INTRODUCTION
Intraspinal synovial cysts are reported with increasing frequency in the literature but continue to be an uncommon cause of radicular pain9). These cysts have intraspinal and extradural location and originate from the facet capsules caused by degeneration of the facet joints, being therefore known as synovial, juxtafacet, ganglion, or ligamentum flavum cysts3). Incidentally, can be diagnosed during pain when the investigations are located in the spine and/or due to myeloradicular symptoms; now they are more easily diagnosed through magnetic resonance imaging (MRI)1). This enables accurate preoperative planning and avoidance of therapeutic pitfalls. The SC of the thoracolumbar spine is infrequent and the world literature shows a shortage of documented cases. This fact collaborates with the aim of this study, presentation of a case of SC in a middle aged patient, occurring in the thoracolumbar spine and developing progressively compressive symptoms and successfully treated by surgical excision.
CASE REPORT
A 34 years-old lady was admitted with a chief complain of weakness in the left lower limb which had started six months earlier. In the beginning she felt an intermittent weakness, mainly in the left, that interfered in the daily activities. The weakness was progressive, followed by cramps, tingling and interfering in the gait. No alteration of anal and vesical sphincter function. The general examination showed good overall state. The patient was alert, lucid and guided, but with depressed humor. Vital signs were normal. The cardio-respiratory system and the abdomen did not show any alteration during examination. Neurological examination showed: asymmetrical paraparesis (L>R); moderate hypertonia (L>R); increased deep tendon reflexes in the lower limbs. Bilateral Babinski sign showed more evident on left side. Decreased kinetic-postural sensibility were detected in the lower limbs; no involvement of cranial nerves.
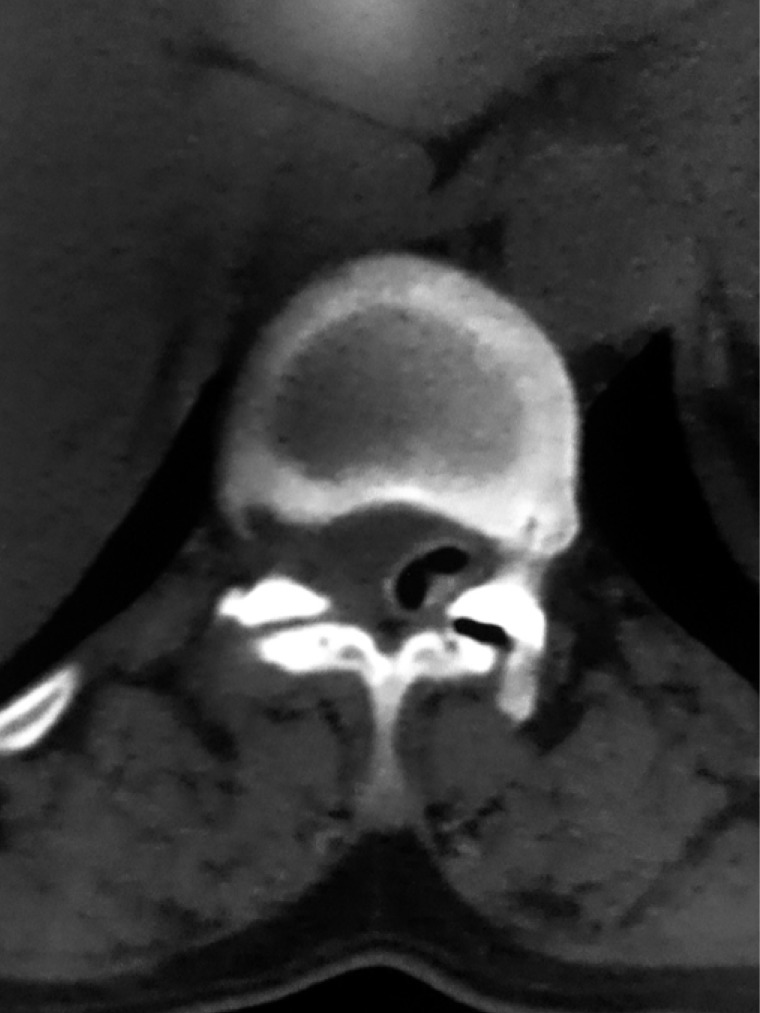
Laboratory tests (complete blood count, biochemical study, electrolytes, urine summary) were normal; MRI of the thoracolumbar spine showed image of cystic aspect of extradural location in T12-L1, hypointense on the T1-weighted sequence and hyperintense on T2-weighted sequence (Fig. 1). Surgical treatment was indicated and a laminectomy accomplished at T12-L1 level, where an extradural cystic tumor was found with posterolateral left location adherent at T12-L1 level. Axial computed tomography (CT) scan showed at same level showed degenerative changes in left facet joint and adjacent cyst (Fig. 2).
The cyst was removed as shown in Fig. 3, the capsule was completely removed and sent for histopathology study which showed cystic formation with thin fibrous walls covered by pavimentous cells in the internal surface; presence of thin perivascular inflammatory infiltrate, compatible with synovial cyst (Fig. 3). Postoperatively the patient showed signs of clinical improvement in terms of decreased pain and paraesthesias. One month later the patient started walking without any assistance.
DISCUSSION
Spinal SC was initially described in 19748). In that study the authors presented a case of SC of the cervical spine operated with success and confirmed by histopathological study. Other authors have reported the presence of this pathology in different locations of the spine. The largest incidence was in the lumbar followed by cervical and less frequently in the thoracic spine. Most of the studied cases prevail in the male sex3). The pathological substratum responsible for the development of the spinal SC includes the degeneration and arthrosis of the articulate facets, causing secondary lesion of the joint capsule and formation of hernia of the synovial membrane.
The presence of myxoid degeneration increases the production of hyaluronic acid with proliferation of mesenchymal cells contributing for the emergence and size of the cysts10). Present clinical observation and experimental date, suggest that the mechanical pressure in the articular facet induces the appearance of a cascade of events as follows: upregulations and release of angiopoietin-1, interleukins-1 and 6, platelet-derived growth factor, basic fibroblast growth factor, vascular endothelial growth factor and substance P liberation, resulting in synovial hyperplasia, neovascularization and exudation of fluid, culminating with the formation of the cysts5). This process could be reversible because the synovial proliferation can decrease on withdrawal of mechanical stress, what in some cases promotes the spontaneous reduction of the cysts5).
The spondylolisthesis and the trauma can also be responsible for the emergence of these cysts. The content can be mucinous, with proteinaceous material and sometimes gaseous. They can present calcification focus or old intracystic hemorrhagic signs.
Bleeding can occur by traumatism of the cyst wall due to the abundance in veined structures.
The preferential location of SC is in the great mobility lumbar spine segments followed by the cervical and less frequently in the thoracic spine. A literature review shows the existence of few told cases in the thoracic location. In 2004 Cohen-Godol et al.4), published 9 cases of SC of lower thoracic spine in a total of 16,000 studied and submitted to the decompressive surgery of the spine due degenerative causes among others. And this is postulated that as T10-L1 represents the transitional zone between relatively immobile thoracic spine and highly mobile lumbar segments so among documented thoracic cysts majority fall in this transitional zone. The above mentioned cases correspond to 0.06% of the total and some literature refer that in the period from 1987 to 2004 only 10 cases have been described reaffirming the low incidence of this pathology. With the exception of a case described by Lynn et al.12) in 2000, of a patient with 24 years-old, the average incidence of this pathology is related to patients of age above 70 years-old.
These cysts may extend into the neural recess and cause radiculopathy11). Clinical presentation may include neurogenic claudication resulting from spinal cord compression by a large cyst6). Symptoms are usually ipsilateral to the side of the cyst; occasionally, larger cysts can also cause contralateral radicular symptoms13). MRI is the investigation of choice in these patients. A lumbar facet joint synovial cyst usually appears as a well demarcated epidural mass with contents isointense or hyperintense to cerebrospinal fluid on T1- and T2-weighted fast spin-echo images14). The slight hyperintensity sometimes seen has been attributed to various causes; one possible explanation is that small amounts of paramagnetic blood breakdown products present in the cyst fluid may be responsible7,8). Occasionally, the synovial cysts may appear hypointense on both T1- and T2-weighted images, which is usually caused by solid calcification in the cyst. MRI may occasionally show signal void due to vacuum phenomenon, and in these cases CT is more helpful in revealing the intracystic air1). The rim of the cyst shows high signal intensity on T1-weighted images except when peripheral calcification or hemosiderin deposition is present6,11). In addition, the cyst rim may show enhancement after the administration of gadolinium11). Tillich et al. showed that a communication is always present between the synovial cyst and the facet joint at surgery, but this is seen in only a minority of cases on MRI, which is probably because of the relatively small size of the communication14). The communication enables the filling and emptying of the cyst, which is dependent on the mechanical stresses and postural changes of the spine2,3). This explains the size variations of the cysts on follow-up imaging in some cases1,2,3). Symptomatic facet joint cysts are usually surgically resected13). Our patient underwent L3-L4 medial facetectomy and resection of the cyst. The patient reported significant improvement in the symptoms at out patient review.