Posterior Epidural Herniation of a Lumbar Disk Fragment at L2–3 That Mimicked an Epidural Hematoma
Article information
Abstract
Lumbar disk herniation is common. Because of the posterior longitudinal ligament, migration usually occurs into the ventral epidural space. Rarely, fragments migrate into the dorsal epidural space. A 57-year-old man presented with lower back pain and weakness on right hip flexion and right knee flexion. He had lower back pain 1 day previously and received a transforaminal epidural block at a local hospital. The next day, he reported weakness of the right lower extremity. Lumbar spine magnetic resonance imaging revealed a dorsal epidural lesion with compression of the thecal sac at L2–3. Initial differential diagnoses included epidural hematoma after the block, neoplasm, and a sequestrated disk. Posterior lumbar decompression was performed. The lesion was identified intraoperatively as a large herniated disk fragment. Posterior epidural herniation of a lumbar disk fragment is rare and may be difficult to diagnose preoperatively. It may present as a variety of clinical scenarios and, as in this case, may mimic epidural hematoma.
INTRODUCTION
Herniation of nucleus pulposus derived from disk degeneration is frequent. Disk fragments generally migrate to the anterior epidural space, which is well-defined and delimited by the posterior longitudinal ligament (PLL) and the attached lateral membranes8). Therefore, posterior epidural herniation of a lumbar disk fragment is rare. Only few cases have been reported1,10). The posterior epidural herniation of a disk fragment have a similarity to tumor, hematoma, and abscess on radiological assesment5,7). Therefore, differential diagnosis of this condition may be difficult.
Here, we report a case of posterior epidural herniation of a lumbar disk fragment at L2–3. The lesion showed unusual radiographic findings and the patient had a past history, so it mimicked an epidural hematoma.
CASE REPORT
The patient was a 57-year-old man who presented with lower back pain and weakness on right hip flexion and right knee flexion. He had lower back pain 1 day previously, and received a transforaminal epidural block at L2–3 at a local hospital. He had taken 100-mg aspirin and antihypertensive drugs for 3 years due to a previous infarction and essential hypertension. The next day, he reported weakness of the right lower extremity. After walking 10 steps, he sat down due to weakness of the right lower extremity.
In our hospital, a neurologic examination was performed. The motor power in right hip flexion and right knee flexion was 4/5. Sensation in the lower extremity was intact. Other neurologic examination was not shown abnormalities. Magnetic resonance imaging (MRI) of the lumbar spine revealed a dorsal epidural lesion with compression of the thecal sac at L2–3. The lesion had relative hypointensity on T2-weighted imaging and isointensity on T1-weighted imaging (Fig. 1). We did not perform enhancement MRI. In blood test, erythrocyte sedimentation rate was 3.0 mm/hr and a C-reactive protein level was 0.29 mg/L. The result showed that the chances of infection were highly unlikely. Prothrombin time and activated partial thromboplastin time were not prolonged (9.9 seconds; 26.1 secodns). Bleeding time was not assessed. The initial differential diagnoses included epidural hematoma after the block, tumor, and a sequestrated disk. Operation was performed. We used laminectomy at L2 via posterior approach. After removal of the ligamentum flavum, a large, solid posterior epidural herniation of disk fragment was identified. The fragment compressed thecal sac, anteriorly (Fig. 2). Granulation tissue was identified around the disk fragment. After removal of the fragment, we identified an annular defect of the disk space. The specimen was determined to be fresh, degenerated fibrocartilage on histopathologic analysis. The postoperative course was uneventful. After 2 weeks of physiotherapy, the patient’s right lower extremity weakness resolved.
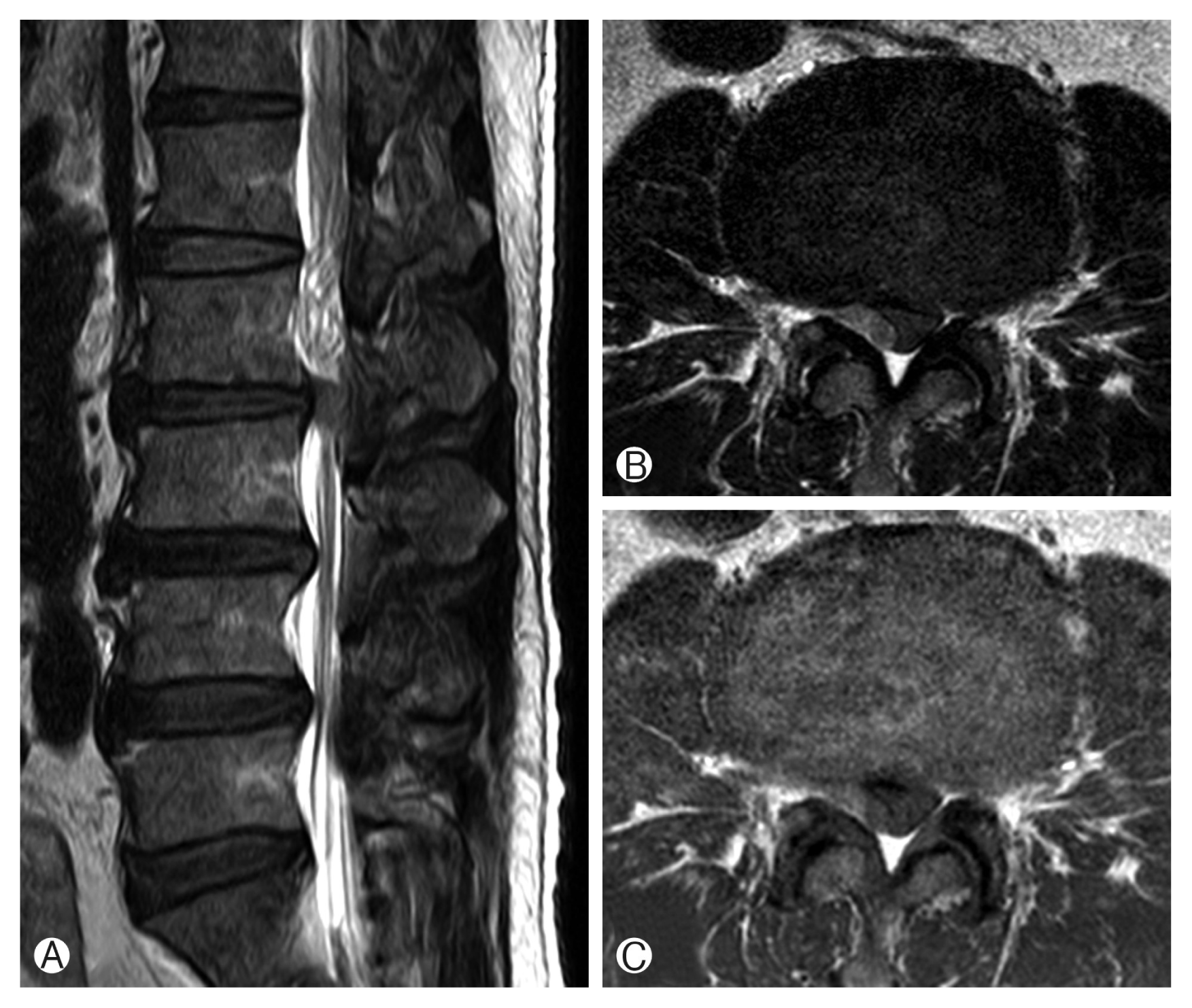
(A) A sagittal T2-weighted magnetic resonance imaging (MRI) of the lumbar spine shows a hypointense epidural mass at the L2–3 level. (B) An axial T2-weighted MRI shows a hypointense epidural mass, compressing the thecal sac. (C) An axial T1-weighted MRI shows an isointense epidural mass, compressing the thecal sac.
DISCUSSION
Posterior epidural herniation of lumbar disk fragments is rare. The disk fragment migrations are commonly limited by the attachments of the PLL and its associated midline septum and peridural or lateral membrane, and the nerve root itself1,2). The disk fragments are usually relocated in the anterior epidural space; they are infrequently found lateral to the thecal sac. Cephalad migration is more common with lateral disk herniation, whereas caudal displacement may be more common in central disk herniation3). The pathogenic mechanism of posterior epidural herniation of lumbar disk fragment was not understood. Maybe, a problem with anatomical barriers, such as PLL, causes posterior epidural herniation of lumbar disk fragment.
The symptoms of posterior epidural herniation of lumbar disk fragment are variable and include lumbago and cauda equina syndrome4). Our patient presented with lower back pain and weakness on right hip flexion and right knee flexion. There were no sensory changes, bladder dysfunction, or bowel problems.
The differential diagnosis of posterior epidural herniation of lumbar disk fragments may be difficult. MRI was the method of choice for radiological diagnosis of lumbar degenerative diseases. However, it was hard to differentiate completely similar lesions such as herniated disk, epidural hematoma, tumor or abscess10).
Herniated disks are usually hypointense on T1-weighted images and hyperintense on 80% of T2-weighted images1,2). The high signal intensity on T2-weighted images is because the herniated substance still has a higher water content compared to an unbroken disk, or may be due to a reparative course leading to a temporary water increase6). In our patient, the lesion was located in the posterior epidural space. The lesion had relative hypointensity on T2-weighted imaging and isointensity on T1-weighted imaging.
The differential diagnosis between posterior epidural herniation of lumbar disk fragment and epidural hematoma is very difficult. Disc herniation with migration may have contact with the disk space from which the fragment arised, whereas hematomas have lesser contact with a disk space9). In our patient, the lesion did not show continuity with a disk space on MRI. Intraoperatively, we identified an annular defect of the disk space. Epidural hematomas are associated with a history of trauma. Our patient had taken antiplatelet drugs. He received a transforaminal epidural block at L2–3 before symptom onset. In a variety of these situations, the lesion mimics an epidural hematoma.
Early surgery is the first choice for treatment. Generally, the surgical outcome of posterior epidural herniation of a lumbar disk fragment is better than conventional disk herniation1,2). Our patient’s surgical outcome was also good.
CONCLUSION
Posterior epidural herniation of lumbar disk fragment is rare and difficult to diagnose, as it may mimic other, more common posterior epidural lesions. Posterior epidural herniation of lumbar disk fragment should be considered in the differential diagnosis of dorsal epidural lesions. Surgical treatment should be considered for the best outcome.
Notes
CONFLICT OF INTEREST
No potential conflict of interest relevant to this article was reported.
