 |
 |
- Search
| Neurospine > Volume 17(1); 2020 > Article |
|
|
Abstract
Objective
Methods
Fig.┬Ā1.
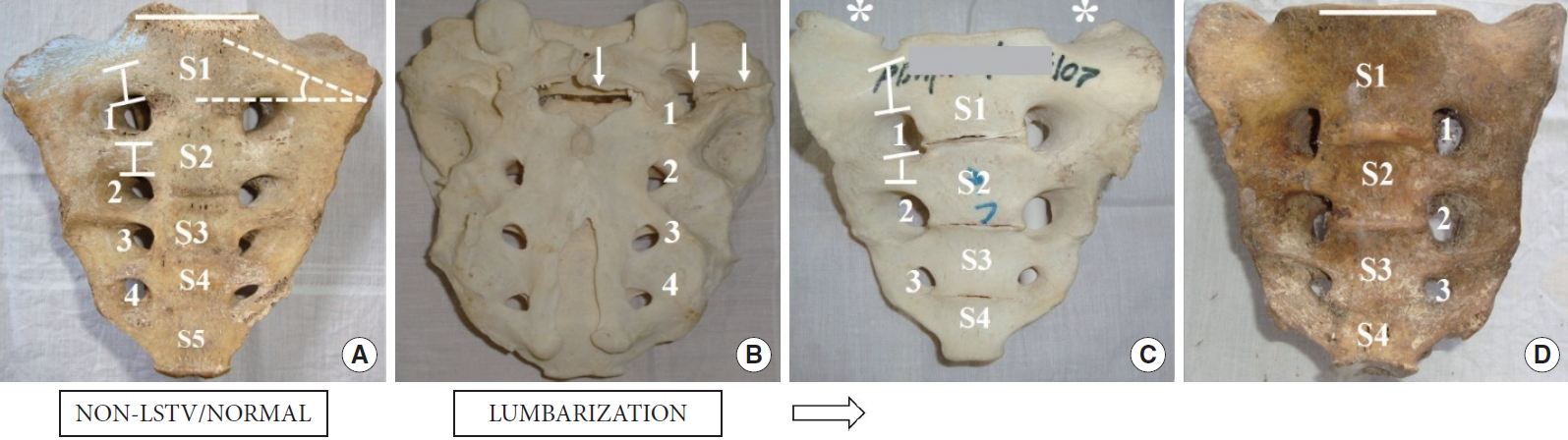
Fig.┬Ā2.

Fig.┬Ā3.
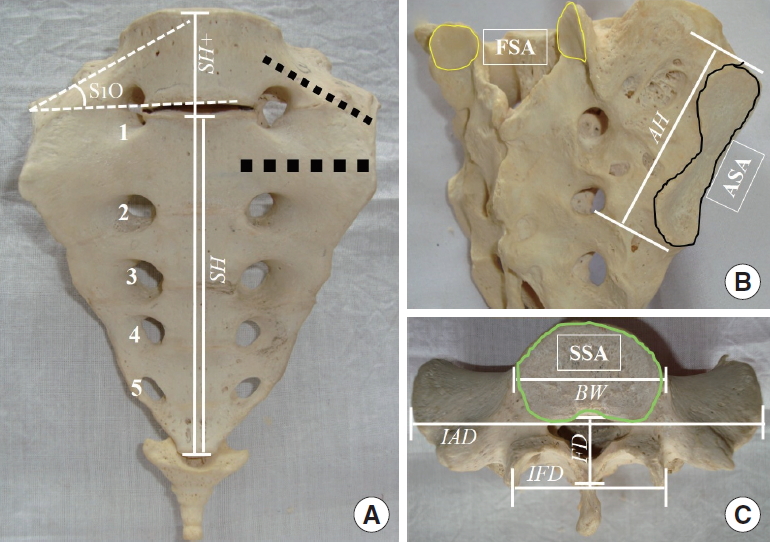
Fig.┬Ā4.
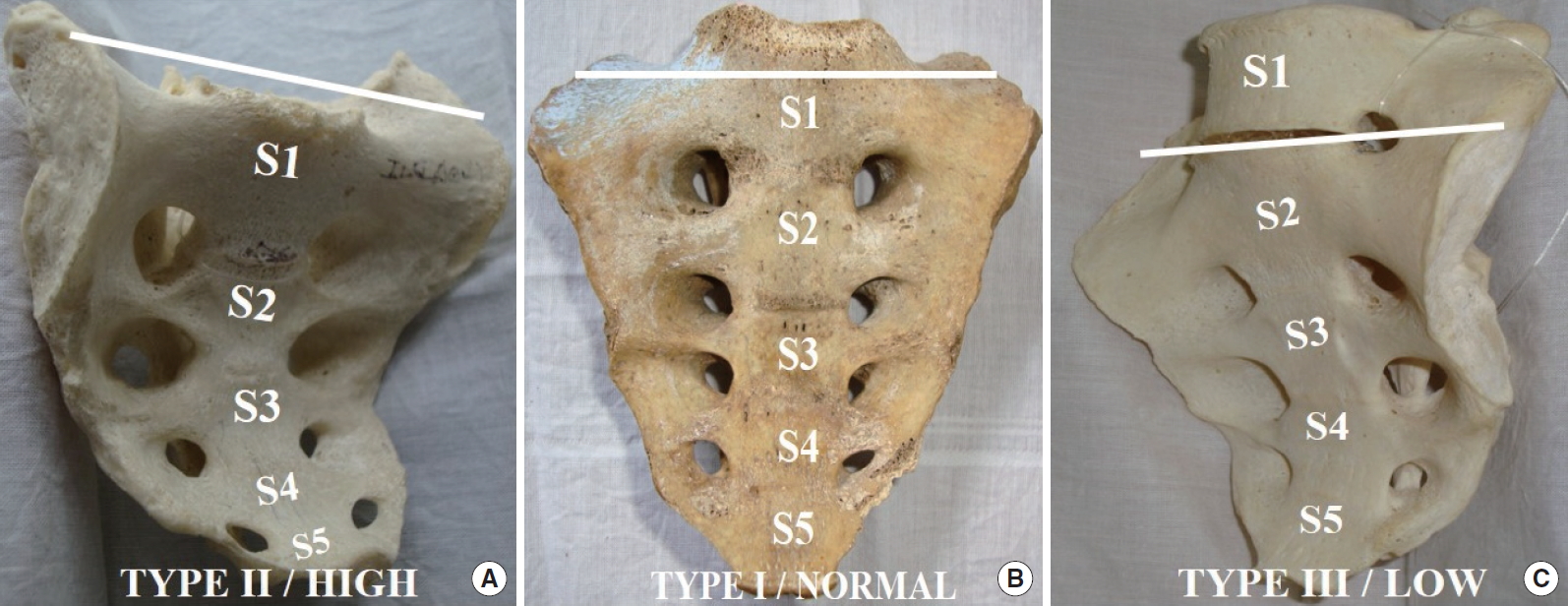
Fig.┬Ā5.

Table┬Ā1.
| LSTV typeŌĆĀ | Subtype | Anatomical criteria | Prevalence |
|---|---|---|---|
| Type I | Unilateral (Ia) | Transverse process(es)ŌĆĪ Ōēź 19 mm (craniocaudal dimension) | ~40% |
| Bilateral (Ib) | |||
| Type II | Unilateral (IIa) | Di-arthrodial joint: transverse process(es) with the sacral ala/e | - |
| Bilateral (IIb) | |||
| Type III | Unilateral (IIIa) | Complete osseous fusion: transverse process(es) to the sacral ala/e | ~11.5% |
| Bilateral (IIIb) | |||
| Type IV | - | Unilateral type II transition with a contralateral type III | ~5.25% |
The overall LSTV prevalence of ranges between 4.0% to 35.9% [10].
ŌĆĀ Castellvi classification does not distinguish lumbarization (separation of the upper sacral segment) and sacralization (addition of L5 as the upper sacral segment) of the lumbar spine while considering the lumbosacral junction. The biomechanical implications of the disparity in the number of sacral segments in these 2 conditions thus get overlooked in this classification.
ŌĆĪ Craniocaudal dimension of the transverse process at the lumbosacral junction. Castellvi classification does not specify if the transverse processes belong to an L5 vertebra (L5ŌĆōS1 accessory articulation), L4 vertebra (in sacralization), or L6 vertebra (in lumbarization) [12].
Table┬Ā2.
Table┬Ā3.
| Variable | Complete lumbarization (4 segments) | Incomplete lumbarization | Normal (5 segments) | Accessory articulation | Incomplete sacralization | Complete sacralization (6 segments) | |||
|---|---|---|---|---|---|---|---|---|---|
| Linear dimension (mm) | |||||||||
| ŌĆā | Sacral height | 90.78* ┬▒ 15.17 | - | 105.37 ┬▒ 15.32 | 105.05 ┬▒ 10.24 | 92.34 ┬▒ 9.39 | - | 102.14 ┬▒ 12.05 | 114.67 ┬▒ 12.4 |
| Auricular surface height | 59.55 ┬▒ 5.16 | 59.6ŌĆĀ ┬▒ 4.03 | 61.7ŌĆĪ ┬▒ 4.9 | 61.15 ┬▒ 8.16 | 59.53 ┬▒ 6.96 | 58.4ŌĆĀ ┬▒ 3.04 | 63.09ŌĆĪ ┬▒ 1.02 | 62.22 ┬▒ 4.3 | |
| Inter facet distance | 47.35 ┬▒ 5.66 | - | 47.73 ┬▒ 11.45 | 52.12 ┬▒ 4.34 | 47.12 ┬▒ 5.84 | - | 45.13 ┬▒ 3.94 | 46.55 ┬▒ 4.34 | |
| Inter auricular distance | 101.53 ┬▒ 9.02 | - | 94.02 ┬▒ 15.63 | 102.79 ┬▒ 10.09 | 100.22 ┬▒ 8.83 | - | 101.43 ┬▒ 6.21 | 98.24 ┬▒ 8.83 | |
| Alar width bilateral | 60.98 ┬▒ 4.9 | - | 48.28* ┬▒ 11.93 | 56.45 ┬▒ 3.47 | 58.73 ┬▒ 0.87 | - | 55.04 ┬▒ 1.76 | 51.39 ┬▒ 2.84 | |
| S1 body width | 40.55* ┬▒ 4.12 | - | 45.74 ┬▒ 3.7 | 46.34 ┬▒ 6.62 | 41.49 ┬▒ 7.96 | - | 46.39 ┬▒ 4.45 | 46.85 ┬▒ 5.99 | |
| Facet depth | 13.25 ┬▒ 5.46 | - | 14.14 ┬▒ 2.35 | 15.24 ┬▒ 2.9 | 12.33 ┬▒ 2.79 | - | 14.33 ┬▒ 3.35 | 16.58 ┬▒ 2.76 | |
| Surface area (cm2) | |||||||||
| Auricular surface area | 9.75 ┬▒ 1.24 | 8.03ŌĆĀ* ┬▒ 1.09 | 9.14ŌĆĪ ┬▒ 1.19 | 10.36 ┬▒ 1.86 | 10.56 ┬▒ 2.33 | 8.53ŌĆĀ ┬▒ 0.32 | 9.56ŌĆĪ ┬▒ 0.68 | 9.82 ┬▒ 1.24 | |
| Superior surface area | 8.35 ┬▒ 1.96 | - | 8.85 ┬▒ 1.23 | 10.02 ┬▒ 2.35 | 9.89 ┬▒ 3.32 | - | 9.46 ┬▒ 0.76 | 10.09 ┬▒ 3.32 | |
| Facet surface area | 1.31 ┬▒ 0.56 | 1.85ŌĆĀ ┬▒ 0.38 | 1.93ŌĆĪ ┬▒ 0.26 | 1.71 ┬▒ 0.51 | 1.29* ┬▒ 0.42 | 1.43ŌĆĀ ┬▒ 0.23 | 1.53ŌĆĪ ┬▒ 0.11 | 1.47 ┬▒ 0.46 | |
Values are presented as mean┬▒standard deviation.
Blank cells (-) denote variants that do not present a measurable anatomical feature on one side (incomplete fusions).
Table┬Ā4.
| Variable | Type II/high | Type I/normal | Type III/low |
|---|---|---|---|
| Linear dimension (mm) | |||
| ŌĆāSacral height | 94.82* ┬▒ 7.81 | 105.05 ┬▒ 10.24 | 108.4 ┬▒ 14.72 |
| ŌĆāAuricular surface height | 60.04 ┬▒ 6.36 | 61.15 ┬▒ 8.16 | 61.97 ┬▒ 5.01 |
| ŌĆāInter facet distance | 102.04 ┬▒ 6.3 | 102.79 ┬▒ 10.09 | 100.86 ┬▒ 10.25 |
| ŌĆāInter auricular distance | 42.9 ┬▒ 5.9 | 46.34 ┬▒ 6.62 | 46.97 ┬▒ 5.63 |
| ŌĆāAlar width bilateral | 47.88 ┬▒ 5.07 | 52.12 ┬▒ 4.34 | 47.9 ┬▒ 6.1 |
| ŌĆāS1 body width | 59.14 ┬▒ 3.4 | 56.45 ┬▒ 3.47 | 53.89 ┬▒ 4.62 |
| ŌĆāFacet depth | 13.98 ┬▒ 2.7 | 15.24 ┬▒ 2.9 | 15.88 ┬▒ 3.62 |
| Surface area (cm2) | |||
| ŌĆāAuricular surface area | 10.98 ┬▒ 1.78 | 10.36 ┬▒ 1.86 | 10.06 ┬▒ 1.58 |
| ŌĆāSuperior surface area | 9.85 ┬▒ 2.3 | 10.02 ┬▒ 2.35 | 9.89 ┬▒ 2.82 |
| ŌĆāFacet surface area | 1.52 ┬▒ 0.48 | 1.71 ┬▒ 0.51 | 1.77 ┬▒ 0.48 |
| Transverse element obliquity & thickness | |||
| ŌĆāS1 obliquity of the upper osseous corridor (┬░) | 16.64 ┬▒ 2.40 | 25.30 ┬▒ 3.79 | 30.6* ┬▒ 5.82 |
| 33.0* ┬▒ 4.33 | |||
| ŌĆāS1 craniocaudal thickness (mm) | 21.90 ┬▒ 3.41 | 19.40 ┬▒ 4.88 | 21.10 ┬▒ 2.39 |
| 13.88* ┬▒ 3.45 | |||
| ŌĆāS2 craniocaudal thickness (mm) | 14.56 ┬▒ 3.14 | 13.60 ┬▒ 2.45 | 15.64 ┬▒ 2.67 |
| 19.48* ┬▒ 3.40 |
REFERENCES

- Related articles in NS
-
Journal Impact Factor 3.2



























