The Transspinal Canal Screwing Technique for Atlantoaxial Anomalies: A Technical Note and 2 Case Reports
Article information
Abstract
It is difficult to treat atlantoaxial instability in patients with a high-riding vertebral artery or anomalies of the craniocervical junction. We report 2 successful cases in which the transspinal canal screwing technique was used because of difficulties performing conventional fixation methods. Case 1: A 78-year-old woman suffered from progressive myelopathy due to severe spinal cord compression with a congenital anomaly of the craniovertebral junction. Bilateral transspinal canal screws from the axis body with spondylolisthesis to the dens were inserted by retracting the dural sac medially after foramen magnum decompression and cervical laminoplasty. Case 2: A 20-year-old man with a spinal deformity due to Loeys-Dietz syndrome presented to our hospital for treatment of syringomyelia. He had no obvious neurological deficits, but spinal cord compression due to right atlantoaxial rotating dislocation was observed. A screw was inserted from the vertebral body of the axis to the right lateral mass of the atlas via the spinal canal after laminectomy of the atlas. The transspinal canal screwing technique is useful for treating atlantoaxial instability in cases where other fixation methods are difficult.
INTRODUCTION
Surgical treatments for atlantoaxial dislocation such as Magerl and Goel-Harms technique are representative methods that can obtain firm fixation. But in cases with high riding vertebral artery (VA) or anomalies of craniovertebral junction, it is difficult to preserve trajectory of screw. We present technical note and 2 case reports with screw fixation via spinal canal because conventional methods are impossible.
CASE REPORTS
1. Case 1
A 78-year-old female presented with a 3-month history of progressive dysthesia of her upper and lower limbs and gait disturbance. Her gait was spastic and unstable and her deep tendon reflex of lower limbs was increased. Computed tomography (CT) showed atlas fusion to occipital bone and axis, and spondylolisthesis of axis body with fusion failure (Fig. 1B). Functional plain radiograph showed slight instability of axis bodies with spondylolisthesis (Fig. 1A). Magnetic resonance imaging (MRI) showed severe spinal cord compression at the level of craniovertebral junction (Fig. 1C).
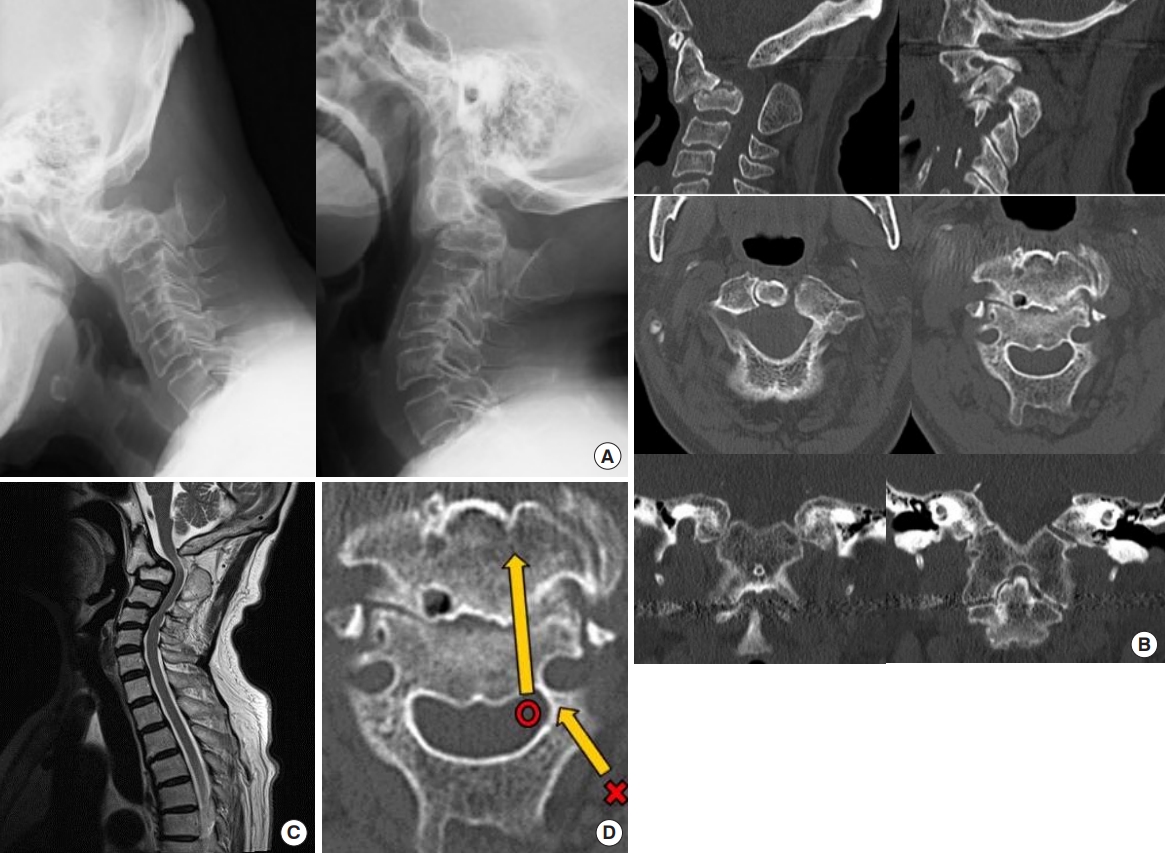
Preoperative images: (A) functional plain radiograph, (B) computed tomography, (C) magnetic resonance imaging, and (D) schema of screw trajectory in computed tomography.
To treat this pathology, decompression of spinal cord and fixation of unstable axis bodies with spondylolisthesis were necessary. However, selection of fixation method was difficult because conventional methods for atlantoaxial instability were all impossible for her congenital anomaly. Occipital-cervical fixation was also considered, but hesitated because the risk of postoperative dysphagia was high for her age. We decided to perform transspinal canal screw fixation by designing the trajectory with modifying Magerl method because left VA was high riding (Fig. 1D).
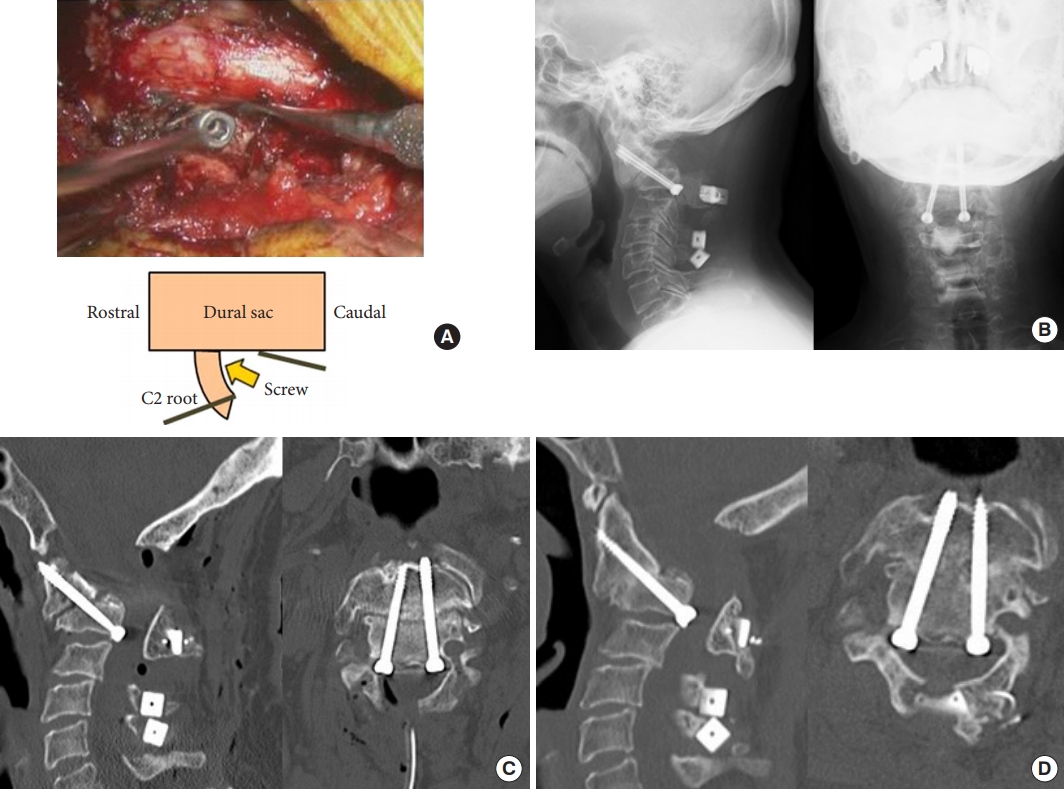
Reduction of listhesis by position under general anesthesia was tried as much as possible but the degree was small. Decompression of spinal cord by resection of occipital bone and cervical laminoplasty was performed. Then, bilateral transcanal screws from caudal axis body to dens were inserted by retracting dural sac medially with lateral fluoroscopy (Fig. 2A-C). Her symptoms were gradually improved and she went back home. Six months after operation, bony fusion was confirmed (Fig. 2D).
2. Case 2
A 20-year-old man with spinal deformity for Leys-Dietz syndrome visited our hospital to treat syringomyelia that was pointed out incidentally. There was no obvious neurological deficit but CT showed right atlantoaxial rotating dislocation (Fig. 3B, C). Functional plain radiograph showed that instability was unclear (Fig. 3A). MRI showed spinal cord compression at the level of atlas and syringomyelia (Fig. 3D).
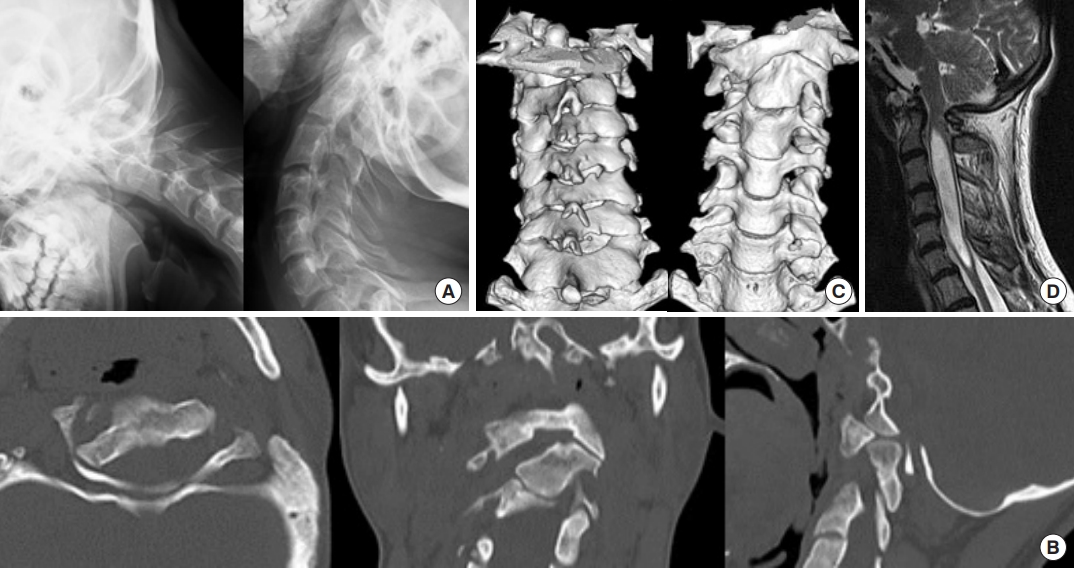
Preoperative images: (A) functional plain radiograph, (B) computed tomography, (C) 3-dimentional computed tomography, and (D) magnetic resonance imaging.
Reduction of rotating dislocation was expected to be difficult for chronic change. Atlantoaxial fixation was planned to be care for risk of luxation due to laminectomy of atlas. However, conventional methods for atlantoaxial instability were all impossible to preserve screw trajectory. So we decided to perform transcanal screw fixation.
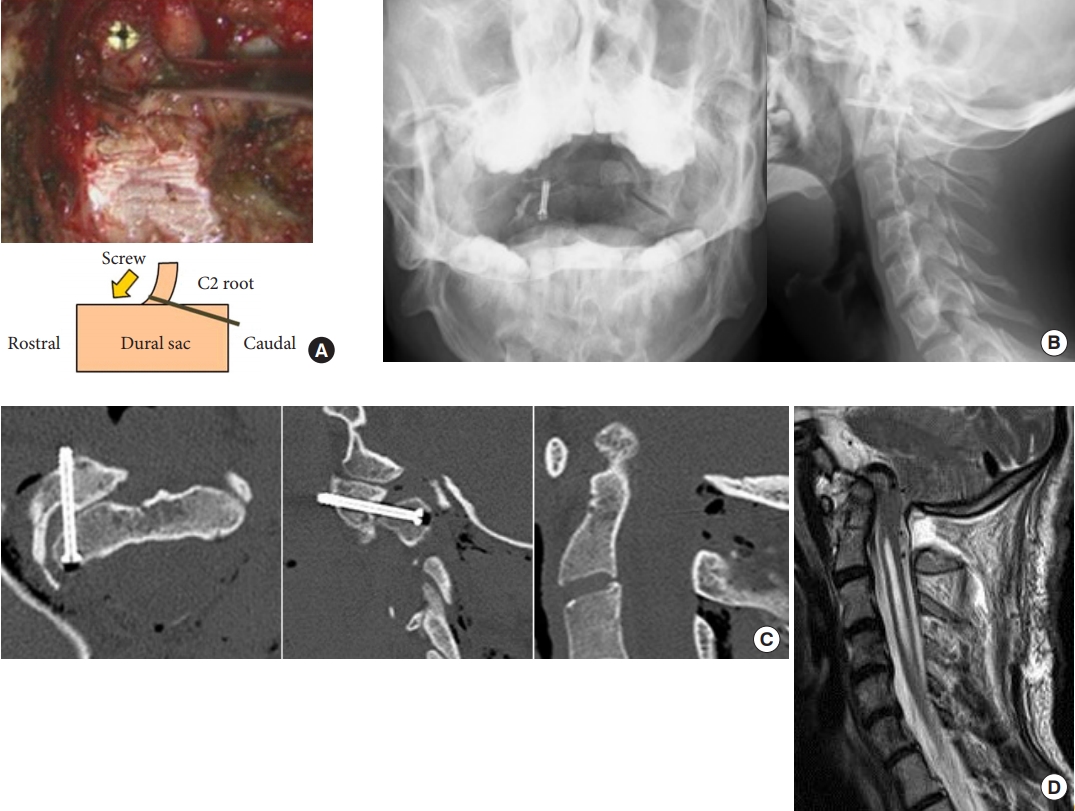
After general anesthesia, reduction of rotation was tried but impossible. Screw was inserted from the vertebral body of axis to right lateral mass of atlas via spinal canal by retracting right C2 nerve root caudally after laminectomy of atlas (Fig. 4A-C). After operation, neurological deterioration was not found and syrinx tended to shrink (Fig. 4D).
DISCUSSION
The sclerotome occurs from the mesoderm-derived somite node. The vertebral body is formed by splitting and fusing adjacent sclerotomes [1-4]. The axis is formed from dens, caudal sclerotome of C2 and rostral sclerotome of C3. Os odontoideum, representive dysplasia of axis, occurs as a result of fusion failure between dens and C2 sclerotome [3,5-8]. Case 1 was considered to be fusion failure of axis body between C2 and C3 sclerotomes. About dysplasia of atlas, caudal component of C1 sclerotome fused to clivus and occipital bone, rostral component of C2 fused to axis body and lamina. Though obvious reduction was not able to make for slightness of instability, decompression and fusion was considered to be sufficient from improvement of her symptom. From the view point of bone grafting, occipital-cervical fixation was considered, but it was hesitated because the risk of postoperative dysphagia. By using this technique, it was possible to preserve mobility between occipital and axis. Bone grafting to the space of listhesis was impossible, but bony fusion was obtained.
Loeys-Dietz syndrome is a connective tissue disorder characterized by musculoskeltal, cardiovascular malformation due to TGFBR 1/2 gene abnormality [9]. It is reported high prevalence of instability, particularly C2–3 although case 2 was atlantoaxial rotating dislocation [10]. The cause of syrinx was considered to be disturbance of cerebrospinal fluid circulation at the level of craniovertabral junction. Therefore, it was considered that the shrinkage of syrinx was due to improvement of cerebrospinal fluid circulation by decompression procedure. Bony fusion may not be obtained because bone graft could not be applied to the space of luxation. Considering the stress of neck rotation, single screw fixation without bony fusion may not be sufficient for long-term stability, so careful follow-up is necessary.
The indication of transspinal canal screwing technique is in case with difficulty of preserve of screw trajectory for atolantoaxial instability with anomaly. The merit of this technique is that the procedure is possible with lateral fluoroscopy, so 3-dimensional CT navigation system is unnecessary because of the absence of VA injury risk even in high riding cases. The demerits are the risks of spinal cord injury and bleeding from epidural venous plexus due to retracting procedure. Moreover, it is difficult to preserve bony fusion bed because this technique requires laminectomy or laminoplasty. However, in case with difficulty by conventional methods anatomically, it is considered to be a useful option.
CONCLUSION
Transspinal canal screwing technique is useful to treat atlantoaxial instability when other fixation methods are difficult.
Notes
The authors have nothing to disclose.