Surgery for Recurrent Lumbar Disc Herniation During Pregnancy: A Case Report
Article information
Abstract
A few cases of lumbar disc herniation (LDH) that have been treated by surgery during pregnancy have been reported in the literature. However, symptomatic recurrent LDH during pregnancy has been rarely reported. A 32-year-old parous woman presented with lumbago and severe right leg pain at 20 weeks' gestation. Eleven years prior to admission, she had undergone an open discectomy for right-sided LDH at the L4-5 level. Magnetic resonance imaging (MRI) showed a recurrent disc herniation that affected the nerve root at the right L4-5 level. The radiating pain did not respond to conservative treat-ment. Revision surgery was performed under general anesthesia and in the left lateral position to avoid fetal stress and aortocaval compression, and the ruptured disc particle was completely removed. Postoperatively, the radiating pain was completely relieved. She delivered a full-term healthy girl (birth weight, 3.39 kg) at 40 weeks' gestation by normal vaginal delivery. We report the rare case of a 32-year-old parous woman with recurrent LDH that was successfully treated by revision surgery. In recurrent LDH patients with incapacitating pain who do not respond to opioid injections, surgical treat-ment could lead to a satisfactory outcome maintaining pregnancy.
INTRODUCTION
Low back pain is a common complication of pregnancy, occurring in approximately 50% of women during gestation4,11). However, the incidence of symptomatic LDH is very rare (approximately 1 in 10,000 pregnancies)10). A few cases of LDH treated by surgery during pregnancy have been reported in the literature1,2,5,9). However, symptomatic recurrent LDH has been rarely reported during pregnancy. We report a rare case of a 32-year-old parous woman with recurrent LDH that was successfully treated by revision surgery.
CASE REPORT
A 32-year-old parous woman presented with lumbago and severe right leg pain at 20 weeks' gestation. She had a history of laminectomy and pedicle screw fixation at the L2-3-4 level for an L3 burst fracture in 1998. She had undergone open discectomy for right-sided lumbar disc herniation at the L4-5 level and hardware removal in 1999 at another hospital. Two months prior to admission, the patient experienced new radiating pain in the right leg and conservative management was performed. When the leg pain was further aggravated, she was admitted to the obstetric department for evaluation of the leg pain.
The physical examination showed severe radiating pain and hypesthesia on the right L5 dermatome. Motor function was intact. Straight leg raising test was positive on 15 degrees. MRI showed recurrent disc herniation that affected the nerve root at the right L4-5 level, and the old L3 burst fracture with laminectomy state (Fig. 1, 2).

Sagittal (A) and axial (B) T2-wighted magnetic resonance images showing recurrent lumbar disc herniation with previous laminectomy at the L4-5 level and the previous L3 burst fracture with laminectomy.
The patient was unable to walk or sleep because of the incapacitating pain (visual analog scale: 8 points). The pain was not relieved by opioid injections. We decided to perform surgical treatment at 21 weeks' gestational age. The surgery was performed under general anesthesia and in the left lateral position to avoid fetal stress and aortocaval compression (Fig. 3). Right extended medial facetectomy and adhesiolysis were performed under microscopy. The ruptured disc particle was completely removed. Intraoperative fetal heart monitoring (FHM) was attempted before the operation. However, FHM was unsuccessful because the surgery was performed in the lateral position and due to the relatively small size of the fetus at 21 weeks' gestation. Therefore, instead of FHM, an ultrasonography was immediately performed in the recovery room, and the fetal condition was confirmed to be good.
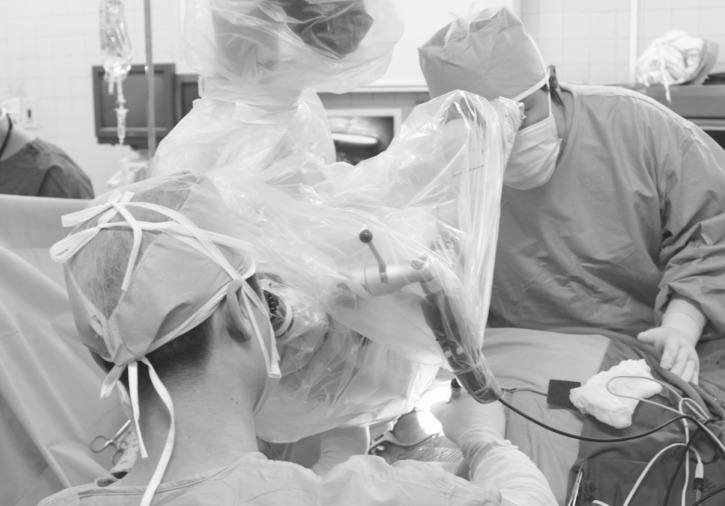
Intraoperative photograph acquired during surgery. Microdiscectomy is being performed in the left lateral position, and the table is slightly tilted for avoiding aortocaval compression and for providing a better surgical view.
Postoperatively, the radiating pain was completely relieved. The patient delivered a full-term healthy girl (birth weight, 3.39 kg) at 40 weeks' gestation by normal spontaneous vaginal delivery. After 1 year after the surgery, she had no pain and recurrence.
DISCUSSION
Although LDH is the most common spinal pathological condition in pregnancy, the disorder is very rare, occurring in approximately 1 in 10,000 pregnancies10). A few cases of LDH treated by surgery during pregnancy have been reported in the literature1,2,5,9). In the young female population, surgery for LHD is not common, particularly in the first and second decade of life3,12,14). Therefore, symptomatic recurrence of LDH during pregnancy is extremely rare. The incidence of LDH is probably not increased by pregnancy, and recurrence of LDH is a common complication after surgery for LDH18). Therefore, in our case, the recurrence of LDH cannot be fully explained by the effects of pregnancy. However, the patient had already undergone fusion surgery for L3 burst fracture, and therefore had a predisposing factor for recurrent LDH due to the increased load at the adjacent segments. Additionally, the enlarged uterus, which causes an anterior shift of the center of gravity, might have resulted in further strain on the intervertebral disc. We suggest that the combination of adjacent fusion surgery and an enlarged uterus may have caused an increased load on the intervertebral disc weakened by a previous discectomy, and this might have resulted in the recurrence of LDH during pregnancy.
Surgical indications for LDH in pregnant women are not different from those in the general population. Absolute indications are cauda equina syndrome or progressive motor weakness. In addition, if the patient experiencing incapacitating pain does not respond to conservative treatment, surgical treatment can be also performed4,5,16). In particular, as seen in our case, when incapacitating pain is not relieved by opioid injection, surgical treatment should be actively considered; this is because the high levels of maternal stress may increase the risk of abortion or preterm birth6,15).
For pregnant women with LDH, epidural anesthesia is usually recommended because it is safe during any age of gestation2,5). However, in our case, general anesthesia was performed because the operating time for revision surgery could have been longer if postoperative adhesion or unexpected dural laceration occurred. In operation for recurrent LDH, other special regards for pregnancy are not different from primary LDH. The lateral surgical position was selected to avoid aortocaval compression by the gravid uterus during the second trimester, and the operative table was slightly tilted for better surgical approach. However, during the first and early part of the second trimester, surgery can be performed in the prone position because there is minimal aortocaval compression5,7,17). In addition, intraoperative FHM is very important to ensure fetal safety during surgery8). In our case, FHM was attempted prior to the operation by an obstetrician. However, FHM was unsuccessful because of the small size of the fetus at 21 weeks' gestation and because the surgery was performed in the lateral position. Indeed, FHM is indicated after 23 weeks' gestation, and its use between 20 and 23 weeks' gestation is still controversial. In such cases, immediate postoperative ultrasonography can be performed as a substitute for FHM.
Symptomatic recurrent LDH has been rarely reported in pregnant women. However, LDHs are most common in individuals aged 35-55 years, and the mean age of pregnant women has increased in recent years13,18). In addition, lumbar discectomy has been commonly performed in a young and active population3). Thus, the number of reports on primary LDHs and recurrent LDHs in pregnant women can be expected to increase in the future.
CONCLUSION
We report a rare case of a 32-year-old parous woman with recurrent LDH that was successfully treated by revision surgery. Because surgery for LDH has been commonly performed in the young and active population and because the mean age of pregnant women has recently increased, the number of reports on recurrent LDH in pregnant women is expected to increase in the future. In recurrent LDH patients with incapacitating pain who do not respond to conservative management, surgical treatment may lead to a satisfactory outcome maintaining pregnancy.
Notes
This study was supported by clincal research grant (2011), Pusan National University Hospital.
