 |
 |
- Search
|
|
||
Abstract
Thymoma and thymic carcinoma are rare epithelial tumors that originate from the thymus gland. Extrathoracic metastases occur in the liver, kidney, and bone in 1% to 15% of patients. Although thymoma and thymic carcinoma exhibit highly aggressive biological behavior, spinal metastasis is rare. We describe a 78-year-old man with left wrist and grasp weakness that occurred 7 days before admission. The patient underwent thymoma surgery 7 years ago and was cured. Magnetic resonance images showed a rim-enhanced mass in the C6–7–T1 epidural space. C6–7–T1 laminectomy was performed and the mass was removed. Histological examination was performed and patient was diagnosed with metastatic thymoma. The previous reported case occurred with involvement of the vertebral body or posterior element, but our case was mostly rim-enhanced and appeared as an abscess and intradural extramedullary tumor.
Thymoma and thymic carcinoma is a rare tumor originating from epithelial cells of the thymus. Metastasis occurs mainly in the local site or thoracic cavity2). Spine metastasis was reported in 7 cases3,5,6,8,10,12). These cases were easily distinguished from metastasis by destroying the surrounding vertebral bone. However, our case was uniquely limited to the epidural space and invaded the intervertebral foramen.
A 78-year-old man developed weakness of the left wrist and grasp (grade 2). He experienced pain for 2 days, but there was no pain at admission. The patient was diagnosed with malignant thymic tumor with involvement of the lungs and underwent surgical resection 7 years ago. Histopathologically, malignant thymoma was diagnosed with combined thyroid B2 and B3. Therefore, additional radiotherapy was performed. The tumor did not recur and the patient was cured.
Cervical spine magnetic resonance imaging (MRI) revealed a rim-enhanced lesion compressing the cord into the C6–7–T1 epidural space and invading the C7–T1 intervertebral for a-men. MRI with contrast showed low signal lesions in the vertebral bone of C7 (Fig. 1). A laboratory study was performed at admission. White blood count, erythrocyte sedimentation rate, and C-reactive protein levels were normal.
A nearly total resection preserving nerve roots was performed via a total C6–C7–T1 laminectomy.
Histopathologically, the malignant thymoma that was operated on 7 years ago was composed of lobules separated by fibrous scar, and necrosis was observed in some of them. There were 2 types of tumor lobules: some lobules were mixed with lymphocytes of tumor epithelium, and some lobules were mostly tumor epithelial cells and lymphocytes were rarely observed (Fig. 2). The nuclei of tumor cells were round or ovoid, and the boundaries of cells were unclear. The nucleus was vesicular, indistinct, or distinct. Mitosis was rare. Tumor cells were positive for epithelial cell markers, including cytokeratin and epithelial membrane antigen, and negative for CD5 indicating B2 and B3 type thymoma. The tumor was invading the lungs and no lymph node metastasis was observed. Cervical lesions were accompanied by necrosis or bleeding. Tumor cells mixed with lymphocytes were observed. Tumor nuclei were round or ovoid and nonnodular (Fig. 3). Tumor cells were positive for epithelial cytokeratin and positive for PAX8, a thymic epithelial cell marker, and a patient was diagnosed with recurrent (metastatic) malignant thymoma.
We explained to the patient and patient’s family about the patient’s systemic condition and side effects of radiotherapy and chemotherapy. However, the patient and his family refused further treatment.
Thymoma and thymic carcinoma are uncommon epithelial lesions that originate from the thymus gland2). The incidence of thymomas has been estimated at 0.13 per 100,000 person in a year1). On the basis of the appearance of epithelial cells, the World Health Organization unified classification proposed 3 histological types of thymomas (types A, B, and C), and 5 classes (medullary, mixed, lymphocytic, cortical, and epithelial)13). Moran and Suster9) differentiated thymomas according to atypia of the neoplastic epithelial cells (type A–B2, well differentiated thymomas; type B3, atypical thymoma; type C, thymic carcinoma). Although thymic carcinomas are classified as type C in the World Health Organization classification, these tumors are not just another variant of thymoma.
In 6 cases reported previously, extradural lesions that were close to the spinal canal in MRI were compressing the dura mater and invading the paravertebral muscles3,5,6,8,10,12). In 1 case, intradural extramedullary metastasis was present after surgical treatment with extradural mass. After gadolinium administration, tumors showed strong enhancement. In computed tomography (CT) study, infiltrated vertebral bodies can show both as osteoplastic and osteolytic lesions. Our case was different from the case reported previously. MRI showed that the tumor was rim-enhanced, and CT showed that the tumor was not invading the vertebral body (Table 1).
Local spreading occurs rapidly in thymoma but distant metastasis occurs late. The distant spinal metastasis of thymoma requires an average of 11 years (4 to 17 years)8). Our case also developed distant metastasis after 7 years.
The 5-year survival rate of patients with distant metastasis of thymoma varied widely between 13.3% and 81% after multimodality treatment, including surgical resection of primary tumor, pleurectomy, chemotherapy, and irradiation14). However, surgical resection is the most important treatment for thymoma metastasis. In recurrent thymoma, reoperation is more effective at increasing the 5-year survival rate than radiation and chemotherapy7). The reoperation is aggressively recommended if it is possible to resect the lesion completely. Overall 5-year survival rates of the recurrence cases without reoperation were 36% and 51%, respectively, whereas the 5-year survival rates of the recurrence cases with reoperation were 47% and 64%, respectively. Also, overall 10-year survival rates of the recurrence cases without reoperation were 17 % and 43%, respectively, whereas the 10-year survival rates of the recurrence cases with reoperation were 35% and 53%, respectively4,11). In metastatic thymoma, surgical treatment is also more important than other treatments.
Spinal metastasis of thymoma is rare and occurs a few years later. The previous reported case occurred with involvement of the vertebral body or posterior element, but our case was purely rim-enhanced and appeared as an abscess and intradural extramedullary tumor. In addition, if there is a spinal epidural lesion, distant metastasis due to underlying disease should be considered.
CONFLICT OF INTEREST
CONFLICT OF INTEREST
No potential conflict of interest relevant to this article was reported.
Fig. 1
Magnetic resonance imaging with contrast of the cervical spine in sagittal (A), coronal (B), and axial (C) planes shows a rim enhancement lesion in left C6-C7-T1 epidural space and low signal lesions in the vertebral bone of C7. Plane radiography in anteroposterior (D), lateral (E) views.
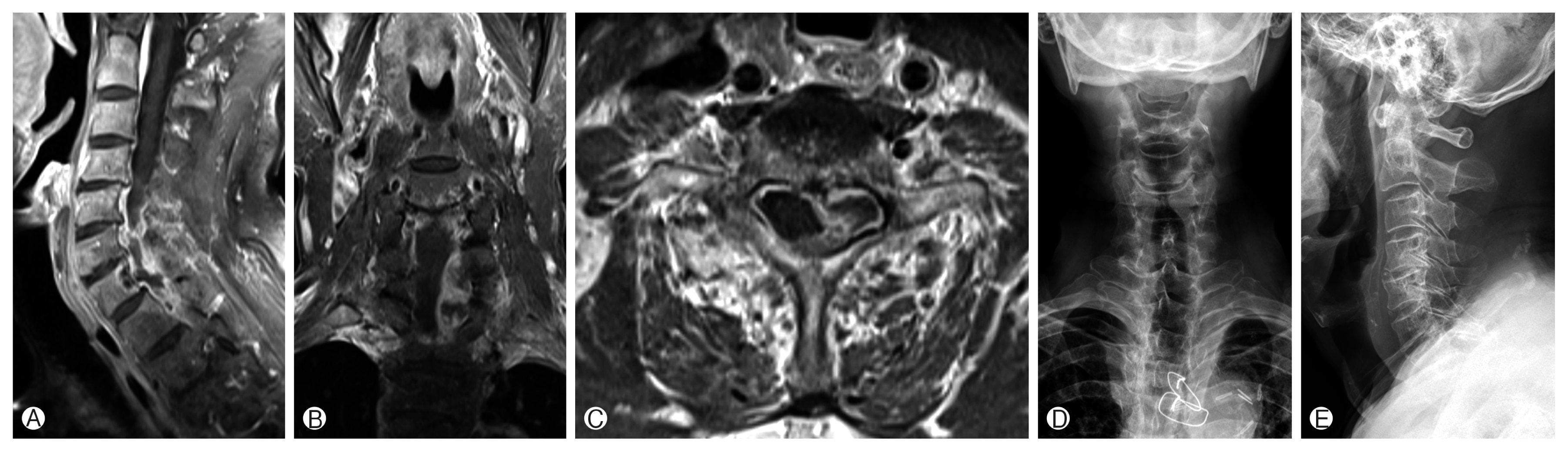
Fig. 2
Malignant thymoma. (A) The tumor shows 2 different components which are separated by fibrous septa (H&E, ×100). (B) The left darker side shows cytokeratin positive epithelial cells admixed with lymphocytes (B2) and the right paler side shows predominant epithelial cells (B3) (cytokeratin, ×100). (C) The nucleus of tumor cells (B3) are variable sized and vesicular and some nuclei show prominent nucleoli (H&E, ×400).
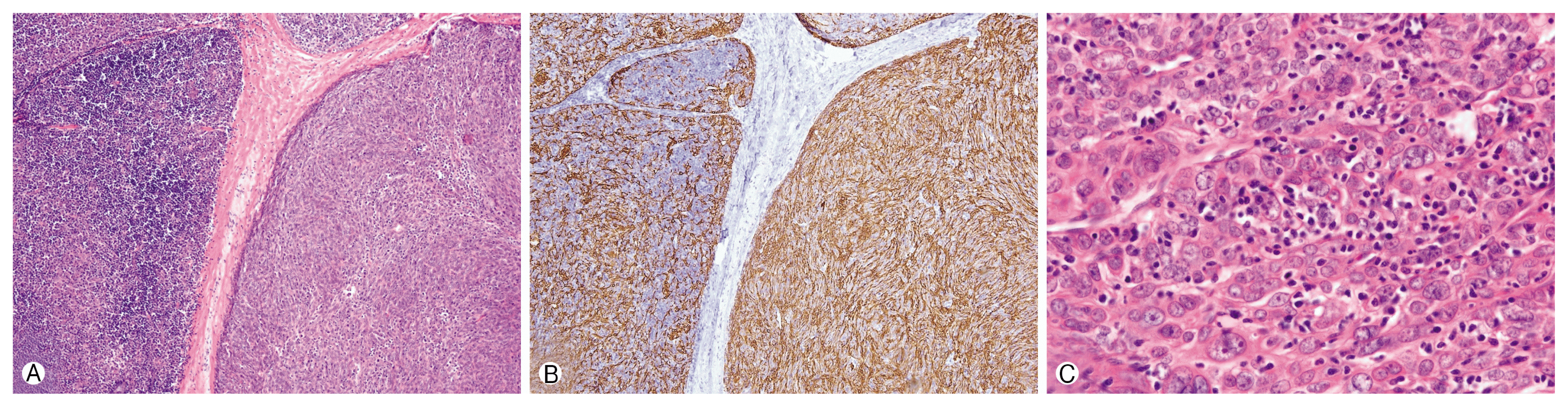
Fig. 3
Metastatic thymoma. (A) The tumor shows sheets of round cells in the background of inflammatory cells (H&E, ×200). The tumor cells are positive for cytokeratin (B, ×200) PAX8 (C, ×200).

Table 1
Literature review of distant spinal metastasis of thymomas
| Study | Age (yr) | Sex | Primary tumor | Time to spinal metastasis (yr) | Symptoms | Location of spinal Metastasis | Surgical procedures | Outcomes |
|---|---|---|---|---|---|---|---|---|
| Farin et al.3) | 45 | Male | Thymoma | 12 | Progressive back pain, sensory disturbance in toe, myasthenia gravis | T11–12, epidural, infiltration of vertebral body, pedicle, paraspinal muscles | Tumor resection via laminectomy T11–12, partial corpectomy interbody fusion | Disease free at 9-month follow-up |
| Toba et al.12) | 29 | Female | Thymoma | 4 | Back pain, myasthenia gravis | T10–11, intervertebral foramen | Tumor resection with resection the head of the 10th and 11th rib | Ne recurrence for 15 months |
| Liu et al.6) | 57 | Male | Thymic carcinoma | Spinal metastasis was diagnosed before primary tumor | Paraparesis | C4–T1, vertebral body, paraspinal muscles | Spinal cord decompression via laminectomy C5–7, posterior fixation C3–7 | Died 5 months later |
| Nagel et al.10) | 67 | Male | Carcinoid tumor of the thymus | 16 | Monoparesis of leg | T3, T9, L5, epidural, vertebral body, paraspinal muscles | Tuomr resection via laminectomies T2–3, T8–9, and L4–5 | Died 1 year later |
| Hong et al.5) | 42 | Female | Thymoma | 8 | Back pain | L4–S1, epidural | L4, L5 hemilaminectomy | Disease free at 9-month follow-up |
| Hong et al.5) | 62 | Female | Thymic carcinoma | 13 | Segmental back pain | T9–10, epidural | Costotransversectomy and facetectomy T9–10 | Died 2 years later |
| Marotta et al.8) | 46 | Male | Thymoma | Not reported | ||||
| Present case | 78 | Female | Thymic carcinoma | 7 | Left wrist, grasping power decrease | C6–C7–T1, Epidural, intervertebral foramen | Laminoplasty C6–7–T1 and tumor resection | Disease free at 6-month follow-up |
REFERENCES
1. Engels EA. Epidemiology of thymoma and associated malignancies. J Thorac Oncol 5(10 Suppl 4):S260-265. 2010.



2. Engels EA, Pfeiffer RM. Malignant thymoma in the United States: demographic patterns in incidence and associations with subsequent malignancies. Int J Cancer 105:546-551. 2003.


3. Farin A, Aryan HE, Abshire B. Thymoma metastatic to the extradural spine. J Clin Neurosci 12:824-827. 2005.


4. Haniuda M, Kondo R, Numanami H, Makiuchi A, Machida E, Amano J. Recurrence of thymoma: clinicopathological features, re-operation, and outcome. J Surg Oncol 78:183-188. 2001.


5. Hong B, Nakamura M, Hartmann C, Brandis A, Ganser A, Krauss JK. Delayed distant spinal metastasis in thymomas. Spine (Phila Pa 1976) 38:E1709-1713. 2013.


6. Liu T, Qiu G, Tian Y. Thymic carcinoma with primary spine metastasis. J Clin Neurosci 18:840-842. 2011.


7. Maggi G, Casadio C, Cavallo A, Cianci R, Molinatti M, Ruffini E. Thymoma: results of 241 operated cases. Ann Thorac Surg 51:152-156. 1991.


8. Marotta N, Mancarella C, Colistra D, Landi A, Dugoni DE, Delfini R. First description of cervical intradural thymoma metastasis. World J Clin Cases 3:946-950. 2015.



9. Moran CA, Suster S. Thymic carcinoma: current concepts and histologic features. Hematol Oncol Clin North Am 22:393-407. 2008.


10. Nagel SJ, Hughes G, Ugokwe KT, Prayson RA, Krishnaney AA. Spinal carcinoid metastasis with dural invasion. World Neurosurg 76:478.e7-478.e11. 2011.


11. Regnard JF, Zinzindohoue F, Magdeleinat P, Guibert L, Spaggiari L, Levasseur P. Results of re-resection for recurrent thymomas. Ann Thorac Surg 64:1593-1598. 1997.


12. Toba H, Kondo K, Takizawa H, Tangoku A. Recurrent thymoma with a pleural dissemination invading the intervertebral foramen. Eur J Cardiothorac Surg 35:917-919. 2009.




- TOOLS
-
METRICS

-
- 4 Crossref
- Scopus
- 6,901 View
- 173 Download

























