|
 |
- Search
|
|
||
Abstract
Objective
Anterior cervical discectomy and fusion (ACDF) is the most common performed surgery in the cervical spine. Dysphagia is one of the most frequent complications following ACDF. Several studies have identified certain demographic and perioperative risk factors associated with increased dysphagia rates, but few have reported recent trends. Our study aims to report current trends and factors associated with the development of inpatient postoperative dysphagia after ACDF.
Methods
The National Inpatient Sample was evaluated from 2004 to 2014 and discharges with International Classification of Diseases procedure codes indicating ACDF were selected. Time trend series plots were created for the yearly treatment trends for each fusion level by dysphagia outcome. Separate univariable followed by multivariable logistic regression analyses were performed to evaluate predictors of dysphagia.
Results
A total of 1,212,475 ACDFs were identified in which 3.3% experienced postoperative dysphagia. A significant increase in annual dysphagia rates was observed from 2004–2014. Frailty, intraoperative neuromonitoring, 4 or more level fusions, African American race, fluid/electrolyte disorders, blood loss, and coagulopathy were all identified as significant independent risk factors for the development of postoperative dysphagia following ACDF.
Conclusion
Postoperative dysphagia is a well-known postsurgical complication associated with ACDF. Our cohort showed a significant increase in the annual dysphagia rates independent of levels fused. We identified several risk factors associated with the development of postoperative dysphagia after ACDF.
Anterior cervical discectomy and fusion (ACDF) is the most common performed surgery in the cervical spine. First described by Robertson and Smith in 1958, it now accounts for over 80% of cervical spine surgeries in the United States [1-4]. Dysphagia, typically secondary to static retraction of the longus colli muscles, esophagus, and trachea, is one of the most common complications following ACDF. Postoperative dysphagia is often a result of soft tissue edema however other reported causes include laceration of the esophagus, local ischemia due to increased intraesophageal pressure, denervation of the pharyngeal plexus via malposition of retractors, or superior laryngeal nerve/recurrent laryngeal nerve stretch injuries [5,6]. Some studies have proposed certain demographic and perioperative risk factors associated with increased dysphagia rates. These include female sex, older age, more comorbidities, increased operative time, use of plating, excessive or prolonged retraction, elevated endotracheal tube cuff pressures, excessive blood loss, increased number of and more cranially oriented operative levels, revision surgery, and prevertebral soft tissue swelling. However, no clear consensus exists regarding the evaluation and prevention of dysphagia following ACDF [5-9]. Thus, we report one of the largest studies to date evaluating current trends and factors associated with the development of inpatient postoperative dysphagia after ACDF.
The National Inpatient sample (NIS) is the largest publicly available, all-payer, inpatient health care database in the United States (US) and is developed by the Healthcare Cost and Utilization Project (HCUP). The database contains a random subsample of 20% of US inpatient hospital records that represent an estimated 35 million annual discharges. The Elixhauser readmission and mortality indices are validated scoring systems that identify variables in the NIS correlated with overall patient health, mortality risk, and 30-day readmission risk [10,11].
The NIS was evaluated from 2004 to 2014 and discharges with International Classification of Diseases (ICD-9-CM) procedure codes indicating ACDF were identified (ICD-9-CM 80.51,81.02, 81.62, and 81.63). Postoperative dysphagia was identified using the ICD-9-CM code 787.2. This diagnosis is recognized by the treating physician. Parameters including age, sex, frailty, obesity, weekend admission status, patient income, race, Elixhauser mortality/readmission indices, intraoperative monitoring (IOM), and number of fused levels were obtained and analyzed. Frailty, as defined in previous works, refers to patients with inpatient hypoalbuminemia and muscle weakness/fatigue [12].
Aggregate national estimates of yearly discharge frequencies were calculated utilizing weighted observations supplied by HCUP. For the years 2004–2011 and 2012–2014, adjusted and normal weights were utilized, respectively, to adjust for temporal database changes. Statistical analysis was performed with SAS 9.4 (SAS Institute Inc., Cary, NC, USA) utilizing procedures that account for NIS stratified-cluster sampling methodology.
The normality of continuous variables was assessed graphically and statistically. Continuous variables with yearly nonparametric distributions were represented as yearly weighted median estimates; whereas, those with yearly normal distributions were represented as yearly weighted mean estimates. Comparisons of means/distributions of normally continuous variables were carried out using least squared means analysis; while, nonparametric distributions were compared with a modern extension of the Wilcoxon rank-sum test that adjusts for clustering, stratification, and weights [13]. Categorical variables were presented as an estimated weighted frequency and percent. Statistical analyses of categorical variables were carried out using chi-square and Fisher exact with the Monte Carlo simulation tests, as appropriate [14].
Time trend series plots were created for yearly treatment trends for each fusion level by dysphagia outcome. To yield a quantitative measurement of yearly distribution trends, yearly means/medians of continuous variables were assessed with univariable logistic regression, with year assessed as a continuous variable. Multivariable logistic regression was performed to evaluate predictors of dysphagia. All available hospital and discharge data were utilized as covariates. Covariates that met a significance level of p < 0.2 in the univariable model were included in the multivariable analysis. A backwards multivariable logistic regression was performed and only variables that met significance were included in the final model. Values of p ≤ 0.05 were considered statistically significant.
A total of 1,212,475 ACDF cases were identified between 2004 and 2014, of which 3.3% (n = 40,028) experienced postoperative dysphagia (Table 1). When compared to those without dysphagia, these patients tende d to be older (58.2 years vs. 52.3 years, p < 0.0001) with higher rates of frailty (1.5% vs. 0.6%) and obesity (11.5% vs. 9.2%), and were more likely to be admitted on the weekend (2.8% vs. 1.6%). They also had higher Elixhauser readmission (4.2 vs. -0.2, p < 0.0001) and mortality indices (-0.7 vs. -0.8, p < 0.0001). With regards to race, African Americans, (13.9% vs. 8.8%), Hispanics (6.3% vs. 5.1%) and Asians (1.5% vs. 1.2%) had higher rates of postoperative dysphagia. Interestingly, patients who developed postoperative dysphagia were also more likely to have had intraoperative neuromonitoring (12.7% vs. 7.1%, p < 0.0001) and dysphagia was also less likely to occur in females (49.4% vs. 52.7%, p < 0.0001). Patient income was not associated with the development of dysphagia after ACDF.
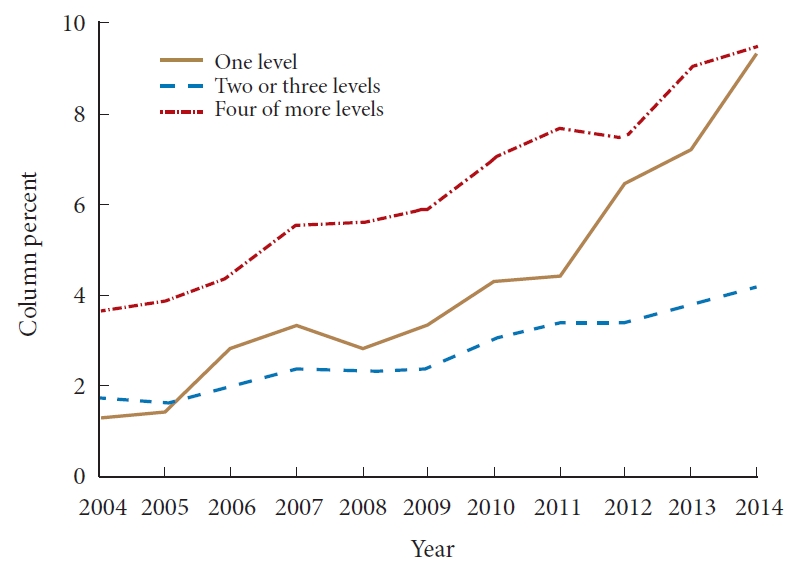
A significant increase in annual dysphagia rates (Table 2) was observed from 2004–2014 (Fig. 1; 1.9% in 2004 vs. 5.1% in 2014, odds ratio [OR] = 1.11) (p < 0.0001). Patients were also evaluated according to the number of levels fused (Table 2) with 31,879 patients undergoing a 1-level fusion, 1,013,712 patients undergoing a 2- or 3-level fusion, and 166,884 patients undergoing a 4 or more level fusion. The overall incidence of dysphagia in each of these cohorts was 3.4%, 2.8%, and 6.6%, respectively. The incidence of dysphagia also increased yearly across all cohorts. Although the 4 or more level fusion group had the highest annual and overall rates of postoperative dysphagia, by 2014 the single-level fusion group exhibited comparable rates (9.5% and 9.3%, respectively). Furthermore, the single-level fusion group also had the highest yearly likelihood of developing postoperative dysphagia during hospitalization (OR, 1.21; 95% confidence interval [CI], 1.16–1.27; p < 0.0001).
The full multivariable logistic regression analysis with CIs and p-values can be seen in Table 3. Frailty, intraoperative neuromonitoring, 4 or more level fusions, African American race, fluid/electrolyte disorders, blood loss, and coagulopathy were all identified as significant independent risk factors (OR> 1.5) for the development of postoperative dysphagia following ACDF.
The incidence of dysphagia after ACDF in this study was 3.3%, which appears to be consistent with several other large database studies [9,15,16]. However, the reported incidence in the literature varies widely due to a lack of unifying criteria and variations in study design [7]. In a systematic review of mainly prospective cohort studies, Riley et al. [8] reported dysphagia rates ranging from 1%–79% within the first week (mean, 33%), decreasing to 13%–21% (mean, 16.8%) 1 year after surgery. A single-surgeon study conducted by Nanda et al. [17], analyzed 1,576 patients from 1995 to 2012, and found a 3.3% (n = 52) dysphagia rate. On the other hand, and contrary to the trends found in the literature, a retrospective single-surgeon study of 1,123 consecutive cases by Mullins et al. [18] reported significantly lower rates, with only 0.62% of patients developing dysphagia.
Interestingly, our cohort showed a significant increase in annual dysphagia rates from 2004–2014 (Fig. 1; 1.9% in 2004 vs. 5.1% in 2014; OR, 1.11) (p < 0.0001). The incidence increased yearly independent of levels fused. The increase in the incidence of dysphagia may be the result of multiple factors. As more literature becomes available in respect to the development of postoperative dysphagia after ACDF, treating physicians may be more conscious in trying to identify and report this complication. Also, the use and implementation of electronic records may have facilitated the recording of dysphagia for administrative reasons, although there is no clear scientific evidence supporting this argument. In addition, several studies have identified that NIS studies may underreport postoperative complications [19]. Furthermore, the comorbidity burden in ACDF procedures has increased over time [1]. Another potential concerning explanation for this finding could be that previous data associating single-level ACDF with relatively low rates of postoperative dysphagia may have led to a decreased in a detailed dissection prior to retractor placement during these cases. Unfortunately, an important limitation of the NIS is the lack of readmission and long-term follow-up data, which hinders our ability to accurately assess long-term dysphagia rates.
Several studies have described a higher incidence of dysphagia among women [20-23]. In contrast, the data from our report shows dysphagia was less frequent in the global female population, a result comparable to the retrospective analysis by Riley et al. [24] and the NIS database review by Singh et al. [9]. Additionally, previous data suggested age as an independent risk factor for postoperative dysphagia [7,9,15,23,25,26]. Our results appear to be congruent with these previous studies, with a 5.9-year age increase seen in the dysphagia group. However, there is conflicting evidence as some studies found no significant association between age and the occurrence of dysphagia [20-22,24]. Few studies have evaluated the relationship between race and dysphagia. While Smith-Hammond et al. [25] reported no association, Singh et al. [9] identified African American race and Asian American race as independent risk factors. The majority of the patients in our sample were Caucasian (81.9%), and using it as a reference, we found that African American, Hispanic, and Asian races had a higher likelihood of developing dysphagia.
The comorbidity burden in ACDF procedures has increased over time [1]. The following comorbidities were identified as independent risk factors for the development of dysphagia by our study and many others: smoking [26,27], fluid and electrolyte disorders [9,16], paralysis [9,16], coagulopathy, neurodegenerative diseases [9], alcohol abuse [9,16], diabetes with chronic complications [28], depression and psychosis [9,16,28]. In contrast to some studies regarding obesity [6,27,29], our results showed that body mass index was significantly associated with dysphagia. Similarly, Wang et al. [26] and Liu et al. [30] found increased rates in the immediate postoperative period only. The authors have suggested the association between obesity and early-dysphagia may be linked to the increased thickness of the prevertebral tissue in obese patients, leading to difficulty in manipulation and excessive esophageal retraction [26,30,31]. Finally, while no past study has elucidated the implication of frailty in the development of dysphagia, the present publication demonstrated a significant association. Frailty which is defined as hypoalbuminemia, muscle weakness or fatigue may make patients especially susceptible to more intraoperative tissue manipulation and thus at increased risk of postoperative dysphagia.
There is conflicting evidence regarding the mortality and complication rates between teaching and nonteaching hospitals. According to the HCUP website, teaching status is assigned if the hospital has one or more Accreditation Council for Graduate Medical Education approved residency programs, is a member of the Council of Teaching Hospitals or has a ratio of full-time equivalent interns and residents to beds of 0.25 or higher [32]. Results from the present study suggest dysphagia was significantly more present in patients treated at academic centers (55.7% vs. 51.4%, p < 0.0003). However, there are limitations to using the NIS database for this purpose because it does not contain information regarding readmissions or dysphagia screening practices. Furthermore, it is difficult to distinguish if the increased complication rates are due to greater average length of stay as teaching facilities often deal with more complex cases and may not represent the population as a whole. Fineberg et al. [33] used the NIS to analyze 211,624 cervical procedures observing that patients treated in academic centers had longer hospitalizations (1.8 days vs. 1.6 days, p < 0.0005), increased mortality (0.06% difference, p < 0.002), and postoperative complications (2.4% vs. 1.7%, p < 0.0005), compared to patients treated in nonteaching institutions. Contrary to our results, Starmer et al. [15] conducted an analysis of 1,649,871 patients from 2001 to 2010 using the NIS and found no statistical significant difference regarding teaching status and dysphagia rates. Resident involvement may also prolong operation time thus potentially increasing time-related co mplications which may explain why we found that dysphagia was more often seen in academic centers in our data [34]. This is in line with the work of Nandyala et al. [35] who determined the impact of the influx of new interns and residents during the month of July using the NIS (n = 52,499) and found a significantly increased incidence of dysphagia (38.3 vs. 27.0 per 1,000, p = 0.006) and longer hospitalizations in the teaching hospital cohort. Conversely, Stienen et al. [34] in a single-center retrospective study determined that outcomes and complication rates from supervised neurosurgical residents with a structured training program were no different to senior surgeons. This difference may be due to the limited number of patients (n = 287), and the single-center nature of the study. Unfortunately, we cannot assess the involvement of the residents or fellows in a case-by-case scenario by NIS teaching status [35].
Among several surgeon-related risk factors, the use of recombinant human bone morphogenetic protein-2 (rhBMP-2) which is a bone graft enhancer that may be used “off label” in ACDF has been studied in relation with dysphagia. A systematic review conducted by Stark et al. [36] reported that rhBMP-2 had the highest fusion rate (100%) compared with other substitutes. However, dysphagia was significantly higher in studies using rhBMP-2 (p < 0.001). Unfortunately, the NIS database does not provide information about use of rhBMP-2 to confirm this result.
There is a tendency for patients who underwent multiple level surgery to complain about postoperative swallowing difficulty [8,20,21,24]. Similarly to previous works [37,38], our findings support the association between ≥ 4-level ACDF and postoperative dysphagia compared to the single- and 2 to 3 level groups. In contrast, Smith-Hammond et al. [25], Chin et al. [39], and Vaidya et al. [40] found no significant difference between dysphagia rates and the number of cervical levels operated. Typically, multilevel ACDF requires a wider exposure and longer operative times, which could lead to prolonged retraction of the esophagus and more prevertebral soft tissue injury [41,42]. Although the evidence is conflicting [23,26], the amount of blood loss during surgery could reflect the complexity and length of the procedure [43]. Wang et al. [26] identified blood loss as a risk factor for dysphagia immediately after surgery (151.6 mL vs. 121.6 mL, p < 0.001). However, Zeng et al. [23] failed to find a statistically significant association. Similarly, operative time was found to be a significant risk factor by some studies [7,24,26,30,44], but other studies failed to identify it as one [23,25,28]. We found blood loss was associated with dysphagia (OR, 2.21; 95% CI, 1.41–3.48; p < 0.0006), although, as mentioned previously, this is likely due to confounding variables such as longer surgical time and more complex procedures.
Interestingly, the present study is the first to our knowledge to show that by 2014, single-level ACDF dysphagia rates were comparable to those involving 4 or more levels (9.3% and 9.5%, respectively). Also, single-level ACDF showed the highest yearly likelihood of developing postoperative dysphagia during hospitalization (OR, 1.21; p < 0.0001). These numbers go against the known trend of higher incidence of dysphagia as the number of fused levels increase. One potential concerning explanation for this finding could be that previous data associating single-level ACDF with relatively lower rates of postoperative dysphagia [37] may have led to a decreased quality of dissection and soft tissue mobilization prior to retractor placement during these cases. Conversely, data suggesting high rates of dysphagia in multilevel ACDF, may lead to surgeons being more careful during dissection and soft tissue mobilization prior to retractor placement, as well as increased consciousness about deep retraction time.
Although dysphagia may be secondary to injury of the superior laryngeal, recurrent laryngeal, hypoglossal, or glossopharyngeal nerves, the efficacy and optimal modality of IOM in anterior cervical surgery remains unclear. Thirumala et al. [44] and Ajiboye et al. [45] failed to show evidence in support of IOM. Limitations in these meta-analyses include heterogeneity in the included studies, variability in the IOM modalities, and lack of standardization in IOM alert criteria [45]. In contrast to the published literature, this study noticed an increase in the rate of dysphagia in cases that used IOM (12.7% vs. 7.1%, p ≤ 0.0001). However, the use of IOM may be indicative of more complex cases with cervical deformity, severe neural element compression or the presence of myelopathy, which may result in increased operative time, blood loss and multilevel procedures; thus, confounding is likely to be present.
With the present findings, preventive measures and proper patient orientation should take precedent. Decreasing the endotracheal tube cuff pressure to 20 mmHg during retractor placement may be helpful, although it has not been consistently shown to reduce dysphagia [46]. Strategies such as intraoperative retropharyngeal steroids, preoperative tracheal retraction exercise, and the use of a posterior approach to the cervical spine in patients at higher risk of developing postoperative dysphagia should be considered as an attempt to diminish this postoperative complication. As mentioned previously, dysphagia rates following ACDFs have continued to increase over time and this phenomenon is likely multifactorial in nature. Future studies evaluating the variables contributing to this trend will help aid our understanding of this unwanted postoperative complication and may allow us to reduce it.
There are several limitations in our study, including the lack of long-term follow-up information. The NIS database provides no information about specific levels treated, readmission rates, previous procedures, medical management, and outpatient procedures. Another limitation is the lack of information about the type of hardware used in the procedures. Furthermore, with any sample size as large as the one in this study, statistically significant differences may be identified but remain difficult to interpret clinically especially if their OR remains close to 1. Although our data includes a large population representative of the entire US population, this study was limited to the evaluation of factors contributing to postoperative dysphagia and future studies are necessary to determine why we observed increasing rates of dysphagia over time.
Postoperative dysphagia is a well-known postsurgical complication associated with ACDF. This study reviews and identifies several associated risk factors for the occurrence of postoperative dysphagia after ACDF in the US using the National Inpatient Sample. Our cohort showed a significant increase in the annual dysphagia rates independent of levels fused.
Table 1.
Patient and procedural characteristics for ACDF stratified by dysphagia
Table 2.
Yearly incidence of post-ACDF dysphagia by fusion levels
Table 3.
Multivariable predictors of dysphagia following ACDF
| Effect | OR | 95% CL | p-value |
|---|---|---|---|
| Age | 1.03 | 1.02, 1.03 | < 0.001 |
| Obesity | 1.12 | 1.03, 1.22 | 0.0071 |
| Frailty | 1.75† | 1.41, 2.17 | < 0.001 |
| Female | 0.87 | 0.83, 0.92 | < 0.001 |
| Race (Ref = White) | |||
| African American | 1.52† | 1.4, 1.66 | < 0.001 |
| Hispanic | 1.29† | 1.14, 1.47 | < 0.001 |
| Asian or Pacific Islander | 1.27† | 1.05, 1.55 | 0.0162 |
| Native American | 0.85 | 0.56, 1.3 | 0.4466 |
| Other | 1.03 | 0.86, 1.24 | 0.7564 |
| Academic hospital | 1.15 | 1.05, 1.27 | 0.0035 |
| Intraoperative monitoring | 1.61† | 1.44, 1.79 | < 0.001 |
| No. of levels fused (Ref = One) | |||
| Two or 3 levels | 0.91 | 0.74, 1.11 | 0.3477 |
| Four levels or more levels | 1.75† | 1.41, 2.16 | < 0.001 |
| Psychoses | 1.32† | 1.14, 1.52 | 0.0002 |
| Neurodegenerative diseases | 1.47† | 1.32, 1.63 | < 0.001 |
| Fluid and electrolyte disorders | 2.87† | 2.62, 3.15 | < 0.001 |
| Diabetic with complications | 1.42† | 1.21, 1.67 | < 0.001 |
| Diabetic without complications | 1.16 | 1.09, 1.24 | < 0.001 |
| Depression | 1.13 | 1.05, 1.21 | 0.0014 |
| Alcohol abuse | 1.35† | 1.14, 1.6 | 0.0005 |
| Blood loss | 2.21† | 1.41, 3.48 | 0.0006 |
| Coagulopathy | 1.59† | 1.28, 1.96 | < 0.001 |
| Paralysis | 1.84† | 1.6, 2.11 | < 0.001 |
REFERENCES
1. Marquez-Lara A, Nandyala SV, Fineberg SJ, et al. Current trends in demographics, practice, and in-hospital outcomes in cervical spine surgery: a national database analysis between 2002 and 2011. Spine (Phila Pa 1976) 2014 39:476-81.

2. Robinson RA, Smith GW. Anterolateral disc removal and interbody fusion for cervical disc syndrome. Bull Johns Hopkins Hosp 1955 96:223-4.
3. SMITH GW, ROBINSON RA. The treatment of certain cervical-spine disorders by anterior removal of the intervertebral disc and interbody fusion. J Bone Joint Surg Am 1958 40-A:607-24.


4. Cheung KM, Mak KC, Luk KD. Anterior approach to cervical spine. Spine (Phila Pa 1976) 2012 37:E297-302.


5. Kepler CK, Rihn JA, Bennett JD, et al. Dysphagia and soft-tissue swelling after anterior cervical surgery: a radiographic analysis. Spine J 2012 12:639-44.


6. Anderson KK, Arnold PM. Oropharyngeal dysphagia after anterior cervical spine surgery: a review. Global Spine J 2013 3:273-86.



7. Kalb S, Reis MT, Cowperthwaite MC, et al. Dysphagia after anterior cervical spine surgery: incidence and risk factors. World Neurosurg 2012 77:183-7.


8. Riley LH 3rd, Vaccaro AR, Dettori JR, et al. Postoperative dysphagia in anterior cervical spine surgery. Spine (Phila Pa 1976) 2010 35(9 Suppl):S76-85.


9. Singh K, Marquez-Lara A, Nandyala SV, et al. Incidence and risk factors for dysphagia after anterior cervical fusion. Spine (Phila Pa 1976) 2013 38:1820-5.


10. Moore BJ, White S, Washington R, et al. Identifying increased risk of readmission and in-hospital mortality using hospital administrative data: the AHRQ Elixhauser Comorbidity Index. Med Care 2017 55:698-705.


11. Elixhauser A, Steiner C, Harris DR, et al. Comorbidity measures for use with administrative data. Med Care 1998 36:8-27.


12. Hebeler KR, Baumgarten H, Squiers JJ, et al. Albumin is predictive of 1-year mortality after transcatheter aortic valve replacement. Ann Thorac Surg 2018 106:1302-7.


13. Natarajan S, Lipsitz SR, Fitzmaurice GM, et al. An extension of the Wilcoxon Rank-Sum test for complex sample survey data. J R Stat Soc Ser C Appl Stat 2012 61:653-64.



14. Spall JC. Monte Carlo computation of the fisher information matrix in nonstandard settings. J Comput Graph Stat 2005 14:889-909.

15. Starmer HM, Riley LH 3rd, Hillel AT, et al. Dysphagia, short-term outcomes, and cost of care after anterior cervical disc surgery. Dysphagia 2014 29:68-77.


16. Joseph JR, Smith BW, Mummaneni PV, et al. Postoperative dysphagia correlates with increased morbidity, mortality, and costs in anterior cervical fusion. J Clin Neurosci 2016 31:172-5.


17. Nanda A, Sharma M, Sonig A, et al. Surgical complications of anterior cervical diskectomy and fusion for cervical degenerative disk disease: a single surgeon's experience of 1,576 patients. World Neurosurg 2014 82:1380-7.


18. Mullins J, Pojskić M, Boop FA, et al. Retrospective single-surgeon study of 1123 consecutive cases of anterior cervical discectomy and fusion: a comparison of clinical outcome parameters, complication rates, and costs between outpatient and inpatient surgery groups, with a literature review. J Neurosurg Spine 2018 28:630-41.


19. Poorman GW, Passias PG, Buckland AJ, et al. Comparative analysis of perioperative outcomes using nationally derived hospital discharge data relative to a prospective multicenter surgical database of adult spinal deformity surgery. Spine (Phila Pa 1976) 2017 42:1165-71.


20. Lee MJ, Bazaz R, Furey CG, et al. Risk factors for dysphagia after anterior cervical spine surgery: a two-year prospective cohort study. Spine J 2007 7:141-7.


21. Bazaz R, Lee MJ, Yoo JU. Incidence of dysphagia after anterior cervical spine surgery: a prospective study. Spine (Phila Pa 1976) 2002 27:2453-8.

22. Papavero L, Heese O, Klotz-Regener V, et al. The impact of esophagus retraction on early dysphagia after anterior cervical surgery: does a correlation exist? Spine (Phila Pa 1976) 2007 32:1089-93.

23. Zeng JH, Zhong ZM, Chen JT. Early dysphagia complicating anterior cervical spine surgery: incidence and risk factors. Arch Orthop Trauma Surg 2013 133:1067-71.


24. Riley LH 3rd, Skolasky RL, Albert TJ, et al. Dysphagia after anterior cervical decompression and fusion: prevalence and risk factors from a longitudinal cohort study. Spine (Phila Pa 1976) 2005 30:2564-9.

25. Smith-Hammond CA, New KC, Pietrobon R, et al. Prospective analysis of incidence and risk factors of dysphagia in spine surgery patients: comparison of anterior cervical, posterior cervical, and lumbar procedures. Spine (Phila Pa 1976) 2004 29:1441-6.

26. Wang T, Ma L, Yang DL, et al. Factors predicting dysphagia after anterior cervical surgery: A multicenter retrospective study for 2 years of follow-up. Medicine (Baltimore) 2017 96:e7916.


27. Siska PA, Ponnappan RK, Hohl JB, et al. Dysphagia after anterior cervical spine surgery: a prospective study using the swallowing-quality of life questionnaire and analysis of patient comorbidities. Spine (Phila Pa 1976) 2011 36:1387-91.

28. Kang SS, Lee JS, Shin JK, et al. The association between psychiatric factors and the development of chronic dysphagia after anterior cervical spine surgery. Eur Spine J 2014 23:1694-8.


29. Rihn JA, Kane J, Albert TJ, et al. What is the incidence and severity of dysphagia after anterior cervical surgery? Clin Orthop Relat Res 2011 469:658-65.


30. Liu JM, Tong WL, Chen XY, et al. The incidences and risk factors related to early dysphagia after anterior cervical spine surgery: a prospective study. PLoS One 2017 12:e0173364.



31. Perez-Roman RJ, McCarthy D, Luther EM, et al. Effects of body mass index on peri-operative outcomes in patients undergoing anterior cervical discectomy and fusion surgery. Neurospine 2020 Nov 17 [Epub]. https://doi.org/10.14245/ns.2040236.118.

32. Agency for Healthcare Research and Quality. HCUP NIS description of data elements. Rockville (MD), Agency for Healthcare Research and Quality. 2008 [cited 2020 May 3]. Available from: www.hcup-us.ahrq.gov/db/vars/hosp_teach/nisnote.jsp.
33. Fineberg SJ, Oglesby M, Patel AA, et al. Outcomes of cervical spine surgery in teaching and non-teaching hospitals. Spine (Phila Pa 1976) 2013 38:1089-96.


34. Stienen MN, Joswig H, Jucker D, et al. Anterior cervical discectomy and fusion: is surgical education safe? Acta Neurochir (Wien) 2015 157:1395-404.


35. Nandyala SV, Marquez-Lara A, Fineberg SJ, et al. Perioperative characteristics and outcomes of patients undergoing anterior cervical fusion in July: analysis of the “July effect”. Spine (Phila Pa 1976) 2014 39:612-7.

36. Stark JR, Hsieh J, Waller D. Bone graft substitutes in single- or double-level anterior cervical discectomy and fusion: a systematic review. Spine (Phila Pa 1976) 2019 44:E618-28.

37. De la Garza-Ramos R, Xu R, Ramhmdani S, et al. Long-term clinical outcomes following 3- and 4-level anterior cervical discectomy and fusion. J Neurosurg Spine 2016 24:885-91.


38. Danto J, DiCapua J, Nardi D, et al. Multiple cervical levels: increased risk of dysphagia and dysphonia during anterior cervical discectomy. J Neurosurg Anesthesiol 2012 24:350-5.

39. Chin KR, Eiszner JR, Adams SB Jr. Role of plate thickness as a cause of dysphagia after anterior cervical fusion. Spine (Phila Pa 1976) 2007 32:2585-90.

40. Vaidya R, Carp J, Sethi A, et al. Complications of anterior cervical discectomy and fusion using recombinant human bone morphogenetic protein-2. Eur Spine J 2007 16:1257-65.



41. Kang SH, Kim DK, Seo KM, et al. Multi-level spinal fusion and postoperative prevertebral thickness increase the risk of dysphagia after anterior cervical spine surgery. J Clin Neurosci 2011 18:1369-73.


42. Zhou J, Li J, Lin H, et al. A comparison of a self-locking standalone cage and anterior cervical plate for ACDF: Minimum 3-year assessment of radiographic and clinical outcomes. Clin Neurol Neurosurg 2018 170:73-8.


43. Fehlings MG, Smith JS, Kopjar B, et al. Perioperative and delayed complications associated with the surgical treatment of cervical spondylotic myelopathy based on 302 patients from the AOSpine North America Cervical Spondylotic Myelopathy Study. J Neurosurg Spine 2012 16:425-32.


44. Thirumala PD, Muralidharan A, Loke YK, et al. Value of intraoperative neurophysiological monitoring to reduce neurological complications in patients undergoing anterior cervical spine procedures for cervical spondylotic myelopathy. J Clin Neurosci 2016 25:27-35.



- TOOLS
- Related articles in NS
-
Journal Impact Factor 3.2