Diversity in Surgical Decision Strategies for Adult Spine Deformity Treatment: The Effects of Neurosurgery or Orthopedic Training Background and Surgical Experience
Article information
Abstract
Objective
This study is aimed to investigate whether surgical strategies for adult spinal deformity (ASD) treatment differed among Korean physicians.
Methods
This study is retrospective questionnaire-based study. ASD is challenging to manage, with a broad range of clinical and radiological presentations. To investigate possible nationality- or ethnicity-related differences in the surgical strategies adopted for ASD treatment, the International Spine Study Group surveyed physicians’ responses to 16 cases of ASD. We reviewed the answers to this survey from Korean physicians. Korean orthopedic surgeons (OS) and neurosurgeons (NS) received a questionnaire containing 16 cases and response forms via email. After reviewing the cases, physicians were asked to indicate whether they would treat each case with decompression or fusion. If fusion was chosen, physicians were also asked to indicate whether they would perform 3-column osteotomy. Retrospective chi-square analyses were performed to investigate whether the answers to each question differed according to training specialty or amount of surgical experience.
Results
Twenty-nine physicians responded to our survey, of whom 12 were OS and 17 were NS. In addition, 18 (62.1%) had more than 10 years of experience in ASD correction and were assigned to the M10 group, while 11 (37.9%) had less than 10 years of experience and were assigned to the L10 group. We found that for all cases, the surgical strategies favored did not significantly differ between OS and NS or between the M10 and L10 groups. However, for both fusion surgery and 3-column osteotomy, opinions were divided regarding the necessity of the procedures in 4 of the 16 cases.
Conclusion
The surgical strategies favored by physicians were similar for most cases regardless of their training specialty or experience. This suggests that these factors do not affect the surgical strategies selected for ASD treatment, with patient clinical and radiological characteristics having greater importance.
INTRODUCTION
The treatment of adult spinal deformity (ASD) is one of the most significant medical issues in countries with an aging society, with 60% of patients with ASD being elderly [1,2]. When considering treatment options, physicians must take into account various perspectives, basing their decisions on not only the presentation of ASD upon radiological imaging, but also on patient symptoms and quality of life [3]. In other words, careful consideration should be given to the age, symptoms, and prognosis of patients before proceeding with surgical treatment for ASD [3,4]. It is especially pertinent as the management of ASD can require complex procedures such as multilevel arthrodesis and occasionally also 3-column osteotomy [5]. Therefore, selecting the most appropriate surgical treatment strategy is important for enabling patients to maintain a good prognosis and experience fewer complications.
As in other countries, both orthopedic surgeons (OS) and neurosurgeons (NS) perform spinal surgeries in Korea. Although spine surgeon specialty has not been found to be significantly associated with the risk of 30-day complications in patients with single-level fusion [6], hospital stay length and perioperative transfusion rates significantly differ between patients treated by OS and those treated by NS [7]. However, few studies have reported on differences in the surgical strategies adopted by surgeons practicing in these fields. While OS tend to believe that the vertebra itself is the main factor to be considered in spinal surgery, NS tend to consider nerve decompression to be most important. Therefore, whether strategies for the surgical treatment of ASD differ between OS and NS needs confirmation.
The treatment of ASD may also differ according to doctors’ experience. In a questionnaire-based study of the spine surgeon selection criteria used by patients, Manning et al. [8] found that patients prefer physicians younger than 65 years of age. The importance of physician experience in influencing surgical procedure decisions should therefore not be overlooked or underestimated, with the effect of career length on approaches to surgery for ASD also requiring confirmation.
We therefore aimed to clarify whether there are differences in the surgical strategy adopted for ASD among spinal surgeons in Korea. To this end, the 2016 International Spine Study Group (ISSG) questionnaire, which investigated nationality- and ethnicity-related differences in physicians’ opinions regarding appropriate surgical strategies, was used to survey our participants.
MATERIALS AND METHODS
1. Participants
In this study, we reviewed answers from Korean physicians to the ISSG questionnaire. A total of 41 physicians were targeted in the online survey conducted by ISSG in Korea from December 2016 to January 2017. The physicians were selected from members of the Korean Society of Spine who were experienced in ASD surgery.
2. Questionnaire
The questionnaire given to physicians consisted of instruction and case sheets. In the instruction sheets, physicians were asked to answer the enclosed questions intuitively rather than after thinking deeply. They were then told that they were required to answer questions based on the case information provided. First, physicians were asked if they would proceed with decompression only (i.e., nonfusion treatment) or fusion. If they chose fusion, they were required to select the upper-most instrumented vertebra (i.e., the starting point for fusion) and the lower-most instrumented vertebra. They were also asked to indicate whether they would proceed with 3-column osteotomy and the corresponding level at which it would be performed. Three-column osteotomy procedures included pedicle subtraction osteotomy (PSO), bone-disc-bone osteotomy (BDBO), and vertebral column resection (VCR). Smith-Petersen osteotomy was not included.
Case sheets contained 2 or more thoracolumbar plain radiographs of patients with ASD (Figs. 1-4). The following information was also included with each case: whole-spine standing radiographs with measurement values; Scoliosis Research Society (SRS)-Schwab ASD classification and sagittal modifiers; presence or absence of spinal stenosis, its location, and clinical information including chief complaints; health-related quality of life scores; and visual analogue scale for pain results. A total of 16 cases were included, and their characteristics are described in the following subsection.
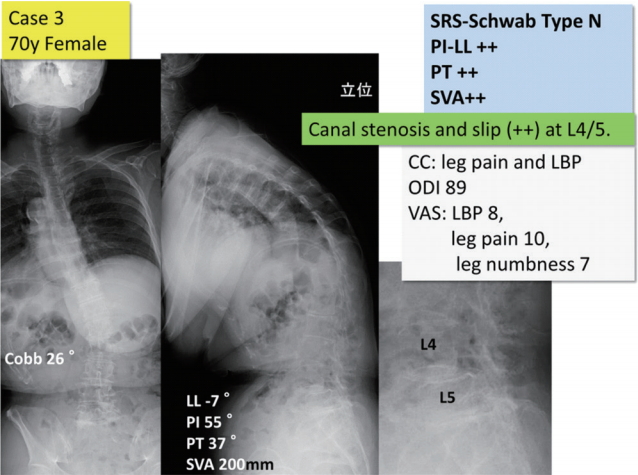
Patient characteristics and whole spine X-ray of case 3. SRS, Scoliosis Research Society; PI, pelvic incidence; LL, lumbar lordosis; PT, pelvic tilt; SVA, sagittal vertical axis; CC, chief complaints; LBP, low back pain; ODI, Oswestry disability index; VAS, visual analogue scale.
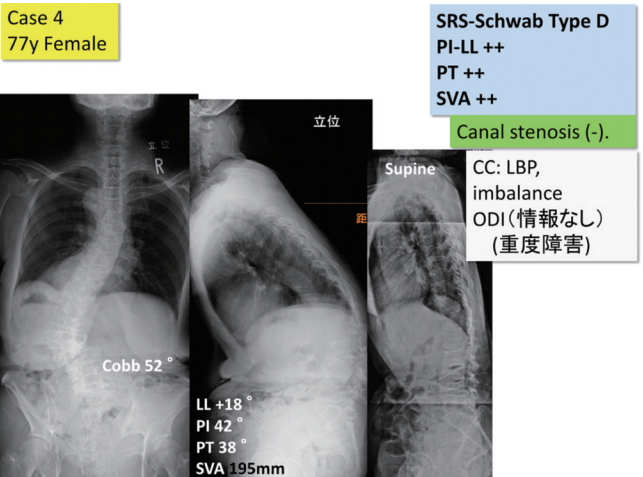
Patient characteristics and whole spine X-ray of case 4. SRS, Scoliosis Research Society; PI, pelvic incidence; LL, lumbar lordosis; PT, pelvic tilt; SVA, sagittal vertical axis; CC, chief complaints; LBP, low back pain; ODI, Oswestry disability index.
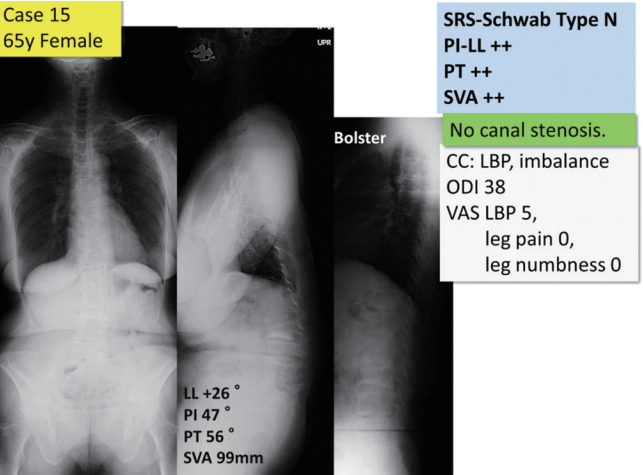
Patient characteristics and whole spine X-ray of case 15. SRS, Scoliosis Research Society; PI, pelvic incidence; LL, lumbar lordosis; PT, pelvic tilt; SVA, sagittal vertical axis; CC, chief complaints; LBP, low back pain; ODI, Oswestry disability index.
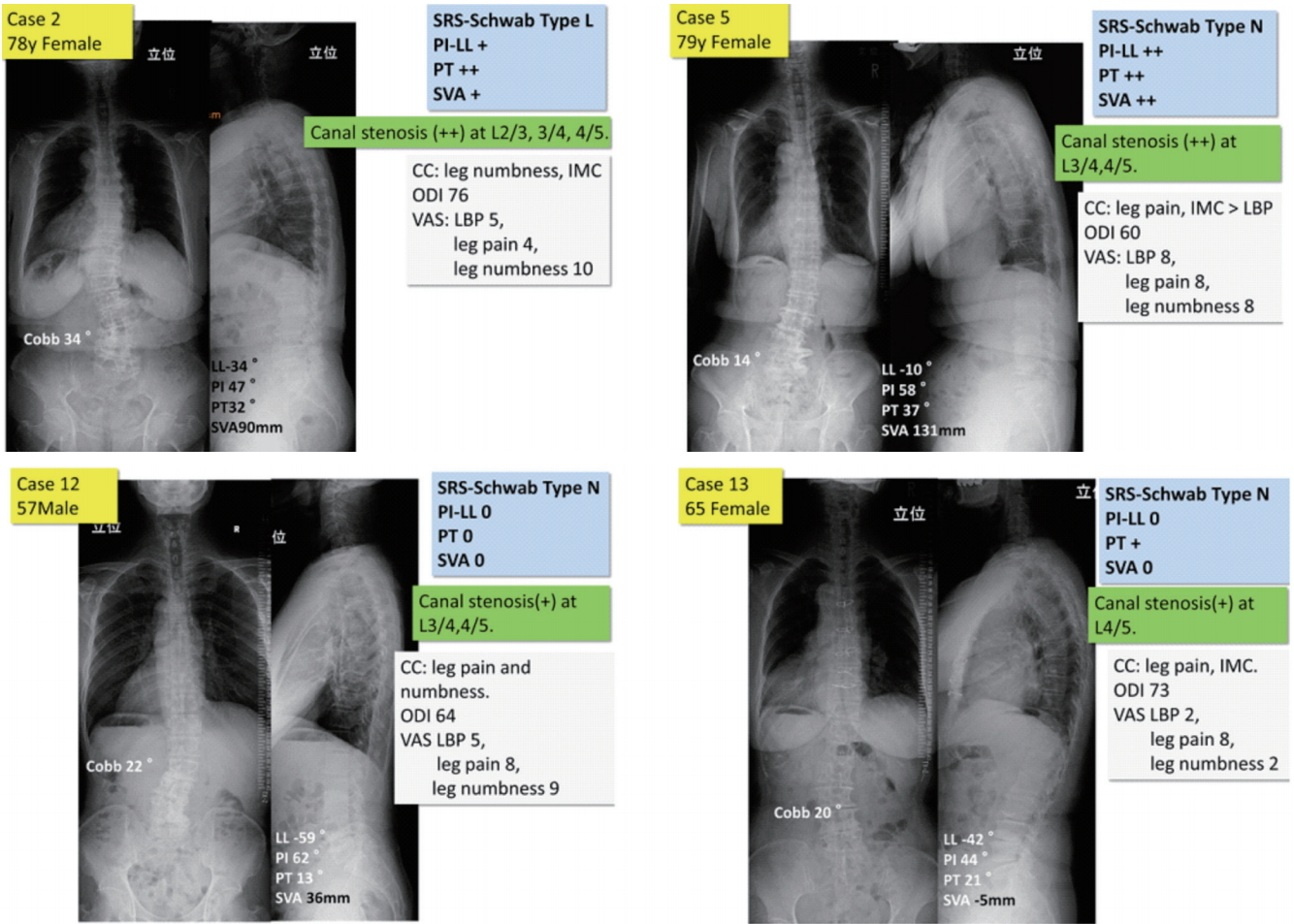
Patient characteristics and whole spine X-ray of 4 cases with high discordance in surgical strategies (2, 5, 12, and 13). SRS, Scoliosis Research Society; PI, pelvic incidence; LL, lumbar lordosis; PT, pelvic tilt; SVA, sagittal vertical axis; CC, chief complaints; LBP, low back pain; ODI, Oswestry disability index.
3. Case sheet patient characteristics
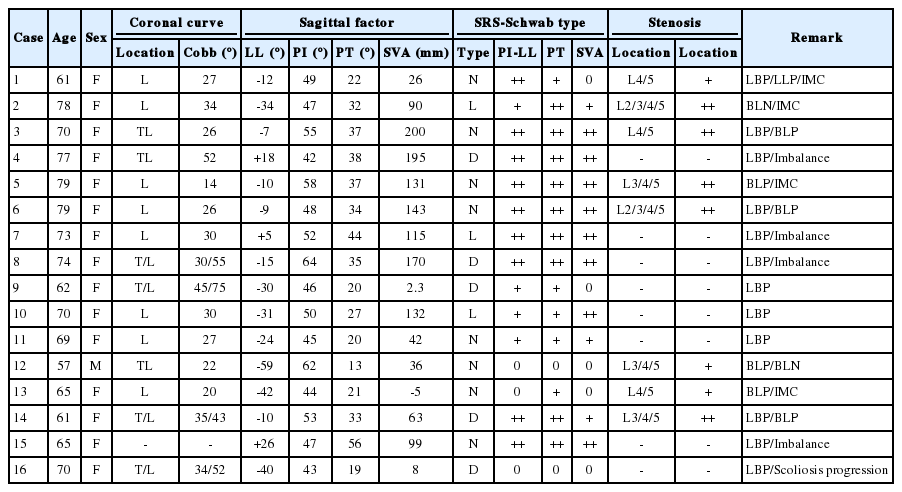
The characteristics of patients described in the case sheets are summarized in Table 1. As mentioned previously, there were 16 cases whose sex and age were included. Imaging features that were provided included the position and Cobb angle of major curves on coronal radiographs. Sagittal parameters included lumbar lordosis (LL), pelvic incidence (PI), pelvic tilt (PT), and sagittal vertical axis (SVA).
SRS-Schwab curve type and the location and severity of stenosis were also summarized. Specifically, major coronal curves were classified as 1 of the following 4 types according to the SRS-Schwab ASD classification system: T, thoracic curve only; L, thoracolumbar or lumbar curve only; D, double curve with both thoracic and thoracolumbar/lumbar curves; and N, no major coronal deformity with all coronal curves having Cobb angles <30°. Sagittal modifiers of SRS-Schwab type (PI minus LL, PT, and SVA) were also shown and each assigned a score of “0,” “+,” or “++” to indicate severity. For PI minus LL, a score of “0” was assigned to values <10°, “+” to moderate values of 10°–20°, and “++” to values >20°. For SVA, which indicates global alignment, “0” was assigned to SVA values <4 cm, “+” to values from 4–9.5 cm, and “++” to values >9.5 cm. Finally, for pelvic tilt, “0” was assigned to values <20°, “+” to moderate values of 20°–30°, and “++” to values > 30° [9].
4. Statistical analysis
Prior to statistical analysis, answers were classified into those from OS (i.e., the OS group) and those from NS (i.e., the NS group). They were also divided into those from physicians with less than 10 years of surgical experience (i.e., the L10 group) and those from physicians with more than 10 years of surgical experience (i.e., the M10 group). The chi-square test and Fisher exact test were then performed to analyze between-group differences in the surgical strategies chosen for ASD treatment. We also conducted multirater agreement analysis with the kappa statistic to assess agreement between groups. The significance level was set at p<0.05. Statistical analyses were conducted using the IBM SPSS Statistics ver. 21.0 (IBM Co., Armonk, NY, USA).
RESULTS
1. Respondent demographics
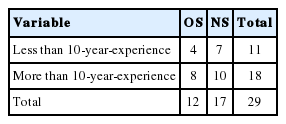
A total of 29 physicians responded to the questionnaire via email. Of these 29 physicians, 12 (41.4%) were OS and 17 (58.6%) were NS. All were specialized in ASD correction surgery at different university hospitals in Korea. Furthermore, 18 (62.1%) had more than 10 years of experience in ASD correction and were assigned to the M10 group. The remaining 11 (37.9%) were assigned to the L10 group. Respondent demographics are summarized in Table 2.
2. Between-group comparisons of questionnaire responses
Questionnaire responses to the question regarding fusion are summarized in Table 3. The distribution of fusion and nonfusion decisions did not significantly differ between specialties (i.e., between the OS and NS groups), nor between levels of experience (i.e., between the M10 and L10 groups). Of note, opinions for cases 2 and 5 tended to be evenly divided in both the OS and NS groups, with 50% of OS and 52.9% of NS agreeing with the fusion strategy. Opinions were also evenly divided for cases 12 and 13, with 55.56% of M10 group and 54.5% of L10 group respondents agreeing with fusion.
With regard to 3-column osteotomy, the strategy chosen did not significantly differ between the NS and OS groups, nor between the M10 and L10 groups (Table 4). As with the question regarding fusion, opinions were roughly evenly divided for some cases (namely, cases 3, 4, and 15) in both the OS and NS groups. The proportions of respondents in favor of 3-column osteotomy for these cases were as follows: case 3, 41.7% of OSs; case 4, 50% of OS and 52.9% of NS; and case 15, 41.7% of OS and 41.2% of NS.
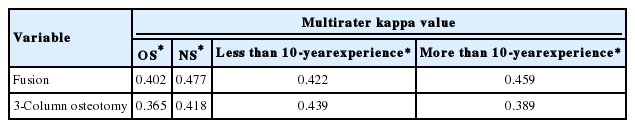
Finally, we also conducted multirater agreement analysis with the kappa statistic to assess agreement between groups. Kappa values were higher than 0.4 for all questions apart from OS and M10 groups answers to the question regarding 3-column osteotomy (Table 5).
3. Case Illustrations
Fig. 1 shows case 3 of survey cases. A 70-year-old female patient with SRS-Schwab type N, who is suffering from legs and back pain, was given. Scoliosis and thoracic kyphosis were observed on X-ray. In addition, spondylolisthesis findings of L4 and L5 are observed. All respondents answered that the patient needed fusion surgery, which was independent of specialty and careers (Table 3). However, there was a lot of debate about whether 3-column osteotomy was performed (Table 4).
In case 4, a 77-year-old female with low back pain may have camptocormia on X-ray. Her SRS-Schwab type was D with high PI-LL. There was no information of ODI, but she has mid-grade disability on activities on daily living (Fig. 2). Twenty-five percentage of OS (3 of 12) did not choose to perform fusion surgery, but in NS only one surgeon did not choose fusion surgery (0.06%, 1 of 17). However, there was no significant difference in OS and NS groups.
DISCUSSION
Increases in life expectancy have increased the prevalence of ASD, and the number of surgeries performed to treat this disease is growing accordingly. In 2009, Li et al. [10] showed that patients over the age of 65 who underwent surgery for adult scoliosis experienced significantly less pain and had better healthrelated quality of life, higher self-image, and better mental health than those who underwent conservative treatment. Smith et al. [11,12] also showed in 2 separate studies that patients who underwent surgical treatment for ASD had reduced back and leg pain, as compared to those who did not undergo surgery to correct adult scoliosis. Taken together, these studies show that surgical treatment is more effective than conservative treatment. To maximize the possibility of achieving good postoperative outcomes, surgical strategies for ASD treatment should be carefully determined with consideration from various perspectives.
Although surgical strategies may differ between each hospital, differences in the training of OS and NS, as well as physicians’ length of surgical experience, are generally thought to be more important in determining surgical strategy selection. As in many other countries, both OS and NS perform spine surgeries for ASD in Korea. The training length for both specialties is similar; after graduating from medical school, most graduates complete a 1-year internship at a qualified hospital. They then choose a specialty and complete a 4-year residency course for that specialty. Therefore, the medical training pathway in Korea can reduce the confounding effect of training length, allowing the effect of training specialty (in our case, OS vs. NS) and experience length to be analyzed more accurately.
We found no significant differences in the surgical strategy adopted (i.e., nonfusion vs. fusion) between OS and NS, nor between the M10 and L10 groups. This suggests that there was no difference in surgical treatment planning for fusion regardless of specialty and career length. However, it is necessary to more closely examine responses to cases 2, 5, 12, and 13 (Fig. 4). For both cases 2 and 5, opinions were evenly divided, with 50% of OS and 52.9% of NS deciding to proceed with fusion surgery. This discordance may be accounted for by the perspective taken by physicians when determining the most appropriate course of action. For example, some physicians may consider stenosis symptoms to be the main therapeutic target, while others may consider the correction of deformity in terms of coronal curve severity, sagittal factors, and SRS-Schwab classification to be more important. Therefore, surgeons may have answered the question differently depending on where their treatment was focused. Opinions were similarly discordant among both OS and NS for cases 12 and 13. Stenosis symptoms were predominant in these 2 cases, with mild scoliosis curves in the lumbar area.
As with responses to the question regarding fusion, there were no significant differences in whether surgeons would proceed with 3-column osteotomy between OS and NS, nor between the M10 and L10 groups. However, opinions on the appropriateness of 3-column osteotomy were more variable than those on the appropriateness of fusion. Opinions were particularly discordant among both OS and NS for cases 3, 4, and 15 (Figs. 1-3). Interestingly, for case 3, relatively young or less experienced surgeons tended not to opt for 3-column osteotomy, while opinions varied among more experienced physicians. It should be noted that the patient in this case had the largest SVA value and showed thoracolumbar kyphosis. It is interesting that most physicians in the L10 group thought that such deformity could be corrected by conventional fixation. If flexion and extension radiographs were also provided, it is likely that the distribution of answers would have been different.
However, it is important for physicians to apply careful consideration before proceeding with 3-column osteotomy for ASD as the procedure has both advantages and disadvantages. Although the 3-column osteotomy techniques of PSO, BDBO, and VCR are all dramatically effective in the correction of coronal or sagittal curves, PSO and VCR result in increased blood loss and lower fusion rates in older populations. These procedures are also associated with major complications such as inadvertent extubation, malignant hyperthermia, severe hypotension, cerebrovascular accident, myocardial infarction, nerve root injury, vascular/visceral injury, instrumentation or junctional failure, and major neurological deficits [13]. Other studies have also shown that there has been a significant increase in complications after 3-column osteotomy [14-20]. Therefore, the necessity of 3-column osteotomy needs to be deliberately and cautiously determined, with the discordance among our surveyed doctors reflecting this prudence.
We also conducted multi-rater agreement analysis with the kappa statistic to assess agreement between groups. Multirater kappa values ranged from 0.365 to 0.477, indicating that answers were relatively reliable. Furthermore, the questions that were skipped for each of the 16 cases did not significantly differ between OS and NS. This demonstrates that strategies for ASD treatment do not differ between these specialties, which have important implications for treatment. Patients want standardized treatment as well as patient-tailored treatment. Our results suggest that this can be achieved as cases will be approached with the same surgical strategy regardless of whether they are being handled by OS or NS. Our results also suggest scope for interdisciplinary collaboration, with spine surgeons being able to offer a greater range of treatment options to patients regardless of their specialty, as well as being able to exchange professional opinions with surgeons in other fields to reach a more informed consensus. For NS in Korea, the spine field is still very popular. Thus, although orthopedic surgery has a long history of spine correction and fixation, patients’ preferences are not clearly divided. In a study by Clark et al. [21] in 2014, members of the American Association of Neurological Surgeons were surveyed about ASD surgery. Neurosurgeons’ experience, research, and academic activities have enhanced their ASD-related knowledge and decision-making. In Korea, the duration of the spine fellowship itself is not different between NS and OS. Likewise, there is little difference in program between the 2 groups at present. However, nowadays neurosurgeons’ research on ASD and their activities are more increasing and active than other fields, which demonstrate the results of our research and Clark’s study.
Similarly, there were no significant differences in the strategy adopted according to the length of clinical experience. This indicates that interaction between surgeons with differing levels of experience is desirable, as increased reliability in the treatment of patients regardless of physician experience enables the increased need for spinal surgery in Korea to be met. Taken together, these results suggest that other factors, such as differences in the clinical and radiological characteristics of patients, are more important in determining surgical strategy than physicians’ training background or surgical experience.
Despite the insights provided by our study, it does have some limitations. Firstly, the case information provided in this questionnaire was limited. Plain radiographs revealing sagittal and coronal deformities, as well as brief descriptions of patients’ stenosis and symptoms were provided. However, magnetic resonance imaging, computed tomography, and X-ray dynamogram data, as well as information on patient lifestyles and comorbidities were omitted, which may have increased the difficulty of the questionnaire. Secondly, the small number of respondents could also be viewed as a limitation. Lastly, physicians were instructed to answer the questionnaire intuitively without discussion with their colleagues. Therefore, individual confusion and unfamiliarity with the cases could have also limited our study by affecting the answers given.
We have also collected responses of UIV and LIV. However, the response rate was very low and we could not find commonality between respondents. Therefore, statistical analysis was impossible and the results were not presented in this study.
Likewise, respondents were divided into 10 years of experience. However, the number of detailed annual deformity operations was not known. The questionnaires were members of the Korean Society of Spine Deformity. Most of them are judged to be professional, but this study has the disadvantage of not showing their objective experience.
CONCLUSION
We investigated whether surgical strategies for the treatment of ASD differ among Korean physicians according to training specialty and length of experience. We found that the surgical strategies favored did not significantly differ between OS and NS, and between surgeons with different levels of experience. This study suggests that physicians’ experience and training specialty do not affect decision-making regarding surgical strategies for ASD, with patient clinical and radiological characteristics having greater importance.
Notes
The authors have nothing to disclose.