I, Kiyoshi Hirabayashi, devised the original expansive laminoplasty (ELAP) procedure for cervical myelopathy in 1977 [1]. Since then, the technique has been an indispensable tool in the treatment of cervical myelopathy, both in Japan and around the world. I would like to take this opportunity to describe the evolution of ELAP for the readers of this journal.
GENESIS OF THE IDEA FOR ELAP
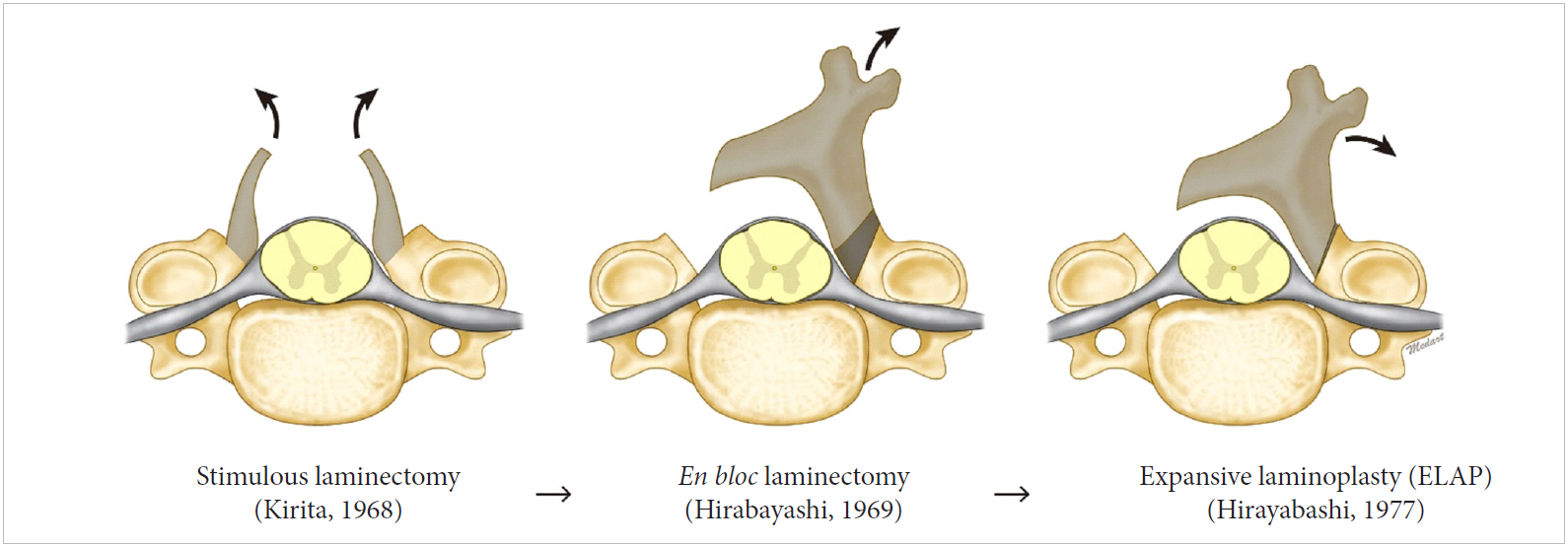
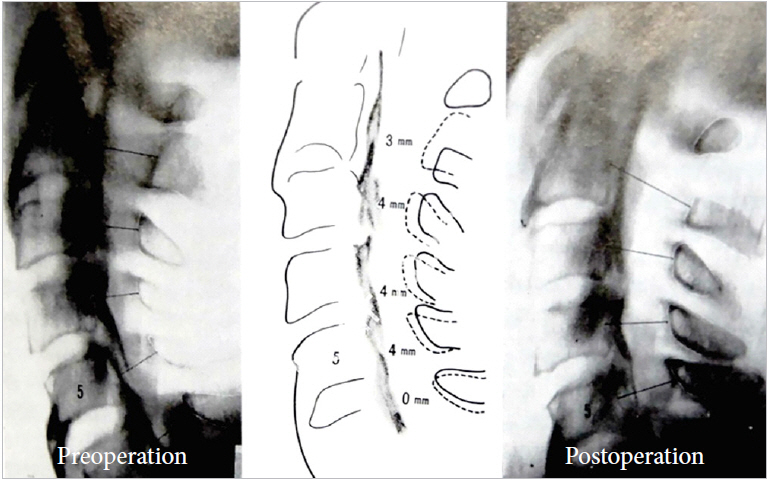
In 1968, extensive laminectomy with simultaneous middorsal division of the lamina was developed by Kirita et al. [2] to replace conventional laminectomy as a decompression technique for cervical stenotic myelopathy. Being safe and effective, the technique markedly improved the surgical treatment of cervical spinal stenotic myelopathy. One day, I was performing decompression surgery using a modification of Kirita’s method. Bilateral bony gutters were made with a high-speed drill at the junction of the laminae and facet joints to remove the laminae in an en bloc manner; then, upon lifting one side of the lamina before its complete removal, I noticed the presence of dural pulsation. The appreciation of dural pulsation was serendipitous in that it gave me the idea of open-door laminoplasty (Fig. 1). Later, instead of conventional laminectomy, I performed the first case of open-door laminoplasty in a patient with ossification of the posterior longitudinal ligament in 1977 and named the technique “expansive laminoplasty” (Fig. 2). In 1982, I described the first series of patients treated using ELAP in the English-language literature [3], with encouraging results.
At that time, the common complications of conventional laminectomy included postoperative kyphosis, caused by vulnerability of the cervical spine, and canal stenosis, caused by the formation of a postoperative scar known as the “laminectomy membrane.” In addition, I experienced cases of postoperative recurrence of radiculomyelopathy, caused by mild neck injury in patients who had undergone conventional cervical laminectomy. These complications may have resulted from postoperative structural weakness in the cervical spine after laminectomy. These postoperative problems in patients who underwent laminectomy also motivated me to refer to the idea of ELAP as serendipitous.
MODIFICATIONS OF THE TECHNIQUE
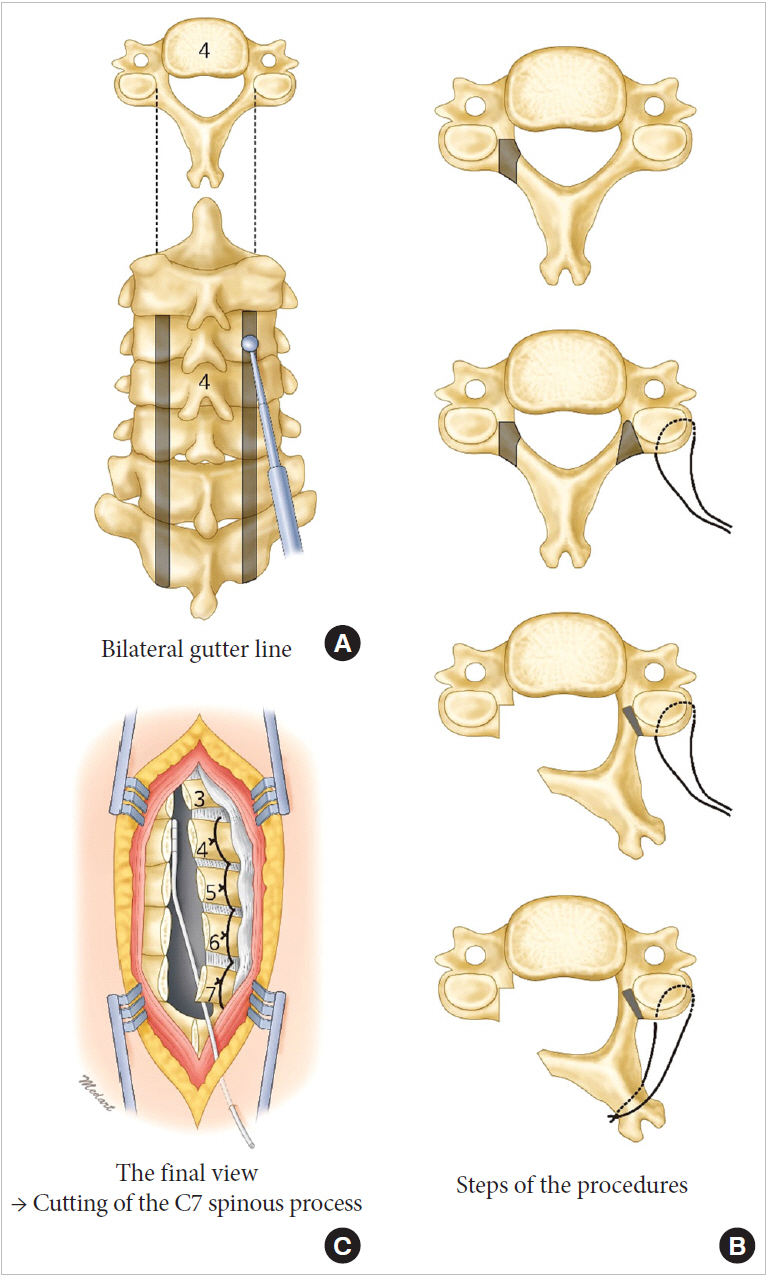
Since the first development of ELAP, I have continued to modify the technique, as follows (Fig. 3):
(1) To prevent lamina closure, I placed anchor sutures around the base of the spinous processes [3]. This modification prevented the recurrence of myelopathy, which requires salvage surgery, including laminectomy.
(2) Because I initially made the gutters on both sides with a cutting bur and then resected the ventral cortex on the open side with a Kerrison rongeur, the ventral cortex on the hinge side sometimes broke during the excision. I changed the sequence of the procedures, making the gutter on the hinge side with the cutting bur after completing all other procedures, including resection of the ventral cortex on the open side and resection of the cephalad and caudal ends of the laminar doors.
(3) Maintaining the lordotic spinal curvature is especially important in patients who require extensive laminoplasty because the more lordotic the spine is, the more dorsal the spinal cord shifts. To maintain and reinforce cervical lordosis, I revised the intraoperative position of the neck from a flexed position to a neutral position just before opening the laminae and completing subsequent procedures. However, to date, creation of physiological lordosis has not been achieved in patients with preoperatively established kyphosis, although preoperative alignment has been maintained or slight correction has been possible to a certain degree.
OVERCOMING THE RELATED COMPLICATIONS
Motor weakness in the C5 or C6 segment is the most notorious complication of ELAP, with a reported incidence between 5% and 10% [4]. The cause of this complication has not yet been elucidated, but it may result from trauma during surgery, rather than a tethering effect on the nerve root; supporting this possibility, the incidence decreased dramatically when air-driven drilling with cooling by cold water was used and when the Kerrison rongeur was handled gently. Nonetheless, motor weakness resulting from the tethering effect on the nerve roots still cannot be prevented, but spontaneous recovery can be expected in most cases within 2 years after surgery. Approximately one-third of patients complained of postoperative axial symptoms, such as stiffness and pain in the shoulder and neck. However, fewer than 10% were taking anti-inflammatory drugs daily to alleviate such symptoms.
Furthermore, approximately one-third of patients complained of a restricted range of motion, mainly difficulty in flexing and rotating their necks, in turning their heads back, and in looking down at their toes. The majority of those patients had minor disturbances in their activities of daily living because of compensation by upper cervical motion. A decrease in range of motion as a result of fusion or contracture at the hinge may help stabilize the spine, which would result in rather favorable long-term results, especially regarding the prevention of recurrent radiculomyelopathy.
INFLUENCE OF PEOPLE AND PROCEDURES ON THE TECHNIQUE
In 1968, Kirita devised a sophisticated technique in which a high-speed drill was used to thin the laminae and divide them at the midline, followed by their en bloc resection on both sides individually; this technique achieved simultaneous total decompression of the compressed spinal cord. It made conventional (piece by piece) laminectomy much safer, and the incidence of neurological complications was significantly reduced. However, the unprotected spinal cord remained vulnerable and radiculomyelopathy recurred, either because of the development of postoperative kyphosis or because of laminectomy membrane formation.
In 1973, Hattori et al. devised an expansive laminoplasty involving Z-plasty of the laminae (Fig. 4). This technique enabled reconstruction of the complete cervical spinal canal except the spinous processes. However, the procedure did not come into widespread use because it required highly meticulous skill and was time-consuming. Since 1977, when the original ELAP was devised, the open-door technique itself also has undergone a variety of modifications by many surgeons throughout the world, including the use of bone grafts [5], spacers [6], plates [7], and other instruments [8], to address problems of reclosure or an established kyphotic deformity (Fig. 4). With regard to postoperative cervical stability, simple ELAP seems to be a rational indication for the majority of cases of typical cervical stenotic myelopathy. The other expansive laminoplasties in which bone grafting, spacers, or plates are used may be indicated in patients with high degree of instability, such as patients with cerebral palsy, or in patients at high risk for pushback in the opened laminar door due to well-developed neck muscles, such as young male patients.
I have described the inspiration for the invention of ELAP, how the technique was improved, and how I overcome the downsides of the technique. I hope this description assists in further improvements of laminoplasty and treatments for cervical myelopathy.