 |
 |
- Search
|
|
||
Abstract
Objective
The purpose of this study was to compare the effect of atlantoaxial fixation on cervical alignment and clinical outcomes in patients with os odontoideum (OO) versus non-os odontoideum (non-OO).
Methods
A total of 119 patients who underwent atlantoaxial fixation for instability were identified between January 1998 and January 2014. Inclusion criteria included age more than 21 years and diagnosis of OO and non-OO. There were 22 OO patients, and 20 non-OO patients. Measuring the Oc–C1 Cobb angle, C1–2 Cobb angle, C2–7 Cobb angle, and C2–7 sagittal vertical axis (SVA) was assessed. Clinical outcome was assessment of suboccipital pain was determined using a visual analogue scale (VAS), and Japanese Orthopedic Association (JOA) scores were obtained in all patients pre- and postoperatively.
Results
The preoperative C1–2 angle in the OO group (26.02°±10.53°) was significantly higher than the non-OO group (p=0.04). After C1–2 fixation, the OO group had significantly higher kyphotic change in the C1–2 angle (ΔC1–2) (3.2°±7.3° [OO] vs. −1.46°±7.21° [non-OO]) (p=0.04), and higher decrease in postoperative C2–7 SVA (ΔC2–7 SVA) (5.64±11.56 mm [OO] vs. −0.51± 6.57 mm [non-OO]) (p=0.04). Both groups showed improvements in the health related quality of life (HRQOL) after surgery based on the VAS and JOA score (p<0.001).
Atlantoaxial articulation is unique part with full range of motion in the spine which depends on ligamentous support and the integrity of the odontoid for its stability. The etiology of atlantoaxial instability includes trauma, congenital malformations, os odontoideum (OO), rheumatoid arthritis, malignancies and skeletal dysplasias. OO is an anomaly defined as an ossicle with smooth circumscribed margins and no osseous continuity with the body of C28,10,20). It was firstly described in 1886 by Giacomini and is a cause of atlantoaxial instability in pediatric patients. Current evidence points to traumatic etiologies in the majority of patients2,17). OO is difficult to treat when associated with cervicomedullary compression, long-term displacement, and myelopathy. There is currently no consensus regarding the optimal management of OO. For asymptomatic OO, some have advocated regular clinical and radiological examinations and if there is evidence of C1–2 instability, to proceed with surgical stabilization1,4). However, few reports have elucidated the cervical sagittal alignment of OO patients versus non-OO patients after an atlantoaxial fixation procedure. Moreover, the biomechanical effect of C1–2 fixation on adjacent segments remains unknown13,26). In this investigation, we studied the effect of atlantoaxial fixation on cervical sagittal alignment, as well as range of motion between OO and non-OO patients.
Between 1998 and 2014, 245 patients with atlantoaxial instability were registered in the Yonsei University Medical Center database. A total of 119 patients who underwent AA fixation by transarticular (TAS) and screw-rod construct (SRC) technique were identified. Patients with any injuries that precluded them from being able to obtain flexion and extension radiographs were also excluded. There were 22 OO patients, and 20 non-OO patients, which included 6 patients with rheumatoid arthritis, 11 degenerative patients, and 3 patients with trauma. Regular follow-up was performed at 3, 12, 24, 36, 48, 56, and 72 months following surgery. Occipitocervical fusion and other types of posterior atlantoaxial fixation procedures, including the use of atlantal trans-laminar screws, atlantoaxial interlaminar hooks/rods, and intra-articular screws with interlaminar clamps were excluded from the study. All radiographic and health related quality of life (HRQOL) data were reviewed. This study was approved by Yonsei University Institutional Review Board (IRB Number: 4-2017-0209).
The patients were placed in a prone position with the skull fixed by a Mayfield clamp. The neck was positioned to optimize access by flexing slightly at the occiput while extending the subaxial spine. An attempt was made to reduce the C1–2 articulation during this positioning process. Procedures were assisted by fluoroscopy. A midline incision was made over C1–2 but extended distally to allow the required drill angulation and the posterior aspects of C-1 and C-2 were fully exposed. Subperiosteal exposure of the C1 arch and C2 posterior elements was performed. A right-angled hook was used to palpate the medial walls of the C1 lateral mass and the C2 pars, to help guide for the screw. We placed the screw after reducing the subluxation and check final implant positioning by fluoroscopy. In TAS technique, iliac bone block was fixed via interlaminar wiring. In SRC, autologous bone graft was implanted
Pre- and postoperative radiographs were obtained in all patients in upright flexion, neutral, and extension positions. Postoperative radiographs were obtained approximately 2 years after surgery. Preoperative AA instability was documented in all patients by plain radiographs, dynamic flexion-extension radiographs, and computed tomography studies. Magnetic resonance imaging supplemented the evaluation in many cases to help define ligamentous disorders. The Oc–C1 angle was measured from the McGregor line drawn from the posterosuperior aspect of the hard palate to the most caudal point on the midline occipital curve and a line drawn parallel to the inferior aspect of C–1. The C1–2 angle was defined as the angle subtended by a line drawn parallel to the inferior aspect of C-1 and a line drawn parallel to the inferior endplate of C–2. Cervical lordosis (CL) was assessed by the C2–7 Cobb angle was defined as the angle subtended by a line drawn parallel to the inferior endplate of the C-2 vertebral body and a line drawn parallel to the inferior endplate of the C-7 vertebral body (Fig. 1). Implant failure was considered if there was an implant pullout, loosening or separation by plain X-ray, and fusion was suggested by the absence of motion on flexion and extension film and the presence of bridging bone on CT or plain X-ray. The Oc–C1, C1–2 and C2–7 angles were measured before and after surgery. The C2–7 SVA was defined as the distance from the posterosuperior corner of C7 and the vertical line from the center of the C2 body. Changes in the cervical alignment (Δ) were calculated with the following formula: alignment change (°)=(preoperative C2–7 Cobb angle)-(postoperative C2–7 Cobb angle), According to this formula, alignment changes >0° were considered postoperative loss of CL or kyphotic changes13,26). The difference between the pre- and postoperative C1–2 and C2–7 angles and the angle of atlantoaxial fixation was established. The extent of change in C2–7 was evaluated. In addition, the effect on adjacent segments was evaluated based on the extent of changes in Oc–C1 before and after surgery. These evaluations were performed between the OO and non-OO groups before and after surgery
The average patient age of the OO group was 43.68±15.50 years and the non-OO group was 52.95±14.82 years (p=0.06). There were 3 male and 19 female patients in the OO group and 9 male and 11 female patients in the non-OO group (p<0.01). An average follow-up in the OO group was 24.23±19.17 months and the non-OO group was 24.7±11.8 months (p=0.92) (Table 1).
In the OO group, there was a statistically significant decrease in the C1–2 Cobb angles (preoperative vs. postoperative) as well as changes of C1–2 angles (ΔC1–2) after surgery. The mean C1–2 Cobb angles in preoperative value was 26.02°±10.53° and significantly decreased to postoperative value of 22.82°±8.3° (p= 0.03) (Table 2). However, In the non-OO group, the mean pre-operative C1–2 Cobb angles was 19.76°±8.48° and postoperative C1–2 Cobb angles was 21.23°±7.85° (p=0.35) (Table 2). After C1–2 fixation, the OO group had significantly higher kyphotic change in the C1–2 angle (ΔC1–2) (3.2°±7.3° [OO] vs. −1.46°± 7.21° [non-OO]) (p=0.04) (Table 3).
In the non-OO group, there was a statistically significant decrease in the C2–7 Cobb angles (preoperative vs. postoperative). In the OO group, the mean C2–7 Cobb angles in preoperative value was 17.63°±13.61° and postoperative value was 15.63°± 4.2° (p=0.26). However, in the non-OO group, the mean C2–7 Cobb angles in preoperative value was 16.76°±9.44° and significantly decreased to postoperative value of 12.76°±9.14° (p= 0.01). There was also a statistically higher postoperative C2–7 ROM in the OO group than non-OO group (p=0.02) (Table 3).
In the OO group, there was a statistically significant higher preoperative C2–7 SVA value and change in C2–7 SVA after surgery (ΔC2–7 SVA) than the non-OO group. In the OO group, the mean C2–7 SVA in preoperative value was 19.36±10.31 mm and significantly decreased to postoperative value of 13.7±9.48 mm(p=0.02). In the non-OO group, the mean C2–7 SVA pre-operative value was 7.5±11.65 mm and postoperative value was 7.51±11.65 mm(p=0.45). The change in C2–7 SVA after surgery (ΔC2–7 SVA) was significantly higher in OO group (5.64±11.56 mm) than the non-OO group(−0.51±6.56 mm) (p=0.04) (Table 3).
In the OO group, the mean O–C1 Cobb angles in preoperative value was 11.3°±7.36° and postoperative value was 10.74°±6.44° (p=0.51). In the non-OO group, the mean O–C1 Cobb angles in preoperative value was 11.38°±6.89° and postoperative value was 8.43°±5.32° (p=0.01).
Results of HRQOL after surgery were summarized in Table 4. There were statistically significant improvements in the VAS after surgery in both groups (p<0.01). The mean VAS in the OO group was 4.87±2.13 before and 0.75±1 after surgery, and in the non-OO group, the mean VAS was 4.65±2.26 before and 1.11±1.02 after surgery. There were statistically significant improvements in the JOA scores in both groups (p<0.01). The mean JOA in the OO group was 15.31±1.2 before and 16.76±0.66 after surgery, and in the non-OO group, the mean JOA was 15.68±1.53 before and 16.8±0.89 after surgery.
OO with instability can be asymptomatic or present with a variety of symptoms, including occipital-cervical pain alone, myelopathy or intracranial symptoms or signs from vertebrobasilar ischemia21). Recent studies have reported that the atlantoaxial angle plays an important role in high cervical alignment14,16). Furthermore, there is a lack of evidence with regard to the most suitable parameter for predicting postoperative loss of lordosis after atlantoaxial fixation. A previous study hypothesized that common radiographic changes included an increase in C1–2 lordosis and a decrease in C2–7 lordosis, which are produced by C1–2 fixation and posterior musculoligamentous injury during posterior surgery3,9,23).
Previous studies reported that increase kyphosis in C1–2 after C1–2 fixation3,26). By contrast, in the present study, the mean C1–2 Cobb angle in the non-OO group was 19.76°±8.48° before surgery and 21.23°±7.85° after surgery (p=0.35), and the ΔC1–2 was −1.47°±7.21°. In the OO group, the C1–2 Cobb angle was 26.02°±10.5° before surgery and 22.8°±8.3° after surgery, and the ΔC1–2 was 3.2°±7.3° (p=0.04) (Table 3). These findings explain that the OO patients have preoperative lordotic posture in C1–2 angle than non-OO patients. Also, final C1–2 angle after the surgery were almost identical in both groups (21.23° in OO vs. 22.8° in non-OO) imply that the mechanical characteristics of C1–2 instrumentation could induce identical angle at C1–2 in both groups5,13,24,25).
The present study also found in the OO group that C2–7 SVA decreased from 19.36±10.31 mm to 13.7±9.48 mm (p=0.02) at the final follow up, along with high ΔC2–7 SVA in the OO group (p=0.04). In order to maintain horizontal gaze, cervical spine alignment and radiological parameters will change reciprocally. Therefore, our finding can be explained by secondary to the realignment after atlantoaxial loss of lordosis and posterior musculoligamentous injury which could decrease ΔC2–7 SVA.
In this study, both OO group and non-OO group decreased postoperative C2–7 Cobb angle. Our current findings in loss of CL at subaxial spine in both groups were similar to previous study11,12,15,16,23,27). Therefore, we support the hypothesis that the injury of musculoligamentous complex during the posterior cervical AA fixation may drive the cervical alignment to more kyphotic than preoperative value.
C2–7 ROM after surgery was higher in the OO group than the non-OO group. This current finding implies that the relatively younger patients population with less association with degenerative changes in the OO group may produce more C2–7 ROM after the surgery.
Although, it is still difficult to justify the relationship between AA fixation and CL, we could hypothesize from the summary of our results that the compensated higher cervical alignment in the OO group could have the potential to lead to greater SVA changes after surgery. After AA fixation, postoperative loss of lordosis was related to conditions, such as posterior muscle injury, age and degenerative change.
The present study reported that there are no differences in the fusion rate between the OO and non-OO groups, and the success rate of bony fusion was approximately 100% in both groups, which is similar to previous findings that reported6,7,22). A screw break in the OO group (4.5%[1 of 22]) in a previous study also resulted in implant failure18).
In this study, perioperative HRQOL after treatment was also significantly different pre- and postoperatively (VAS suboccipital, p<0.01; JOA, p<0.01). This indicates that surgical procedures for atlantoaxial instability are satisfactory in decreasing suboccipital pain and neurological symptoms, which is similar to findings from a previous study19).
Our study has some notable limitations, including its retrospective design, small sample size, and that it was not blinded also cervical T1 slope was not performed. In addition, selection bias and several confounding factors could affect our results. However, despite these limitations, our study demonstrated the radiological characteristics of OO and non-OO patients. Our study is valuable to understanding the relationship between AA fixation and loss of lordosis after fixation in patients with OO and non-OO. Therefore, more consecutive data and future prospective clinical studies will be needed.
ACKNOWLEDGMENTS
The authors would like to thank Dong-Su Jang, MFA(Medical Illustrator, Medical Research Support Section, Yonsei University College of Medicine, Seoul, Korea) for his help with the illustrations.
CONFLICT OF INTEREST
CONFLICT OF INTEREST
No potential conflict of interest relevant to this article was reported.
Fig. 1
Sagittal cervical alignment parameters. (a–b) Oc–C1 angle, (b–c) C1–2 angle, (d–e) C2–7 angles, and (f) C2–7 sagittal vertical axis (SVA) were measured between the lines shown in the figure. The Oc–C1 angle was calculated by subtracting the angle between the McGregor line and the line passing through the inferior aspect of the atlas in extension from that in the forward flexion. The C2–7 SVA was defined as the distance from the posterosuperior corner of C7 and the vertical line from the center of the C2 body. The C2–7 angle was calculated by subtracting the angle between the line drawn horizontal to the inferior endplate of the C–2 vertebral body and the line drawn horizontal to the inferior endplate of the C–7 vertebral body in extension from that in the forward flexion.
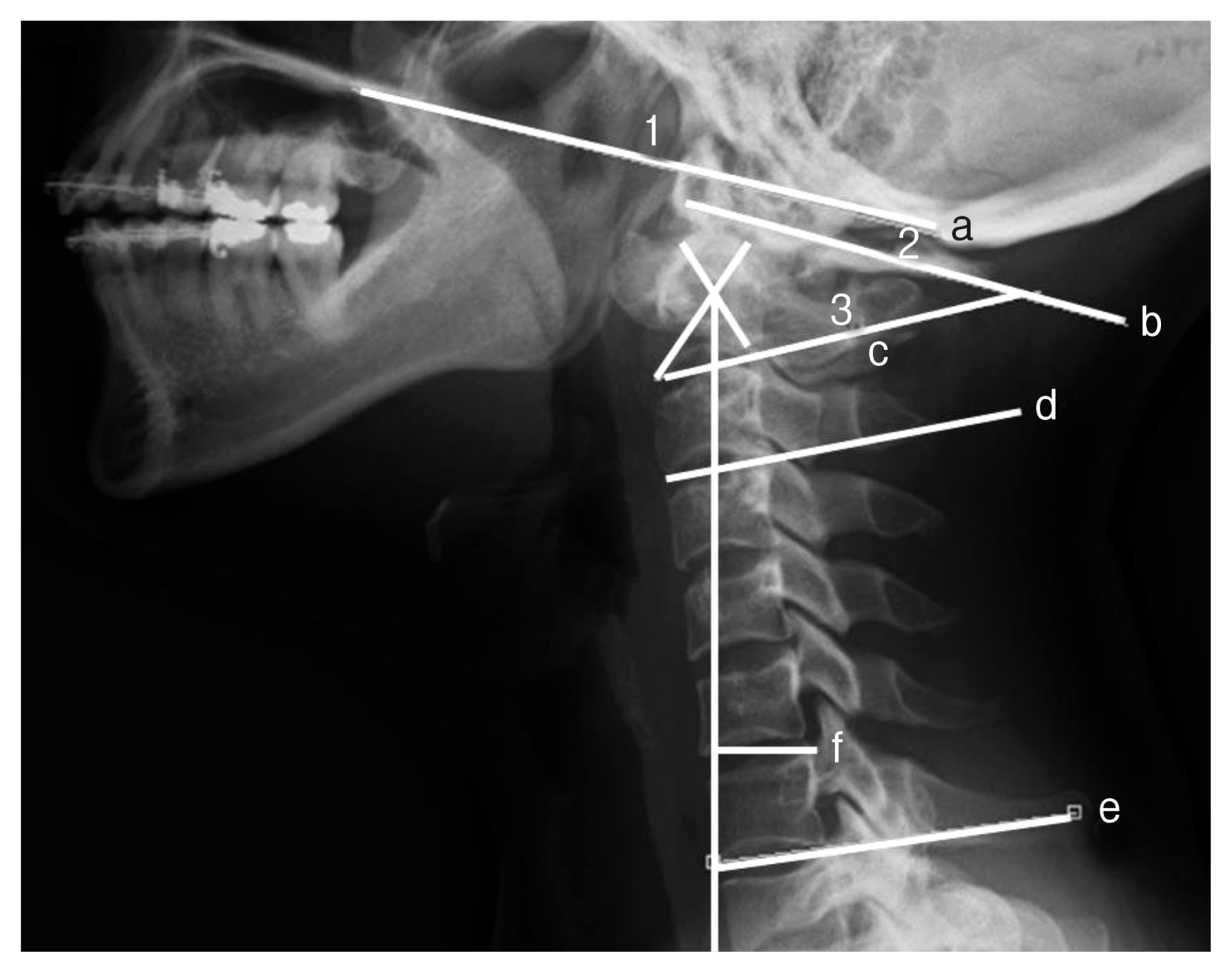
Table 1
Patients characteristics of OO and non-OO groups
| Characteristic | OO group (n=22) | Non-OO group (n=20) | p-value |
|---|---|---|---|
| Age (yr) | 43.68±15.50 | 52.95±14.82 | 0.06 |
| Follow-up time (mo) | 24.23±19.17 | 24.7±11.8 | 0.92 |
| Sex, male:female | 3:19 | 9:11 | <0.01* |
| Implant failure | 1 (4.5) | 2 (10) | 0.47 |
| Fusion | 22 (100) | 20 (100) | 0.96 |
Table 2
Comparison of sagittal parameters before and after surgery for each OO group and non-OO groups
| Parameter | Preoperative | Postoperative | p-value |
|---|---|---|---|
| OO group | |||
| O–C1 (°) | 11.3±7.36 | 10.74±6.44 | 0.51 |
| C1–2 (°) | 26.02±10.53 | 22.82±8.30 | 0.03* |
| C2–7 (°) | 17.63±13.61 | 15.63±4.20 | 0.26 |
| C2–7 SVA (mm) | 19.36±10.31 | 13.7±9.48 | 0.02* |
| O–C1 ROM (°) | 21.48±10.41 | 21.44±8.70 | 0.97 |
| C1–2 ROM (°) | 42.62±11.44 | 45.56±14.36 | 0.15 |
| C2–7 ROM (°) | 64.02±24.17 | 61.96±19.45 | 0.43 |
| Non-OO group | |||
| O–C1 (°) | 11.38±6.89 | 8.43±5.32 | 0.01* |
| C1–2 (°) | 19.76±8.48 | 21.23±7.85 | 0.35 |
| C2–7 (°) | 16.76±9.44 | 12.76±9.14 | 0.01* |
| C2–7 SVA (mm) | 7.5±11.65 | 7.51±11.65 | 0.45 |
| O–C1 ROM (°) | 19.97±11.80 | 18.8±8.92 | 0.50 |
| C1–2 ROM (°) | 44.19±14.54 | 43.28±17.42 | 0.77 |
| C2–7 ROM (°) | 53.89±19.91 | 57.7±16.22 | 0.05 |
Table 3
Summary of preoperative (preop) and postoperative (postop) characteristics of OO and non-OO groups
| OO group | Non-OO group | p-value | |
|---|---|---|---|
| O–C1 preop (°) | 11.29±7.35 | 11.38±6.89 | 0.97 |
| C1–2 preop (°) | 26.02±10.53 | 19.76±8.48 | 0.04* |
| C2–7 preop (°) | 17.63±13.61 | 16.76±9.44 | 0.81 |
| O–C1 postop (°) | 10.73±6.44 | 8.43±5.32 | 0.22 |
| ΔO–C1 (°) | 0.56±9.45 | 2.95±4.83 | 0.20 |
| C1–2 postop (°) | 22.82±8.29 | 21.23±7.85 | 0.53 |
| ΔC1–2 (°) | 3.2±7.33 | −1.47±7.21 | 0.04* |
| C2–7 postop (°) | 15.58±11.88 | 12.76±9.14 | 0.40 |
| ΔC2–7 (°) | 2.05±9.84 | 4.00±7.29 | 0.47 |
| C2–7 ROM postop (°) | 61.97±19.46 | 47.86±16.22 | 0.02* |
| C2–7 SVA preop (mm) | 19.36±10.31 | 7.50±11.65 | 0.00* |
| C2–7 SVA postop (mm) | 13.72±9.47 | 8.01±13.21 | 0.11 |
| ΔC2–7 SVA (mm) | 5.64±11.56 | −0.51±6.56 | 0.04* |
REFERENCES
1. Abd-El-Barr MM, Snyder BD, Emans JB, Proctor MR, Hedequist D. Combined preoperative traction with instrumented posterior occipitocervical fusion for severe ventral brainstem compression secondary to displaced os odontoideum: technical report of 2 cases. J Neurosurg Pediatr 25:724-729. 2016.


2. Akpolat YT, Fegale B, Cheng WK. Treatment of os odontoideum in a patient with spastic quadriplegic cerebral palsy. J Clin Neurosci 22:1239-1243. 2015.


3. Bahadur R, Goyal T, Dhatt SS, Tripathy SK. Transarticular screw fixation for atlantoaxial instability - modified Magerl’s technique in 38 patients. J Orthop Surg Res 5:872010.



4. Chung JC, Jung SS, Park KS, Ha HG. Intraoperative vertebral artery angiography to guide c1-2 transarticular screw fixation in a patient with athetoid cerebral palsy. J Korean Neurosurg Soc 51:177-181. 2012.



6. Goel A, Desai K, Muzumdar DP. Atlantoaxial fixation using plate and screw method: a report of 160 treated patients. Neurosurgery 51:1351-1356. 2002.


7. Goel A, Laheri V. Plate and screw fixation for atlanto-axial subluxation. Acta Neurochir (Wien) 129:47-53. 1994.


8. Grob D, Jeanneret B, Aebi M, Markwalder TM. Atlanto-axial fusion with transarticular screw fixation. J Bone Joint Surg Br 73:972-976. 1991.


9. Guo Q, Ni B, Yang J, Liu K, Sun Z, Zhou F, et al. Relation between alignments of upper and subaxial cervical spine: a radiological study. Arch Orthop Trauma Surg 131:857-862. 2011.


10. Ikuchi K, Nakagawa H, Watanabe K, Kowada M. Bilateral vertebral artery occlusion secondary to atlantoaxial dislocation with os odontoideum: implication for prophylactic cervical stabilization by fusion--case report. Neurol Med Chir (Tokyo) 33:769-773. 1993.


11. Johnson GM, Zhang M, Jones DG. The fine connective tissue architecture of the human ligamentum nuchae. Spine (Phila Pa 1976) 25:5-9. 2000.


12. Kim B, Yoon DH, Ha Y, Yi S, Shin DA, Lee CK, et al. Relationship between T1 slope and loss of lordosis after laminoplasty in patients with cervical ossification of the posterior longitudinal ligament. Spine J 16:219-225. 2016.


13. Klimo P Jr, Kan P, Rao G, Apfelbaum R, Brockmeyer D. Os odontoideum: presentation, diagnosis, and treatment in a series of 78 patients. J Neurosurg Spine 9:332-342. 2008.


14. Liu Q, Guo Q, Yang J, Zhang P, Xu T, Cheng X, et al. Subaxial cervical intradiscal pressure and segmental kinematics following atlantoaxial fixation in different angles. World Neurosurg 87:521-528. 2016.


15. Mukai Y, Hosono N, Sakaura H, Fujii R, Iwasaki M, Fuchiya T, et al. Sagittal alignment of the subaxial cervical spine after C1-C2 transarticular screw fixation in rheumatoid arthritis. J Spinal Disord Tech 20:436-441. 2007.


16. Nolan JP Jr, Sherk HH. Biomechanical evaluation of the extensor musculature of the cervical spine. Spine (Phila Pa 1976) 13:9-11. 1988.


17. Ohya J, Miyoshi K, Kitagawa T, Nakagawa S. Occipitalized os odontoideum: a case report. J Craniovertebr Junction Spine 5:170-172. 2014.



18. Okamoto T, Neo M, Fujibayashi S, Ito H, Takemoto M, Nakamura T. Mechanical implant failure in posterior cervical spine fusion. Eur Spine J 21:328-334. 2012.


19. Oshima S, Sudo H, Ito M, Abumi K. Subaxial sagittal alignment after atlantoaxial fixation techniques. J Spinal Disord Tech 28:E49-55. 2015.


20. Rahimizadeh A, Soufiani HF, Hassani V, Rahimizadeh A. Atlantoaxial subluxation due to an os odontoideum in an achondroplastic adult: report of a case and review of the literature. Case Rep Orthop 2015:1425862015.




21. Rozzelle CJ, Aarabi B, Dhall SS, Gelb DE, Hurlbert RJ, Ryken TC, et al. Os odontoideum. Neurosurgery 72(Suppl 2):159-169. 2013.



22. Suchomel P, Stulík J, Klézl Z, Chrobok J, Lukás R, Krbec M, et al. Transarticular fixation of C1-C2: a multicenter retrospective study. Acta Chir Orthop Traumatol Cech 71:6-12. 2004.

23. Takeshita K, Peterson ET, Bylski-Austrow D, Crawford AH, Nakamura K. The nuchal ligament restrains cervical spine flexion. Spine (Phila Pa 1976) 29:E388-393. 2004.


24. Toyama Y, Matsumoto M, Chiba K, Asazuma T, Suzuki N, Fujimura Y, et al. Realignment of postoperative cervical kyphosis in children by vertebral remodeling. Spine (Phila Pa 1976) 19:2565-2570. 1994.


25. Watanabe M, Toyama Y, Fujimura Y. Atlantoaxial instability in os odontoideum with myelopathy. Spine (Phila Pa 1976) 21:1435-1439. 1996.



- TOOLS
-
METRICS

-
- 3 Crossref
- Scopus
- 7,358 View
- 204 Download

























