 |
 |
- Search
| Neurospine > Volume 16(4); 2019 > Article |
|
|
Abstract
Objective
To study the association of facet joint angulation and joint tropism with degenerative spondylolisthesis (DS) through a comparison with a matched control group.
Methods
This radiographic study was carried out in 2 groups of 45 patients each. Group A contained patients with single-level DS, while group B (control) contained non-DS patients with similar age and degeneration who underwent surgery for disc prolapse or lumbar stenosis. DS was diagnosed based on translation of ≥ 3 mm on standing lateral radiography. Axial magnetic resonance imaging from L3 to S1 was utilized to assess the angulation of facet joints in relation to the coronal plane; a difference of ≥ 8° was considered to indicate tropism.
Results
Among 45 patients with DS, 15 were males and 30 females. Their mean age was 62.2 years. Facet tropism was identified in 20 of 45 patients at the level of DS, 12 patients at a level proximal to DS, and 15 patients at a level distal to DS. Facet tropism was found in 7 of the 45 patients in group B. At L3–4, facet tropism was observed in 13 patients (28.88%) in group A and 2 (4.44%) in group B. At L4–5, tropism was observed in 19 patients (42.22%) in group A and 5 (11.11%) in group B. At L5–S1, tropism was seen in 17 patients (37.77%) in group A and 2 (4.44%) in group B. Group A showed a significantly higher prevalence of multilevel facet tropism and tropism at levels adjacent to the DS level. A higher average angulation of facet joints was observed in the DS group, but the difference was not statistically significant at all levels.
Conclusion
The present study documented a statistically significant relationship between facet tropism and DS. A higher prevalence of facet tropism was also found in DS patients at non-DS levels, which is a novel observation. This finding supports the argument that facet tropism is a pre-existing morphological variation contributing to the development of DS, not a result of secondary remodelling.
Degenerative spondylolisthesis (DS) is common disorder of middle and old age. DS most commonly occurs at L4–5 level and more common in women than in men [1]. Several predisposing factors have been found to be associated with development of DS, facet joint orientation being one of them [2-4].
The facet joints play a critical role in maintaining stability of the lumbar spine by sharing load in compression and extension, and protecting the disc from excessive shear and rotational forces. Determined by their spatial orientation, facet joints also guide motion between 2 adjacent vertebrae. Their oblique orientation in the lumbar spine allows flexion, extension, and lateral bending, but only a small amount of axial rotation [5-7]. It has been shown that in patients with DS, the facet joints are significantly more sagitally oriented, thus allowing the superior vertebra to glide anteriorly. Individuals with sagitally oriented facet joints have therefore been regarded as prone for development of DS [2,8].
Facet tropism is defined as asymmetry between left and right facet joint orientation, a difference of 8° or more is considered as tropism [9]. Recently, there have been multicentre studies [9,10] on this topic, however, the scope of these studies was limited by the fact that they did not include any control group without DS at any level. We aim to study the facet joint angulation and presence of facet tropism in patients with DS and compare it with a control group of patients without DS at any level.
This is a retrospective radiographic study of facet joint orientation in patients of DS and control group comprising of patients with degenerative lumbar stenosis or disc prolapse without DS, operated at our hospital from 1st January 2014 to 31st December 2016.
Group A included 45 consecutive patients with single-level DS. DS was diagnosed with a 3 mm or greater slip-on lateral standing plain radiographs [3]. The main clinical features in this group were low back pain, neurogenic claudication, leg pain with or without neurological involvement (Table 1). Group B was an age and sex-matched control group comprising of 45 patients, who were operated for disc prolapse or stenosis, but without DS at any level. The common clinical features in this group were radicular pain, neurogenic claudication with or without neurological involvement. For selecting the control group, all patients with lumbar degenerative spine without spondylolisthesis which were operated at our institute during the abovementioned study period were listed as per their age and sex. Now for each patient in group A, we selected a patient of same age (± 1 year if exact same age was not available) and sex from the selected group, to be included as control in group B. The observer involved in this matching process was blinded to patient’s images and all other characteristics. The reason for selecting such a control group is to include patients with similar age, sex and degeneration but without lysthesis, and thus eliminating these confounding factors [11]. Exclusion criteria included patients with previous spinal surgery, congenital anomalies, transitional vertebrae, previous infection, trauma, tumours, isthmic spondylolisthesis, degenerative lumbar scoliosis and unsatisfactory imaging.
The study was approved by the Institutional Review Board (IRB) of P D Hinduja Hospital and Medical Research Center (1084-17-SD MRC). Waiver of consent obtained from IRB since this is an observational radiographic study.
Magnetic resonance images of lumbar spine were obtained. Axial images were selected at each disc level L3–4, L4–5, L5–S1, such that the magnetic resonance imaging cut included the posterior/superior corner of caudal vertebral body. This particular level has been shown to closely bisect the facet joint, and hence ideal for measurement [2,10].
Images were processed via the picture archiving and collecting system (PACS) used in our hospital, and the PACS software (AGFA Healthcare ICIS view 2014.1) was used to calculate the angles. The angle formed by the line along the posterior border of vertebral body in the coronal plane, with the line bisecting the superior and inferior tips of facet joint process was taken as facet joint angle (Fig. 1). If the difference in angulation of either facet joints was 8° or more, it was considered as facet tropism [9]. Assessment of all the images was carried out by an independent observer who was not part of patient management and who was blinded to whether the image belonged to the case or control group.
Prevalence of facet tropism was studied at L3–4, L4–5, and L5–S1 levels in both groups A and B. MedCalc Statistical Software ver. 17.1 (MedCalc Software bvba, Ostend, Belgium; https://www.medcalc.org) was used to analyse data. Pearson chi-square test and odds ratio were calculated. Statistical analysis was also carried out for the orientation of facet joints at all 3 levels in both groups. Values of p< 0.05 was taken as significant.
Among 45 patients with DS, 15 were males and 30 females. Mean age was 62.2 years (38–79 years). Most common level of DS was L4–5.
In group A, 4 of 45 patients (8.8%) had DS at L3–4. Out of these, 2 patients (50%) had facet tropism at index level and all 4 had facet tropism at adjacent distal level. Thirty-seven patients (82.2%) had DS at L4–5. Out of which, 14 patients (37.8%) had facet tropism at index level, 11 patients (29.7%) had tropism at adjacent proximal level and 11 patients (29.7%) had tropism at adjacent distal level (Fig. 2). Four patients (8.8%) had DS at L5–S1 level. All 4 patients (100%) had facet tropism at index level and 1 patient had tropism at adjacent L4–5 level also.
Prevalence of facet tropism in group A: Facet tropism was identified in 20 of 45 patients (44.4%) at the level of DS. It was also noted that 12 patients (26.6%) had facet tropism at level proximal to DS level and 15 patients (33.3%) at level distal to the DS level. Nineteen patients (42.2%) had tropism at single level, 9 patients (20%) had 2 level tropism and 4 patients (8.8%) had tropism at all 3 levels. Hence, among 45 patients with DS, 32 (71.1%) had facet tropism at either 1 or more levels.
The mean angulation of facet joints at L3–4 was 57.8°± 10.1° on left and 59.6°± 9.8° on right, at L4–5 it was 54.2°± 13.8° on left and 54.1°± 12.1° on right. At L5–S1 it was 44.4°± 10.2° on left and 43.6°± 10.9° on right (Table 2).
Among 45 patients in the control group without DS, 15 were males and 30 females. Mean age was 62.1 years (38–79 years).
Among group B, 2 patients (4.4%) had facet tropism at L3–4, 5 patients (11.1%) had tropism at L4–5 and 2 patients (4.4%) had tropism at L5–S1 level. Five patients (11.1%) had tropism at single level, while 2 patients (4.4%) had tropism at 2 levels. There was no patient with tropism at all 3 levels. Hence, facet tropism was observed in total 7 patients (15.5%) in group B.
The mean angulation of facet joints at L3–4 was 52.2°± 10.3° on left and 54.4°± 10.1° on right, at L4–5 it was 48.5°± 11.1° on left and 49.8°± 10.1° on right. At L5–S1 it was 44.4°± 8.5° on left and 44.1°± 8.1° on right (Table 2).
The prevalence of facet tropism was compared among both the groups, at each individual level, L3–4, L4–5, and L5–S1, irrespective of the level of DS (Fig. 3). At L3–4 facet tropism was observed in 13 patients (28.8%) in group A, as compared to 2 (4.4%) in group B. At L4–5, tropism was observed in 19 patients (42.2%) in group A and 5 (11.1%) in group B. At L5–S1, tropism was seen in 17 patients (37.7%) in group A and 2 (4.4%) in group B. Fischer exact test was found to be statistically significant at all 3 levels (Table 3). Odds ratio was found to be 8.73, 5.84, and 13.05, respectively at L3–4, L4–5, and L5–S1.
Facet joint angulation was studied at all 3 levels and compared between groups A and B (Table 2). We observed that mean facet joint angulation was higher in group A as compared to group B at L3–4 and L4–5, while it was similar in both groups at L5– S1. The difference was statistically significant at L3–4 level and left L4–5 only.
DS is a common spine disorder of middle and old age, often presenting as back pain, radiating pain or neurogenic claudication. It is more common in females [1] and L4–5 is the most common level affected [2-4]. Several factors have been proposed to be predisposing this condition, including hormonal and biomechanical factors [2,3]. Kirkaldy-Willis et al. [12] have described how the degenerative cascade of spine begins with the intervertebral disc degeneration, which alters the biomechanics of the motion segment, leading to overloading of facet joints. It is the failure or remodelling of facet joints which ultimately leads to development of DS.
The role of facet joint orientation and presence of joint tropism in the development of DS has been a matter of debate. Devine et al. [13], in a systematic review, reported no significant relationship between tropism and DS. Berlemann et al. [3] had observed that facet joint orientation was more sagittal at L4–5 in patients with DS as compared to patients without DS. They attributed this to a secondary remodelling of the joint orientation rather than a pre-existing morphological feature. However, Samartzis et al. [9], in a multicentric large-scale study involving 349 patients of single-level DS, found significant association between facet tropism and DS. The scope of this study was limited by the fact that there was no control group without DS for comparison, and possible interobserver variability as it was carried out in multiple centres.
The present study is a retrospective radiographic analysis, comparing the prevalence of facet tropism in patients with single-level DS with a matched control group without evidence of DS at any level. The reason for taking a sex- and age-matched control group and patients operated for degenerative lumbar spine is to neutralise these confounding factors [11]. The most common level of DS in our study was L4–5. Facet tropism was observed in 44.44% patients at the level of DS. It is interesting to note that among group A, facet tropism was also found in a significant number of patients at adjacent non-DS levels. Thus, presence of facet tropism might influence development of DS not only at the corresponding level, but it is also likely to influence the biomechanics at adjacent proximal or distal levels. So, we have compared the prevalence of facet tropism between the 2 groups, at all 3 levels, irrespective of the level of DS. We observed that the prevalence of tropism was higher in group A at levels L3–4, L4–5, and L5–S1 as compared to corresponding levels in group B; and this difference was found to be statistically significant.
We have found that in the present study, the prevalence of multiple level tropism was significantly higher among patients with DS as compared with the control group. Among group A (patients with DS), 20% had facet tropism at 2 levels and 8.88% had tropism at all 3 levels. While among group B (patients without DS), 4.44% had tropism at 2 levels and none of the patients had tropism at all 3 levels. Samartzis et al. [10] have compared a group of patients with DS at L4–5 with a group of patients with DS at a level other than L4–5, as control group. They have observed that more sagitally oriented facet joints were associated with L4–5 DS and proposed a critical value of 58° or greater for the facet joint angulation, above which the likelihood of L4–5 DS increases significantly. In the present study, our control group comprises of patients without DS at any level. Here, the average angulation of facet joints was observed to be higher in group A at L3–4 and L4–5 as compared with group B while it was similar in both groups at L5–S1 level. While this observation partially supports the claims of previous studies; that, more sagitally oriented facet joints may be associated with development of DS, we could not get statistically significant difference at all levels. Sagitally oriented facets seem to have a higher preponderance for developing DS at L3–4 and L4–5, while at L5–S1, the orientation of facet joints does not seem to increase the risk of DS. This may be because of additional stabilizing structures at L5–S1, which is also the reason why DS is overall less common at L5–S1.
Difference in orientation of left and right facet joints can create an asymmetrical stress distribution in the intervertebral disc and zygapophyseal tissues. Cyron and Hulton [14], through their cadaveric study, concluded that a relative axial rotation caused by facet asymmetry places higher compressive load on the facet that has the smallest orientation and could add rotational stress on the contralateral side of the annulus fibrosus and in the contralateral facet capsule, thereby accelerating the degenerative process. Any asymmetrical loading of the facet joints contributes to the development of facet osteophytes, cartilage erosion, fibrillation, or denudation, as well as narrowing of the joint space and neural foramen [15].
In our study, DS has a statistically significant association with presence of facet tropism. It should also be noted that facet tropism was found to be more prevalent in DS group than control group even at levels non-DS. This indicates that facet tropism at one level may influence development of DS not only at corresponding level, but at adjacent levels also. We consider that a patient with single-level DS does not have only a single isolated spinal unit which is abnormal/dysfunctional. Rather, this is a global disorder of spine and hence our study should not be limited to a single spinal segment. These patients need close followup as adjacent segments are likely to become symptomatic over a period of time. Several biomechanical [16] and clinical studies [17] have shown that presence of facet tropism at adjacent segment influences the biomechanics at that level and results in increased risk of adjacent segment disorder as well as spondylolisthesis at adjacent segment. With this context, it may be argued that these patients with tropism at adjacent non-DS levels might be prone to early development of adjacent segment degeneration. Further study with a long-term follow-up of these patients would be required to ascertain whether this subset of patients is more prone to develop degeneration at adjacent level and whether the plan of management needs to be modified in these cases.
The present study while reinforcing the relationship between facet joint tropism and DS; also outlines the novel finding of a higher prevalence of facet joint tropism at adjacent non-DS levels, in patients with DS. This observation supports the argument of facet tropism being a pre-existing morphology contributing to development of DS; and not a result of secondary remodelling. Whether the subset of patients with facet tropism at adjacent non-DS levels are at increased risk of developing adjacent segment degeneration and/or instability after surgical treatment of DS level, remains to be evaluated.
ACKNOWLEDGEMENTS
This study was presented in the Annual Conference of Association of Spine Surgeons of India at Hyderabad in 2017.
Fig. 1.
(a) Showing facet joint angulation measurement in a patient. The angle formed by line AB and line ED is the right facet joint angulation which is 51°. The angle formed by the line AB and line CF is the left joint angulation which is 49°. The difference being 2°, there is no facet tropism. (b) Showing facet joint angulation measurement in a patient. The angle formed by line AB and line CD is the right facet joint angulation which is 54°. The angle formed by the line AB and line EF is the left joint angulation which is 39°. The difference being 15°, there is facet tropism at this level.

Fig. 2.
Comparing prevalence of facet joint tropism in patients with degenerative spondylolisthesis (DS) at L4–5 (n = 37) in group A with corresponding levels in control group B (n= 45). It is noteworthy to observe the presence of joint tropism at adjacent non-DS levels in a significant number of patients of group A. Group A, patients with single-level degenerative spondylolisthesis; group B, control.
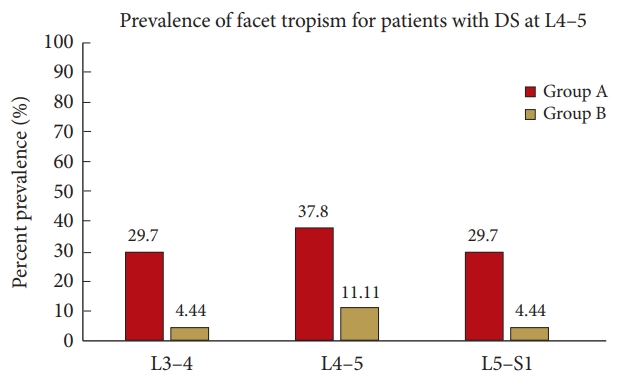
Fig. 3.
Prevalence of facet tropism is compared at each corresponding level among groups A and B, irrespective of the level of degenerative spondylolisthesis, and the differences are statistically significant. Group A, patients with single-level degenerative spondylolisthesis; group B, control.
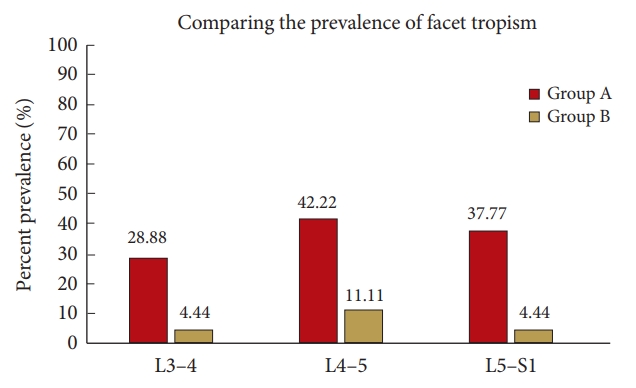
Table 1.
Characteristics of patients in groups A and B
Table 2.
Showing significant difference in mean facet joint angulation
| Level | Facet joint angulation | p-value |
|---|---|---|
| L3–4 Right | 0.015* | |
| Grade A | 59.6 ± 9.8 (45-80) | |
| Grade B | 54.4 ± 10.1 (37-85) | |
| L3–4 Left | 0.011* | |
| Grade A | 57.8 ± 10.1 (36-81) | |
| Grade B | 52.2 ± 10.3 (35-83) | |
| L4–5 Right | 0.068 | |
| Grade A | 54.1 ± 12.1 (25-82) | |
| Grade B | 49.8 ± 10.1 (40-75) | |
| L4–5 Left | 0.035* | |
| Grade A | 54.2 ± 13.8 (22-94) | |
| Grade B | 48.5 ± 11.1 (34-72) | |
| L5–S1 Right | 0.786 | |
| Grade A | 43.6 ± 10.9 (21-72) | |
| Grade B | 44.1 ± 8.1 (38-65) | |
| L5–S1 Left | 0.973 | |
| Grade A | 44.4 ± 10.2 (26-73) | |
| Grade B | 44.4 ± 8.5 (39-66) |
Table 3.
Shows the prevalence of facet tropism is significantly higher in group A at all 3 levels
| Facet tropism present | Group A (n = 45) | Group B (n = 45) | p-value* | Odds ratio |
|---|---|---|---|---|
| L3–4 | 13 | 2 | 0.002 | 8.73 |
| L4–5 | 19 | 5 | 0.001 | 5.84 |
| L5–S1 | 17 | 2 | 0.0001 | 13.05 |
REFERENCES
1. Rosenberg NJ. Degenerative spondylolisthesis. Predisposing factors. J Bone Joint Surg Am 1975 57:467-74.


2. Grobler LJ, Robertson PA, Novotny JE, et al. Etiology of spondylolisthesis. Assessment of the role played by lumbar facet joint morphology. Spine (Phila Pa 1976) 1993 18:80-91.


3. Berlemann U, Jeszenszky DJ, Bühler DW, et al. The role of lumbar lordosis, vertebral end-plate inclination, disc height, and facet orientation in degenerative spondylolisthesis. J Spinal Disord 1999 12:68-73.


4. Sato K, Wakamatsu E, Yoshizumi A, et al. The configuration of the laminas and facet joints in degenerative spondylolisthesis. A clinicoradiologic study. Spine (Phila Pa 1976) 1989 14:1265-71.


5. Adams MA, Hutton WC. The effect of posture on the role of the apophysial joints in resisting intervertebral compressive forces. J Bone Joint Surg Br 1980 62:358-62.


6. Haher TR, O'Brien M, Dryer JW, et al. The role of the lumbar facet joints in spinal stability. Identification of alternative paths of loading. Spine (Phila Pa 1976) 1994 19:2667-70.


7. Sharma M, Langrana NA, Rodriguez J. Role of ligaments and facets in lumbar spinal stability. Spine (Phila Pa 1976) 1995 20:887-900.


8. Gao F, Hou D, Zhao B, et al. The pedicle-facet angle and tropism in the sagittal plane in degenerative spondylolisthesis: a computed tomography study using multiplanar reformations techniques. J Spinal Disord Tech 2012 25:E18-22.


9. Samartzis D, Cheung JP, Rajasekaran S, et al. Is lumbar facet joint tropism developmental or secondary to degeneration? An international, large-scale multicenter study by the AOSpine Asia Pacific Research Collaboration Consortium. Scoliosis Spinal Disord 2016 11:9.




10. Samartzis D, Cheung JP, Rajasekaran S, et al. Critical values of facet joint angulation and tropism in the development of lumbar degenerative spondylolisthesis: an international, large scale multicentre study by the AO Spine Asia Pacific Research Collaboration Consortium. Global Spine J 2016 6:414-21.


11. Dai LY. Orientation and tropism of lumbar facet joints in degenerative spondylolisthesis. Int Orthop 2001 25:40-2.




12. Kirkaldy-Willis WH, Wedge JH, Yong-Hing K, et al. Pathology and pathogenesis of lumbar spondylosis and stenosis. Spine (Phila Pa 1976) 1978 3:319-28.


13. Devine JG, Schenk-Kisser JM, Skelly AC. Risk factors for degenerative spondylolisthesis: a systematic review. Evid Based Spine Care J 2012 3:25-34.




14. Cyron BM, Hutton WC. Articular tropism and stability of the lumbar spine. Spine (Phila Pa 1976) 1980 5:168-72.


15. Gallucci M, Puglielli E, Splendiani A, et al. Degenerative disorders of the spine. Eur Radiol 2005 15:591-8.




- TOOLS
- Related articles in NS
-
Journal Impact Factor 3.2



























