in the unfused and fused lumbar spine. Eur Spine J 2014;23:1384-93.



24. Rothenfluh DA, Mueller DA, Rothenfluh E, et al. Pelvic incidence-lumbar lordosis mismatch predisposes to adjacent segment disease after lumbar spinal fusion. Eur Spine J 2015;24:1251-8.



25. Tempel ZJ, Gandhoke GS, Bolinger BD, et al. The influence of pelvic incidence and lumbar lordosis mismatch on development of symptomatic adjacent level disease following single-level transforaminal lumbar interbody fusion. Neurosurgery 2017;80:880-6.































