 |
 |
- Search
|
|
||
Abstract
Objective
The purpose of this study is to characterize the learning curve of endoscopic lumbar decompression based on peri- and postoperative parameters and to suggest the potential of full endoscopic decompression as a primary treatment option for lumbar canal and lateral recess stenosis.
Methods
The records of 223 consecutive patients who underwent percutaneous endoscopic decompression by a single surgeon for their lumbar canal and lateral recess stenosis were reviewed. Patients were stratified into group 1 (n=100) and group 2 (n=123), depending on their case number. After the 100th case, the procedural time reached a plateau and subsequent patients were assigned to the second group. Demographics and surgical outcomes, including operative times, change in dural sac dimensions, length of hospital stay, and intraoperative complication rates were compared between the 2 groups. Postoperative clinical outcomes, including the visual analogue scale (VAS), the Oswestry Disability Index (ODI) and reoperation rates were compared between the 2 groups (group 1, n=90; group 2, n=110) by follow-up evaluation.
Results
Procedural times were greater in group 1 than group 2 (group 1, 105.26 minutes; group 2, 67.65 minutes; p<0.05) and they had higher complication rates (group 1, 16% [16 of 100]; group 2, 8.3% [8 of 123]; p<0.05). The length of hospitalization, postoperative improvement in VAS and ODI, and reoperation rates were not different between the groups. In both groups, stenotic spinal canals were effectively decompressed.
Conclusion
Continued surgical experience was associated with a reduction in operative times and less intraoperative complications. Although the learning curve was steep and additional surgical experience may be needed to overcome the learning curve, percutaneous full endoscopic lumbar decompression is a safe, clinically-feasible, and effective surgical technique and can be adopted as the primary treatment for lumbar canal and lateral recess stenosis.
Endoscopic spine surgery in lumbar disease has continuously evolved over the past three decades since several pioneers introduced it to traditional spine surgeons [1-3]. Endoscopic surgery has many advantages over traditional open surgery, including less iatrogenic injury and postoperative back pain, and earlier return to a normal life. The efficacy and safety of endoscopic spine surgery has also been demonstrated by several studies [4-8]. The development of endoscopic spinal surgical techniques and the advancement of endoscopic instruments have broadened the utilization of surgical endoscopic spine surgery to applications ranging from simple disc herniation to more complicated cases, such as highly migrated disc herniation, and other pathologies combined with bony degeneration to produce foraminal and canal stenosis [9-13]. Nowadays, degenerative lumbar stenosis in the spinal canal and lateral recess can be treated with full-endoscopic surgery using various accesses and techniques and several authors have reported their successful outcomes [8,14-17].
However, endoscopic spine surgery is usually associated with a steep learning curve and high complication rates, and much time and experience are needed before surgeons become familiar with the technique [18-21]. Such complexity of the operation and concerns by the surgeon regarding the safety of endoscopic spine surgery have presented barriers to its adoption as the primary technique for treatment of lumbar spinal canal and lateral recess stenosis. No comprehensive study has evaluated operative times, perioperative complications, or outcomes associated with gaining experience with the percutaneous endoscopic decompression technique in cases of lumbar canal and lateral recess stenosis. The results of such studies could provide valuable information to spine surgeons who begin to perform this operation and help them to avoid severe complications in the early stages of the learning curve.
The purpose of this study was to discuss the safety and practical feasibility of endoscopic lumbar decompression by characterizing a single surgeon’s learning curve based on perioperative and postoperative parameters and to suggest the potential of the full endoscopic decompression technique as a primary treatment option for lumbar canal and lateral recess stenosis. Additionally, surgical strategies and technical tips necessary to overcome the learning curve are discussed.
The study inclusion criteria were preoperatively diagnosed lumbar central canal or lateral recess stenosis with symptoms of neurogenic intermittent claudication and radiculopathy that were refractory to conservative treatment for a period of at least three months. Patients with documented diagnoses of segmental instability, degenerative spondylolisthesis greater than Meyerding grade I, scoliosis of more than 20 degrees, combined foraminal stenosis in the same or lower level, or coexisting pathologic conditions, such as acute inflammation, infection, or the known presence of tumors were excluded.
Total 223 consecutive patients who underwent a percutaneous endoscopic lumbar decompression (with or without discectomy) by a single surgeon for degenerative lumbar canal and lateral recess stenosis between November 2013 and February 2018 were retrospectively reviewed. The case number at which the procedural time plateaued along a distribution graph was used to represent the learning curve, which in this scenario was after the 100th patient in our series. Thus, based on the date of surgery, we divided the cases into 2 groups: 100 cases in group 1 (from November 2013 to April 2017) and 123 cases in group 2 (from April 2017 to February 2018) (Fig. 1). The initial 100 patients who underwent surgery were compared with the second 123 patients in regard to demographics and perioperative parameters, such as operative times and length of hospital stays. Data was collected on previously reported perioperative complications, including dural tears, neural damage (postoperative dysthesia and motor weakness), excessive resection or fracture of the facet joint, postsurgical hematomas, and surgical site infections, and were compared between the 2 groups. To evaluate the degree of decompression radiologically, the cross-sectional area of the dural sac was examined and compared pre- and postoperatively by axial magnetic resonance imaging (MRI) images at the middisc level, and also compared between the 2 groups. Radiologic measurements were done using automated and digitalized tools in the PACS system, PiView 1.0 (Infinitt Co. Ltd., Seoul, Korea).
Postoperative outcome evaluation by visual analogue scale (VAS) and Oswestry Disability Index (ODI) was conducted three months after surgery and on the day of final follow-up. The changes in VAS and ODI after the operation were compared between the 2 groups. Any second spinal surgeries at the index level occurring during the follow-up period were designated as “reoperations.” The incidence, indications, and type of second surgery were compared between the groups. Statistical calculations, including means and standard deviations, were obtained using SPSS ver. 17.0 (SPSS Inc., Chicago, IL, USA). Pearson correlation coefficient was used to characterize the relationship between the case numbers and the perioperative outcome measures. The independent t-test and paired t-tests were used to compare the differences in each parameter between the 2 groups. Statistical significance was established at a p-value of less than 0.05.
This study was approved by the local Institutional Review Board of the Leon Wiltse Memorial Hospital (approval number: 2019-W02) and informed consent was obtained from all individual participants included in the study.
The operations were all performed under general or epidural anesthesia with sedation, with the patient in a prone position, as reported by previous authors [15]. The operation was performed bilaterally via a unilateral access approach as in conventional microscopic bilateral lumbar decompression with a unilateral approach. After making a paramedian skin incision approximately 9 mm long (target point: the caudal margin of the upper lamina), blunt insertion of a serial dilator toward the target point was performed. This was followed by insertion of the operating sheath over the dilator with the beveled opening facing medially toward the ligamentum flavum. The procedure was performed under direct endoscopic visual control and with constant irrigation. Depending on the pathology, the first ipsilateral decompression, including a cranial and caudal laminotomy and partial facetectomy, was performed with a drill and punch. The contralateral side was entered dorsally to the dura. The ligamentum flavum was initially left intact as much as possible to protect the dura, and contralateral bony decompression was performed, again using a cranial and caudal laminotomy and partial facetectomy. Subsequently, the ligamentum flavum was removed in en bloc fashion in most cases. The decompression concluded when the dura and spinal nerves were seen to be clearly decompressed on both sides (Fig. 2A-C). The removal of any disc herniation seen to indent, compress, or displace the thecal sac or nerve root, and intradiscal nucleotomy were performed on a case-by-case basis, as needed. Drainage was applied postoperatively and removed one day after the surgery.
Patient demographics and procedure types are described in Table 1. Group 1 had a higher proportion of male patients than group 2. Patient ages were similar between the groups. Group 2 was more likely to undergo the procedure at 2 levels (p<0.05), and lumbar decompression was less likely at 1 level (p<0.05), than in group 1. No differences were seen in the case numbers, the type of surgery (unilateral vs. bilateral, combined discectomy), or severity of the pathology (the degree of stenosis) between the groups.
The mean operative time was 84.51±31 minutes for 1 level. Pearson correlation coefficient demonstrated that the case number was associated with decreased surgical times (r=-0.65, p<0.001) (Fig. 3A) and that there was no significant association between case number and length of hospital stay (r=-0.06, p=0.398) (Fig. 3B). The case number at which the procedural time plateaued along a distribution graph was used to represent the learning curve, which in this scenario occurred after the 100th patient in our series. Comparative analyses between groups 1 and 2 showed that procedural times (105.26±30.49 minutes vs. 67.65±18.83 minutes, respectively, p<0.05) and perioperative complication rates (16 of 100 [16%] vs. 8 of 123 [6.5%], respectively, p<0.05) were greater in group 1 compared to group 2. No significant differences in hospital stays (5.49±6.52 days vs. 5.37±5.09 days, p=0.882) were identified between the 2 groups (Table 2).
Dural sac expansion was observed by the comparison of preand postoperative MRI axial images. The differences between pre- and postoperative spinal canal dimensions were statistically significant in both groups (group 1: preoperative 60.65±30.32, postoperative 162.54±52.38, p=0.001; group 2: preoperative 53.74±34.34, postoperative 194.89±63.84, p=0.001). Our study showed that more decompression was achieved in group 2, compared to group 1 (group 1: 101.89±42.68, group 2: 138.31±56.86, p=0.001) (Table 3).
A total of 23 patients dropped out the study (group 1: 10 patients [3 lost contact, 7 refused telephone interviews]; group 2: 13 patients [5 lost contact, 7 refused telephone interviews, and 1 died of a heart attack]). Clinical parameters for a total of 200 patients (group 1: 90 patients, group 2: 110 patients) were followed-up and evaluated (Fig. 1).
The average follow-up duration was 22.34±12.49 months (group 1: 31.82±13.20 months, group 2: 14.63±2.97 months, p>0.05). Both groups had comparable VAS and ODI scores preoperatively. At 3 months postoperatively and at the last postoperative follow-up, similar statistically significant improvements in VAS and ODI outcome scores were found in both groups (VAS back pain preoperatively, 3 months postoperatively, last postoperative follow-up: group 1, 5.96±2.65, 3.25±1.71, and 2.60±1.70 respectively; group 2, 5.91±2.30, 3.52±1.72, and 2.68±1.58, respectively; VAS leg pain preoperatively, 3 months postoperatively, last postoperative follow-up: group 1, 6.44±2.41, 3.60±1.85, and 2.67±1.60, respectively; group 2, 6.56±2.16, 3.79±1.83, and 2.86±1.63 respectively) (Fig. 4A); ODI preoperatively, 3 months postoperatively, last postoperative follow-up: group 1, 22.37±10.25, 13.98±7.83, and 10.34±7.83, respectively; group 2, 22.04±9.49, 13.37±6.53, and 9.63±6.38, respectively (Fig. 4B). The rate of reoperation at the index level did not differ between groups 1 and group 2 (5 of 90 [5.5%] and 3 of 110 [2.7%], respectively, p=0.37). In group 1, 4 cases of disc reherniation were treated by secondary percutaneous endoscopic lumbar discectomy (2 cases), and microscopic laminectomy and discectomy (2 cases), and a case of restenosis was corrected with microscopic revision surgery. In the second group, a case of dura tearing was managed by an additional microscopic laminectomy and dural repair, and 2 cases of disc reherniation were treated by microscopic revision surgery and anterior lumbar interbody fusion.
Today, percutaneous full endoscopic spinal surgery is a standard surgical technique. Previous authors have reported many surgical advantages of endoscopic spinal surgery compared to traditional spinal surgery, including less postoperative pain and faster recoveries attributed to fewer iatrogenic injuries [4-8]. Therapeutic indications for endoscopic spinal surgery have been extended beyond simple disc herniation to more complicated cases, such as highly migrated disc herniation, and other pathologies combined with bony degeneration to produce foraminal and canal stenosis [9-13]. The clinical efficacy and feasibility of endoscopic spinal surgery in lumbar spinal canal and lateral recess stenosis have been demonstrated by favorable clinical results in several studies [8,14-17]. However, the steep learning curve and high complication rates are hurdles for spine surgeon to adopt endoscopic spine surgery as the primary treatment for lumbar canal stenosis [18-21].
To construct a learning curve model for percutaneous full endoscopic lumbar laminectomies and foraminotomies with or without discectomy, our study analyzed objective perioperative (procedural times and lengths of hospital stay) and postoperative outcomes (complications and reoperations). Our findings suggest that improvements in surgical outcomes, such as operative times and complication rates following percutaneous full endoscopic laminectomies and foraminotomies, were associated with an increase in the case number. Operative times for percutaneous full endoscopic lumbar decompression were relatively long in the current study (84.51±31 minutes for 1 level), compared to operative times in previous spinal stenosis surgery, and other minimally invasive decompressive surgeries [22-26]. Although the operator was a surgeon who had abundant experience in spinal surgery, operative times reached a plateau following 100 cases and higher complication rates in the early stage of learning were observed, indicating that percutaneous full endoscopic surgery for lumbar canal decompression had a steep learning curve. However, as shown in the current study, operative times continually shortened and stabilized as the surgeon overcame the learning curve and the complication rates dropped in the late period of the learning curve. Interestingly, such a steep learning curve did not affect the postoperative clinical outcomes or the level of completion for spinal canal decompressions. The results showed favorable clinical outcomes, even in the early stages of the learning curve. The ability of the percutaneous endoscope to achieve canal decompression proved to be satisfactory on radiologic analysis of canal diameter changes in this study. There was no revision case owing to incomplete decompression in either group, which also supports the stable efficacy of endoscopic decompression, with no associated with the learning curve. These results suggest that the percutaneous full endoscopic lumbar laminectomy and foraminotomy technique has a steep learning curve, but that the procedure can be learned with time, and is relatively safe and provides credible postoperative outcomes, regardless of the operator’s skill and experience.
The learning curve is associated with more than a shortening of the operative times. It also represents more complicated components, such as understanding of the operative anatomy and procedural steps, manipulation skills, and some other factors related to the outcome of the operation. The learning curve is not only a criterion for judging whether the endoscopic surgeon has entered the stable stage of the operation in terms of the operative times and complications, but also helps the surgeon discover his or her weak and strong technical points and to gain insight into the details of the procedure [20,21,24,27]. A few issues should be considered in order to overcome the learning curve for percutaneous full endoscopic lumbar laminectomy and foraminotomy techniques.
The authors think it is a prerequisite for smooth surgeries that a surgeon should be full-equipped with specialized endoscopic instruments. The surgeon in this study first began performing percutaneous full endoscopic lumbar laminectomies and foraminotomies with primitive endoscopic instruments used for endoscopic discectomies. Performance of the procedures was paused for a period due to heavy surgical burden in the early stage of the learning curve. The introduction of endoscopic instruments, specialized for endoscopic decompression changed the situation, breaking the deadlock and restarting the surgeries and made the entire procedure easier and shortened the total operative times. Endoscopic drills with large-sized burrs, high speed and strong torque, variable-sized punches with wide and thin footprints enhanced the surgical step in which the bony structure was removed and a newly developed bipolar radiofrequency (RF) instrument was efficiently used to control the intraoperative bleeding and ablate soft tissue. The current endoscopic instruments still have several shortcomings that need to be evolved. Further development of instruments optimized for endoscopic decompressive surgery would change the learning curve more flat.
The operative view in endoscopic spinal surgery is very narrow and magnified during the procedure. Additionally, the unique optical angle (20°–25°) of endoscope can induce operator to have confusion in understanding the related anatomical structures and initial operative orientation during surgery, which can be the initial barrier to overcome in the surgical learning curve. The surgeon should not get lost during surgery by using specific structure as their surgical landmark. Ligament flavum is a useful landmark to determine the midline, upper, and lower borders of the bony decompression. The superior articular process is another landmark useful in determining the lateral margin of an ideal bony decompression (Fig. 2D-G). Such landmarks can provide anatomical orientation to the operator in the early stage of the operation, which allow the surgeon to proceed the operation with confidence and to overcome the learning curve easily.
The difference between a genuine operative angle and an endoscopic optical angle may also cause an operator to perform excessive bony work or to identify incomplete decompression in initial learning period. Drilling in lateral direction from midline with 180° rotation of the scope is helpful to preserve the facet joint as much as possible and accomplish proper decompression. Besides, a skillful rotation and tilting maneuver of the endoscope can provide the surgeon with the best operative view to explore hidden areas where are not accessible by microscope and enable the surgeon to manage dangerous surgical blind spots effectively with direct endoscopic observation.
Postoperative dysthesia, motor weakness and dural tear were typical complications reported in the current study. The general incidence of such complications was not high compared to previously reported results of other minimally invasive spinal surgeries [22,26,28-32]. Complication rates were relatively high in the early stage of the learning curve. However, complications rarely occurred after the learning curve was overcome and operative times stabilized. The major causes of intraoperative neural injury were the excessive retraction and manipulation of the neural structure without beforehand adhesiolysis. Minimal, delicate manipulation and beforehand adhesiolysis of the neural structures are essential to minimize intraoperative neural injury, and bipolar RF of adequate intensity (soft tissue ablation and bone bleeding control: 250 W, but around the neural structures: below 90 W) is mandatory to avoid postoperative dysthesia. In the current study, there were five cases of dural tears (2.2%), which was very low compared to previous studies [19,33-37]. Constant intraoperative saline irrigation through a working channel provided more safe space to differentiate the neural structures from the surrounding structures. These advantages helped the surgeon to easily confirm adequate decompression and made the entire procedure safer, which lowered the risk of dural injury during the endoscopic decompression. Beginners in endoscopic decompressive surgery should be careful to avoid complications in the early stage of the learning curve. Previous experience in traditional open and endoscopic surgery can be helpful to shorten the period needed to overcome the learning curve. Supervision by experts, indirect surgical experiences through cadaveric workshops, operative illustration videos, and observation of experts’ surgeries are recommended to lower the complications in the early period of the learning curve and to overcome the learning curve in short time.
However, this study was based on a single surgeon’s experience had relatively abundant experience with both microscopic and endoscopic spinal surgery. Therefore, the results should not be generalized to most other spine surgeons. A surgeon who has much experience in endoscopic or traditional lumbar spine surgery would need more cases to overcome the learning curve and avoid intraoperative complications.
Continued surgical experience in percutaneous full endoscopic lumbar decompression was associated with reduced operative times and less intraoperative complications. Independent of surgical experience, all patients demonstrated similar improvements in clinical outcomes, successful decompression of the stenotic canals, and lateral recesses following the surgeries. These findings suggest that, although the learning curve is steep and surgical experience may be needed to familiarize surgeons with the procedure, endoscopic lumbar decompression is a safe, clinically-feasible, and effective surgical technique which can be adopted as the primary treatment for lumbar canal and lateral recess stenosis.
Fig. 1.
Flowchart of patient inclusion, exclusion, and postoperative outcome evaluation. VAS, visual analogue scale; ODI, Oswestry Disability Index.
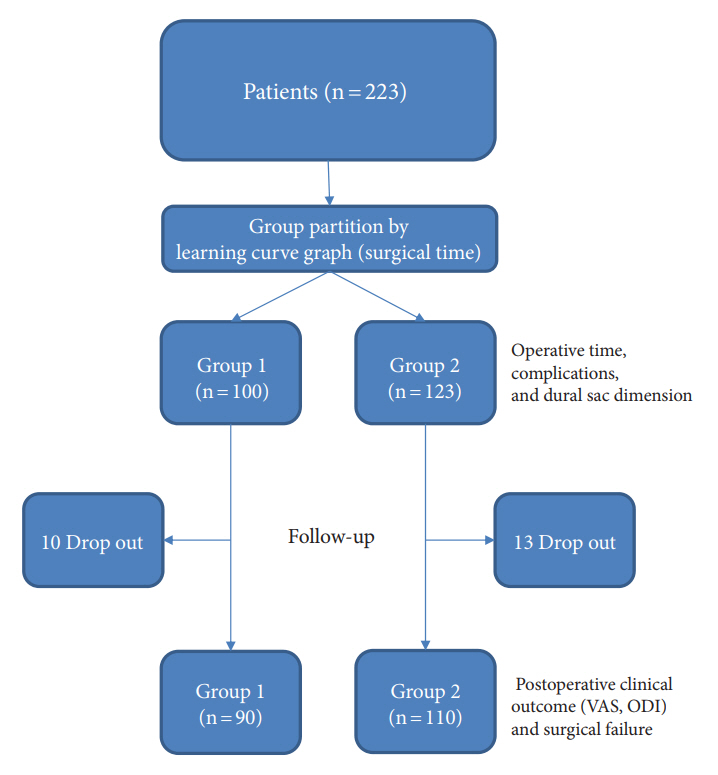
Fig. 2.
(A-C) Operative illustration of endoscopic intraoperative findings showing decompressed thecal sac, ipsilateral, and contralateral traversing root (asterisk). (D-G) Anatomical landmarks in percutaneous endoscopic lumbar canal decompression showing ligament flavum (asterisk), midline (red dotted line), medial margin of the ipsilateral superior articular process (SAP) (black dotted curved line), and medial margin of the contralateral SAP (white dotted curved line).
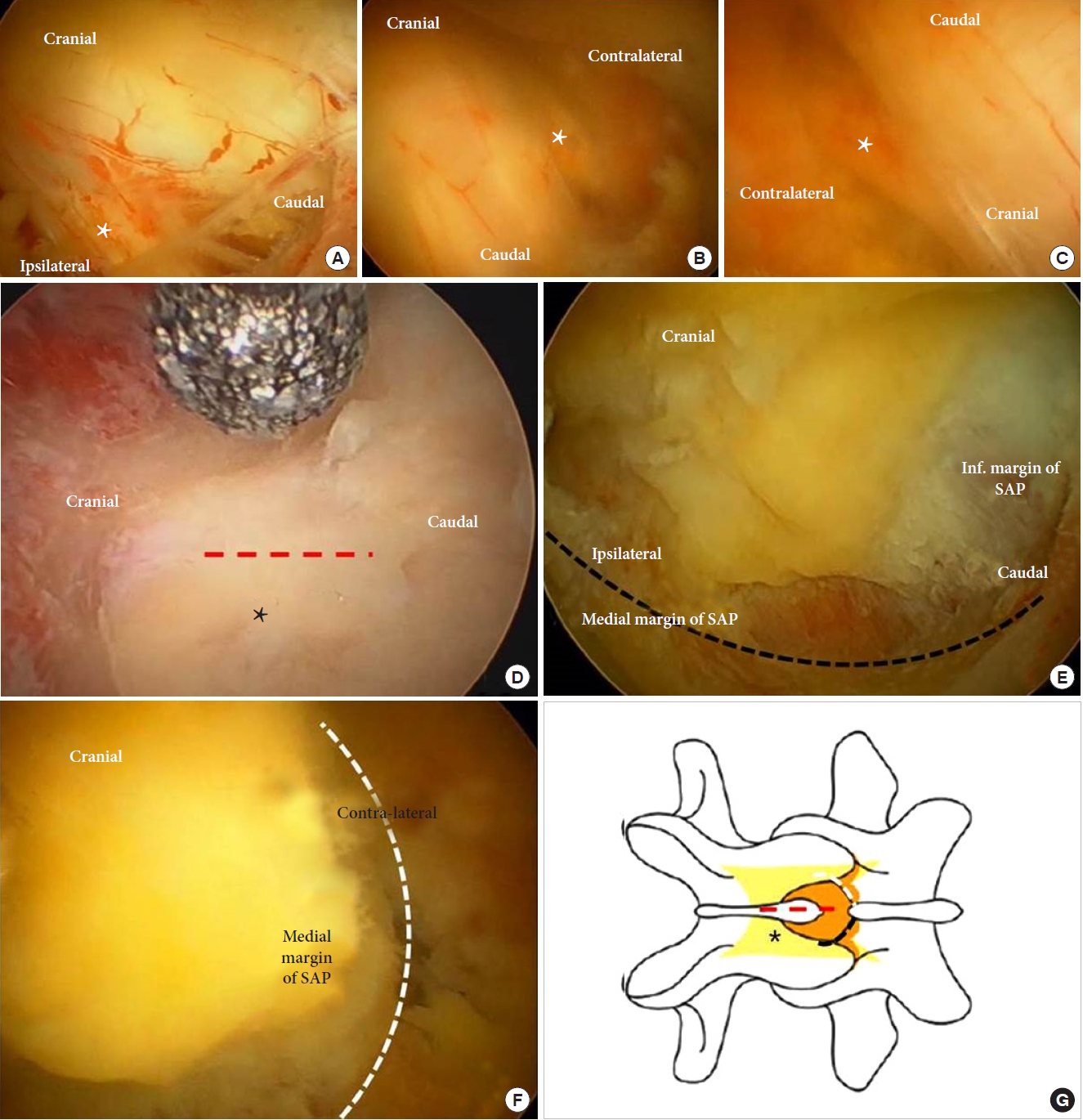
Fig. 3.
Graph of the learning curve based on operation time (A) and length of hospitalization (B) plotted against case number.
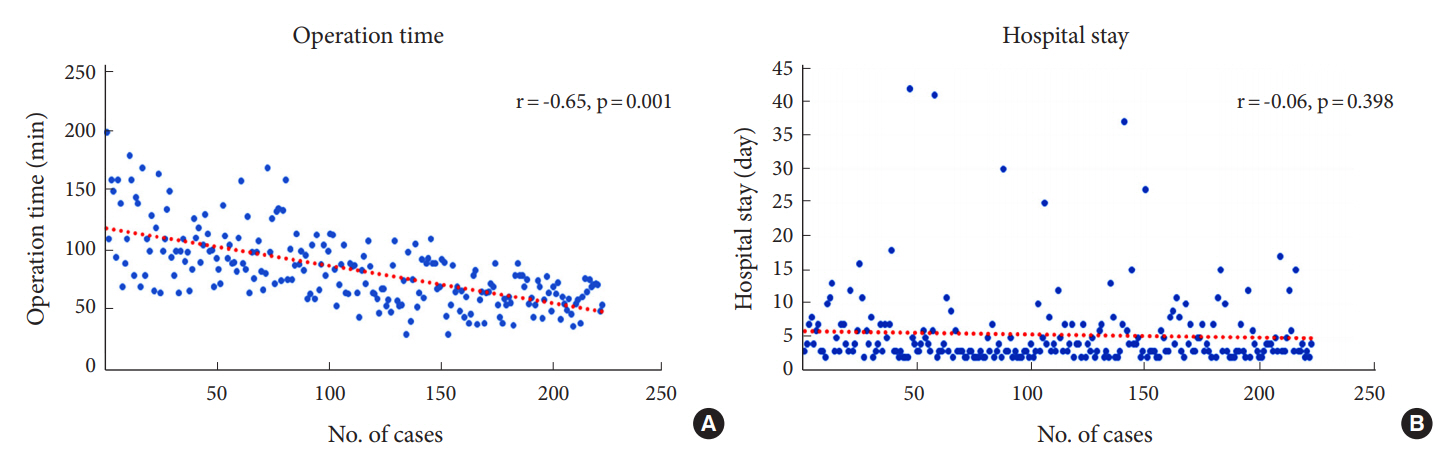
Fig. 4.
Changes in the visual analogue scale (VAS) (A) and Oswestry Disability Index (ODI) (B) improvement.
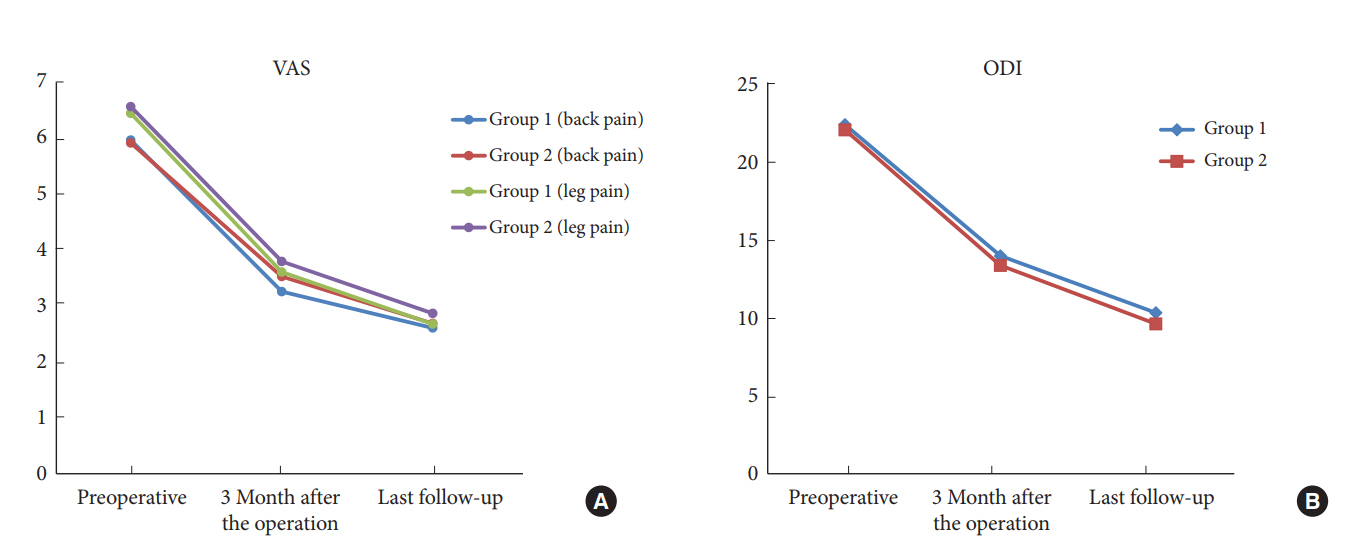
Table 1.
Patient demographics and characteristics (n=223)
| Characteristic | Group 1 (n = 100) | Group 2 (n = 123) | p-value |
|---|---|---|---|
| Age (yr) | 61.32 ± 13.51 | 63.14 ± 12.3 | 0.338 |
| Sex, male:female | 54:46 | 49:74 | 0.035* |
| Levels (n = 263) | 112 | 151 | 0.059 |
| 1 | 90 | 96 | 0.017* |
| 2 | 8 | 26 | 0.006* |
| 3 | 2 | 1 | 0.446 |
| The degree of decompression | |||
| Unilateral:bilateral | 51:61 | 54:97 | 0.293 |
| Discectomy | 21 | 20 | 0.366 |
| Severity of stenosis | |||
| Mild | 10 | 11 | 0.487 |
| Moderate | 81 | 122 | 0.080 |
| Severe | 21 | 18 | 0.124 |
Table 2.
perioperative and postoperative comparison of surgical outcome
| Variable | Group 1 (n = 100) | Group 2 (n = 123) | p-value |
|---|---|---|---|
| Surgery time (min/level) | 105.26 ± 30.49 | 67.65 ± 18.83 | 0.001* |
| Hospital stay (day) | 5.49 ± 6.52 | 5.37 ± 5.09 | 0.882 |
| Perioperative complication | 16 (16) | 8 (8.3) | 0.023* |
| Dura tear | 4 | 1 | |
| Motor weakness | 2 | 2 | |
| Dysthesia | 3 | 2 | |
| Postoperative hematoma | 2 | 1 | |
| Excessive facet resection | 5 | 2 |
REFERENCES
1. Kambin P, Brager MD. Percutaneous posterolateral discectomy. Anatomy and mechanism. Clin Orthop Relat Res 1987 (223):145-54.

2. Yeung AT, Tsou PM. Posterolateral endoscopic excision for lumbar disc herniation: Surgical technique, outcome, and complications in 307 consecutive cases. Spine (Phila Pa 1976) 2002 27:722-31.


3. Hijikata S. Percutaneous nucleotomy. A new concept technique and 12 years' experience. Clin Orthop Relat Res 1989 (238):9-23.

4. Phan K, Xu J, Schultz K, et al. Full-endoscopic versus microendoscopic and open discectomy: a systematic review and meta-analysis of outcomes and complications. Clin Neurol Neurosurg 2017 154:1-12.


5. Akçakaya MO, Yörükoğlu AG, Aydoseli A, et al. Serum creatine phosphokinase levels as an indicator of muscle injury following lumbar disc surgery: comparison of fully endoscopic discectomy and microdiscectomy. Clin Neurol Neurosurg 2016 145:74-8.


6. Cong L, Zhu Y, Tu G. A meta-analysis of endoscopic discectomy versus open discectomy for symptomatic lumbar disk herniation. Eur Spine J 2016 25:134-43.


7. Belykh E, Giers MB, Preul MC, et al. Prospective comparison of microsurgical, tubular-based endoscopic, and endoscopically assisted diskectomies: clinical effectiveness and complications in railway workers. World Neurosurg 2016 90:273-80.


8. Komp M, Hahn P, Oezdemir S, et al. Bilateral spinal decompression of lumbar central stenosis with the full-endoscopic interlaminar versus microsurgical laminotomy technique: a prospective, randomized, controlled study. Pain Physician 2015 18:61-70.


9. Lee CW, Yoon KJ, Ha SS, et al. Foraminoplastic superior vertebral notch approach with reamers in percutaneous endoscopic lumbar discectomy: technical note and clinical outcome in limited indications of percutaneous endoscopic lumbar discectomy. J Korean Neurosurg Soc 2016 59:172-81.




10. Akbary K, Kim JS, Park CW, et al. Biportal endoscopic decompression of exiting and traversing nerve roots through a single interlaminar window using a contralateral approach: technical feasibilities and morphometric changes of the lumbar canal and foramen. World Neurosurg 2018 117:153-61.


11. Lee SH, Kang HS, Choi G, et al. Foraminoplastic ventral epidural approach for removal of extruded herniated fragment at the L5-S1 level. Neurol Med Chir (Tokyo) 2010 50:1074-8.


12. Kim HS, Ju CI, Kim SW, et al. Endoscopic transforaminal suprapedicular approach in high grade inferior migrated lumbar disc herniation. J Korean Neurosurg Soc 2009 45:67-73.




13. Choi KC, Lee DC, Shim HK, et al. A strategy of percutaneous endoscopic lumbar discectomy for migrated disc herniation. World Neurosurg 2017 99:259-66.


14. Lee CH, Choi M, Ryu DS, et al. Efficacy and safety of fullendoscopic decompression via interlaminar approach for central or lateral recess spinal stenosis of the lumbar spine: a meta-analysis. Spine (Phila Pa 1976) 2018 43:1756-64.


15. Lee CW, Yoon KJ, Jun JH. Percutaneous endoscopic laminotomy with flavectomy by uniportal, unilateral approach for the lumbar canal or lateral recess stenosis. World Neurosurg 2018 113:e129-37.


16. Kim HS, Paudel B, Jang JS, et al. Percutaneous full endoscopic bilateral lumbar decompression of spinal stenosis through uniportal-contralateral approach: techniques and preliminary results. World Neurosurg 2017 103:201-9.


17. Hwang JH, Park WM, Park CW. Contralateral interlaminar keyhole percutaneous endoscopic lumbar surgery in patients with unilateral radiculopathy. World Neurosurg 2017 101:33-41.


18. Ahn Y. Transforaminal percutaneous endoscopic lumbar discectomy: technical tips to prevent complications. Expert Rev Med Devices 2012 9:361-6.


19. Ahn Y, Lee HY, Lee SH, et al. Dural tears in percutaneous endoscopic lumbar discectomy. Eur Spine J 2011 20:58-64.



20. Sairyo K, Sakai T, Higashino K, et al. Complications of endoscopic lumbar decompression surgery. Minim Invasive Neurosurg 2010 53:175-8.



21. Lee DY, Lee SH. Learning curve for percutaneous endoscopic lumbar discectomy. Neurol Med Chir (Tokyo) 2008 48:383-8.


22. Palmer S, Turner R, Palmer R. Bilateral decompression of lumbar spinal stenosis involving a unilateral approach with microscope and tubular retractor system. J Neurosurg 2002 97(2 Suppl):213-7.


23. Kim K, Isu T, Sugawara A, et al. Comparison of the effect of 3 different approaches to the lumbar spinal canal on postoperative paraspinal muscle damage. Surg Neurol 2008 69:109-13.


24. Ahn J, Iqbal A, Manning BT, et al. Minimally invasive lumbar decompression-the surgical learning curve. Spine J 2016 16:909-16.


25. Arts M, Brand R, van der Kallen B, et al. Does minimally invasive lumbar disc surgery result in less muscle injury than conventional surgery? A randomized controlled trial. Eur Spine J 2011 20:51-7.


26. Hong SW, Choi KY, Ahn Y, et al. A comparison of unilateral and bilateral laminotomies for decompression of L4-L5 spinal stenosis. Spine (Phila Pa 1976) 2011 36:E172-8.


27. Wang B, Lü G, Patel AA, et al. An evaluation of the learning curve for a complex surgical technique: the full endoscopic interlaminar approach for lumbar disc herniations. Spine J 2011 11:122-30.


28. Haddadi K, Ganjeh Qazvini HR. Outcome after surgery of lumbar spinal stenosis: a randomized comparison of bilateral laminotomy, trumpet laminectomy, and conventional laminectomy. Front Surg 2016 3:19.



29. Rahman M, Summers LE, Richter B, et al. Comparison of techniques for decompressive lumbar laminectomy: the minimally invasive versus the “classic” open approach. Minim Invasive Neurosurg 2008 51:100-5.



30. Oertel MF, Ryang YM, Korinth MC, et al. Long-term results of microsurgical treatment of lumbar spinal stenosis by unilateral laminotomy for bilateral decompression. Neurosurgery 2006 59:1264-9.



31. Overdevest G, Vleggeert-Lankamp C, Jacobs W, et al. Effectiveness of posterior decompression techniques compared with conventional laminectomy for lumbar stenosis. Eur Spine J 2015 24:2244-63.


32. Storzer B, Schnake KJ. Microscopic bilateral decompression by unilateral approach in spinal stenosis. Eur Spine J 2016 25 Suppl 2:270-1.



33. Hatta Y, Shiraishi T, Sakamoto A, et al. Muscle-preserving interlaminar decompression for the lumbar spine: a minimally invasive new procedure for lumbar spinal canal stenosis. Spine (Phila Pa 1976) 2009 34:E276-80.


34. Phan K, Mobbs RJ. Minimally Invasive versus open laminectomy for lumbar stenosis: a systematic review and metaanalysis. Spine (Phila Pa 1976) 2016 41:E91-100.


35. Williams BJ, Sansur CA, Smith JS, et al. Incidence of unintended durotomy in spine surgery based on 108,478 cases. Neurosurgery 2011 68:117-23.




- TOOLS
- Related articles in NS
-
Journal Impact Factor 3.2



























